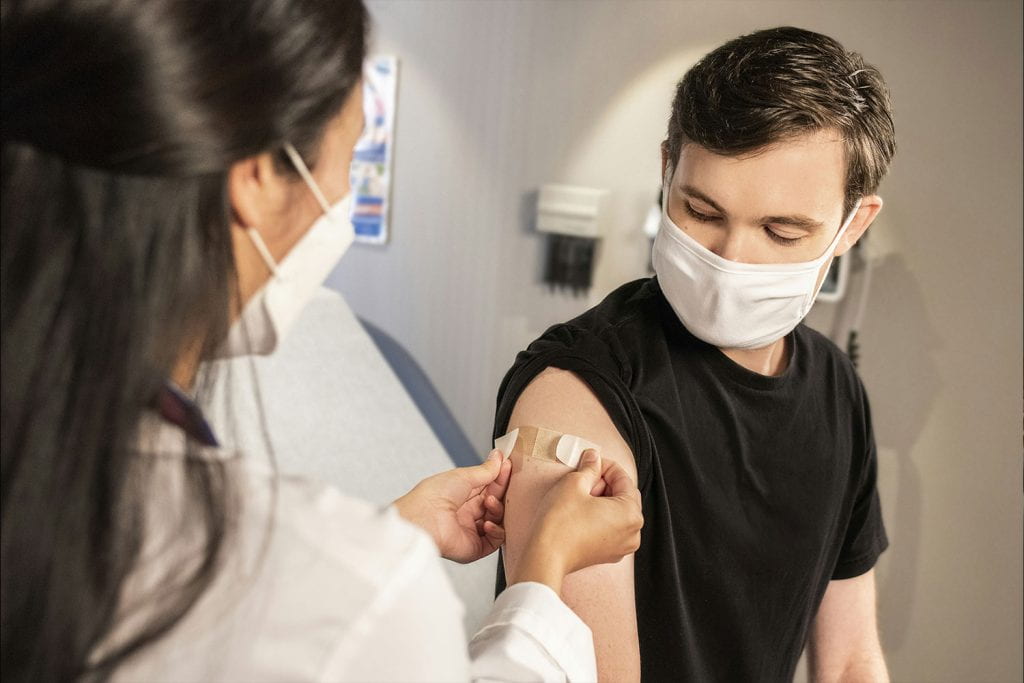
COVID-19 Information
Respiratory illnesses including flu, COVID-19, and RSV impact millions each year. Protect yourself and others by wearing a high-quality face mask in crowded indoor settings; remaining at home if unwell; and staying up to date on vaccines.
COVID-19 Information Links
HUHS Locations

Harvard Square Clinic
location_on
Smith Campus Center
75 Mount Auburn Street
Cambridge, MA 02138
call
Emergency: Dial 911
Office: (617) 495-5711

Law School Clinic
location_on
Pound Hall
1563 Massachusetts Avenue
Cambridge, MA 02138
call
Emergency: Dial 911
Office: (617) 495-4414

Medical Area Clinic
location_on
Vanderbilt Hall
275 Longwood Avenue
Boston, MA 02115
call
Emergency: Dial 911
Office: (617) 432-1370