
March 2022: Periods are different from person to person and can change month to month. It is normal to experience small changes in your period—being shorter or longer in length, having heavier or lighter bleeding, or experiencing new or different symptoms. Periods change for many reasons, including stress, medication, and age.
However, changes to your period that last several months or are very different than your typical period can be a sign that something may not be normal. Here are signs of abnormal menstrual cycles1,2 that may need to be evaluated by a health care provider:
- Your period lasts more than ten days.
- Your period flows so heavily that it impacts your daily routine.
- The time between your periods is less than 24 days or more than 38 days.
- You don’t get a period.
- You spot or bleed frequently in between periods.
Periods are a window into overall health. Survey data from the Apple Women’s Health Study helps us understand the relationship between persistent abnormal periods, polycystic ovarian syndrome (PCOS), and heart health.
Data analysis
Participants contributing data to this study update were those who enrolled from the start of the study in November 2019 through December 2021. Our study’s enrollment is ongoing, meaning people can join at any time and surveys are sent out at different times.
More than 37,000 participants completed the Medical History survey at least once and answered questions about gynecological conditions, family medical history, and heart health. Of the participants that completed the Medical History survey, approximately 30,000 also completed the Reproductive History survey and answered questions about their menstrual cycle over time.
Thanks to survey data shared by participants, we are excited to share preliminary insights.
Insights on polycystic ovarian syndrome (PCOS)
Long menstrual cycles and heavy periods3 can be symptoms of a condition called “polycystic ovarian syndrome”, “polycystic ovary syndrome”, or “PCOS”. People with PCOS can have higher levels of androgen hormones. This hormonal imbalance can cause acne, excess facial or body hair, or scalp hair loss.
Fluid-filled sacs called “follicles” develop on the ovary during a normal menstrual cycle. These follicles can develop into cysts. People with PCOS may have too many follicles or cysts on their ovaries, which can interfere with normal ovulation.
Health care providers diagnose PCOS by listening to a patient’s description of their menstrual cycles and symptoms, examining a patient for physical symptoms, measuring hormone levels through a blood test, and conducting an imaging test of the ovaries and uterus. Since there are other health conditions that cause similar symptoms, health care providers examine and evaluate patients for other diseases4,5. In our study, 12% of participants reported a diagnosis of PCOS.
12%
Reported a PCOS diagnosis
The prevalence of self-reported PCOS among participants in our study is comparable to other scientific studies. Other studies estimate that PCOS impacts 4-20% of women worldwide of reproductive age6. People are typically diagnosed with PCOS in their 20s or 30s7; however, PCOS may be diagnosed as early as adolescence. Most of the participants in our study that have PCOS were diagnosed between the ages of 14 and 35, with a median age of 22 years old.
22 years old
Median age when diagnosed with PCOS
People may not always be aware that their abnormal menstrual cycle is a reason to talk to a health care provider, and PCOS symptoms may develop slowly over time. It typically takes a few years and several appointments with health care providers from the time when a person first has symptoms to receiving a confirmed diagnosis of PCOS8,9. While our study looks at participants who reported a PCOS diagnosis, there may be participants who have abnormal menstrual cycles or PCOS that are not aware or have not had a formal diagnosis.
The causes of PCOS are still not fully clear, but research has identified factors that elevate risk. One of these factors is family history, meaning that if a person’s mother or sister has PCOS, it is more likely that they could have PCOS. One study10 found that among patients with PCOS, 24% of their mothers and 32% of their sisters had also been diagnosed with PCOS.
In our study, participants with PCOS were more likely to report a family history of PCOS. Out of the participants with PCOS, 23% had a family history of PCOS. In comparison, only 5% of participants without PCOS had a family history of PCOS.
23%
Participants with PCOS also had family history of PCOS
We asked participants how long it took for their menstrual cycle to become regular after getting their first period, or menarche. We also asked about their history of hormone use. Medications, such as birth control or pills containing hormones, are typically prescribed to patients when appropriate to help regularize their menstrual cycles11.
Preliminary analysis of study data shows that in comparison to participants without PCOS, participants with PCOS were more likely to have unpredictable or irregular menstrual cycles after menarche.
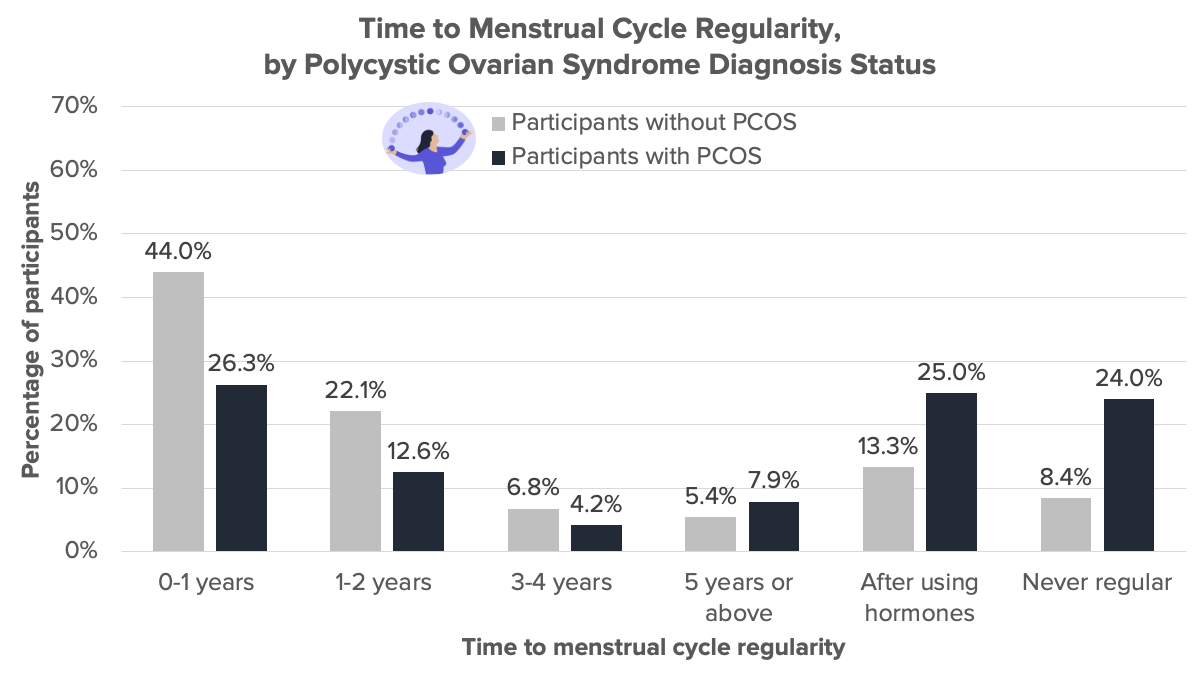
More than 70% of participants without PCOS reported that their menstrual cycles became regular within four years of their first period. In comparison, only 43% of participants with PCOS reported that their cycles become regular during the same time frame.
Almost half, 49%, of the participants that reported a diagnosis of PCOS never had regular menstrual cycles or achieved regularity only after using hormones. In comparison, only 22% of participants without a diagnosis of PCOS never had regular menstrual cycles or achieved regularity using hormones.
Heart health and PCOS
While we often think about PCOS as impacting periods and menstruation, it is also closely linked to heart and circulatory health. PCOS may increase the risk of diabetes, high blood pressure, high cholesterol, obesity, and cardiovascular disease12-15.
The heart moves hormones, oxygen, nutrients, and immune cells through the blood stream to power many organ systems16. Heart disease is the leading cause of death in the US17, and many people have a condition that impacts their heart health.
Preliminary analysis of study data suggests that Apple Women’s Health Study participants with PCOS have a higher prevalence of conditions that can negatively impact heart health.
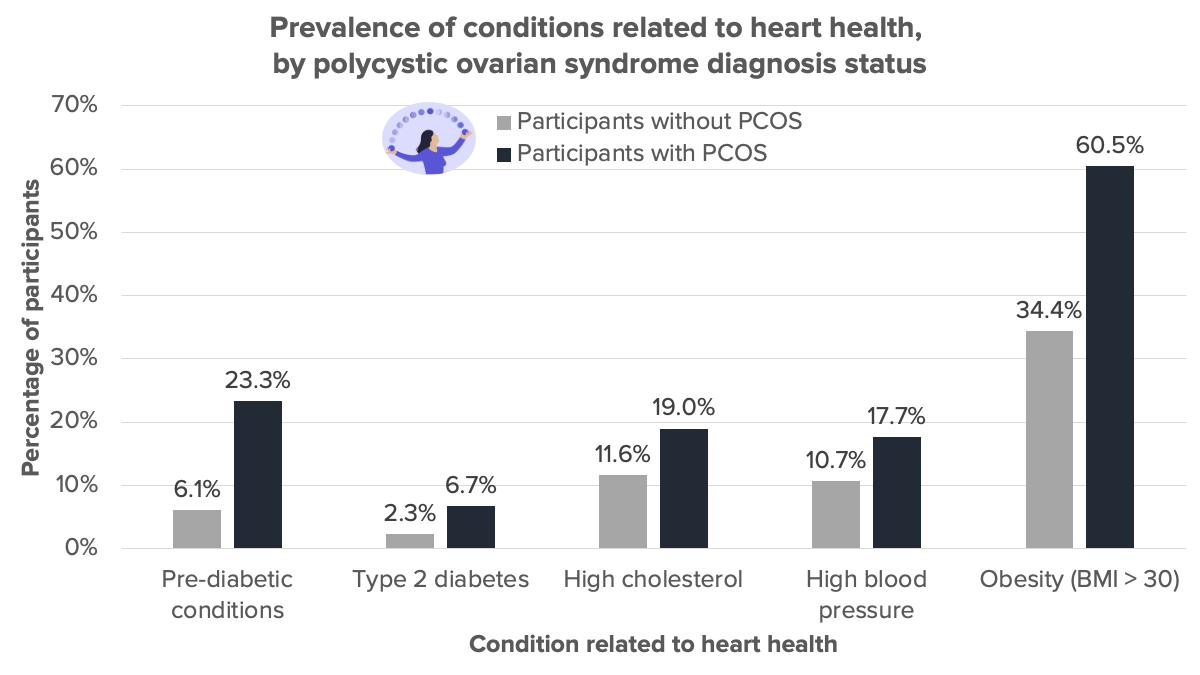
In comparison to participants without PCOS, participants with PCOS were almost four times more likely to have pre-diabetic conditions and three times more likely to have Type 2 diabetes. In people with diabetes, chronic elevations in glucose may damage blood vessels in the heart.
The prevalence of high blood pressure and high cholesterol were 1.7 times higher for participants with PCOS than participants without PCOS. High blood pressure is when blood flows with too much force, and this can damage the walls of arteries over time. Too much bad cholesterol can clog or block arteries, preventing the flow of blood.
A majority, 61%, of participants with PCOS reported obesity, defined by a Body Mass Index (BMI) of more than 30 kg/m2. Prevalence of obesity was almost double for participants with PCOS than participants without PCOS. Obesity can impact cholesterol levels, affect blood pressure, and increase risk of conditions like diabetes18.
Irregular heartbeat, or arrhythmia, was more common among participants with PCOS (5.6%) than participants without PCOS (3.7%). Of the participants that did not report a PCOS diagnosis but reported family history of PCOS, 6.2% had arrhythmia.
Further analysis is needed to understand the relationship between menstruation and other cardiovascular diseases and conditions.
Study data contributes to scientific discovery
Our preliminary analyses showed that in comparison to participants without PCOS, participants with PCOS were more likely to have a family history of PCOS, have abnormal menstrual cycles, and have a higher prevalence of conditions that can negatively impact heart health. These conditions include pre-diabetic conditions, Type 2 diabetes, high cholesterol, high blood pressure, and obesity.
The survey responses provided by Apple Women’s Health Study participants allowed us to make discoveries about abnormal periods, PCOS, and heart health. We would like to encourage participants to continue filling out monthly surveys, as this will help us conduct further analyses to better understand the relationship between menstruation and heart health. Not only will we evaluate survey data, but we will also look at tracked menstrual cycle data and sensor data.
Participants can track and share menstrual cycle data with the Apple Women’s Health Study. While this data provides important information about menstrual health at a population-level, menstrual cycle tracking is an even more important tool for personal health management. It can help you track whether your period is abnormal and should be evaluated by a health care provider.
Receiving a diagnosis of PCOS or a heart condition can be difficult, but it does not define you. A diagnosis can help you and your health care provider determine treatment plans so that you can become healthier and feel better. They might recommend that you live a healthy lifestyle to support your menstrual health and reduce your risk of heart-related conditions19. You can improve your overall health by:
- Exercising
- Eating a nutritious, balanced diet
- Getting restful sleep
- Staying hydrated
- Taking care of your mental health
Features on your iPhone and/or Apple Watch can help you manage parts of personal health. The Health app is a centralized location where you can record menstrual cycle data and view other health data, such as step count and amount of time you sleep. Sensor data provide valuable insights to the Apple Women’s Health Study, as it helps us understand lifestyle factors that impact gynecological health. If you are enrolled in this study, you can share sensor data with the research team.
By analyzing the data shared by participants, our goal is to generate knowledge on menstrual health. We hope our research can lead to new strategies to reduce disease risk and improve health across the lifespan. The study team would like to thank participants for your continued participation and helping to advance scientific discovery.



You must be logged in to post a comment.