Department of Global Health and Population
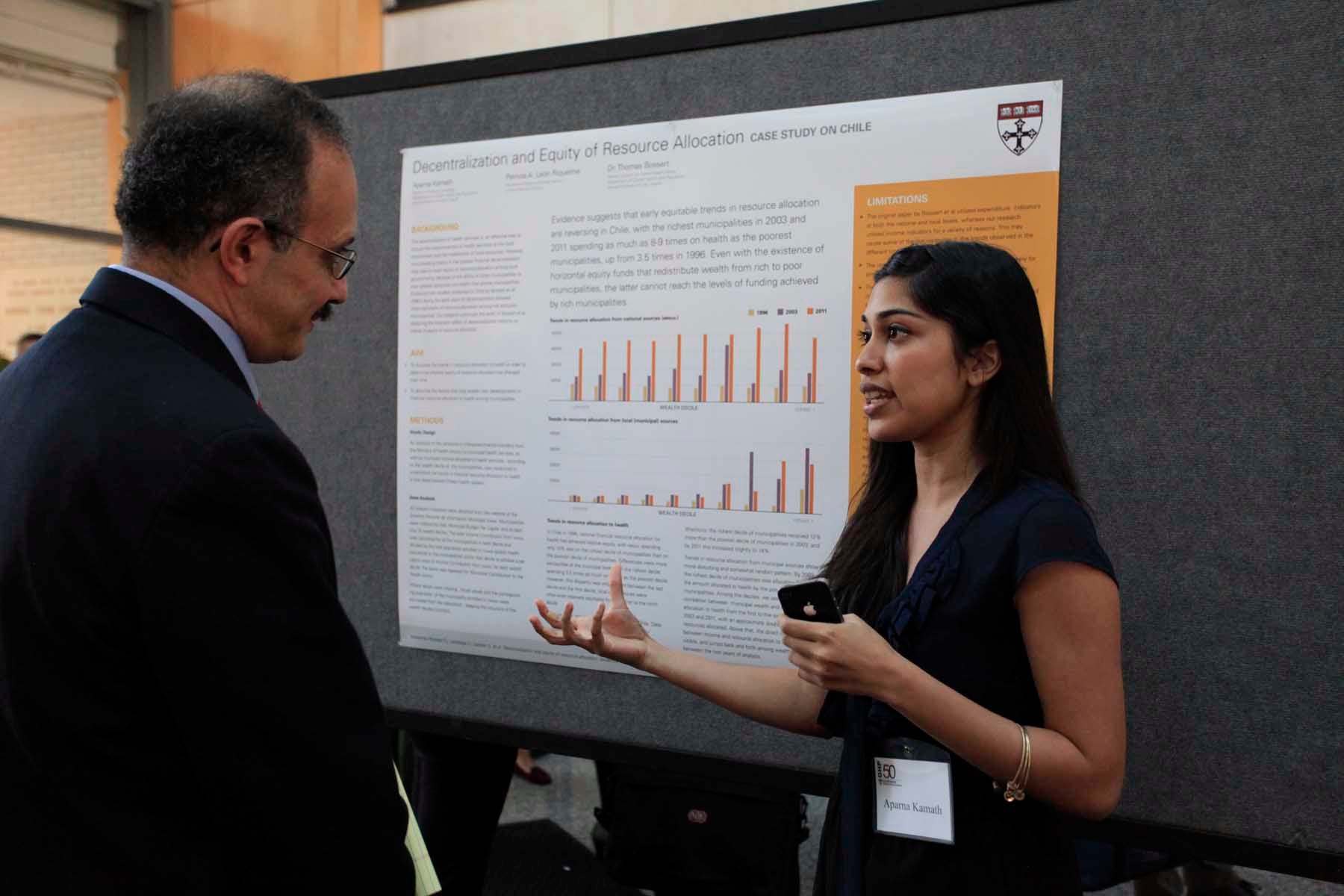
We teach students how to effectively respond to key health challenges impacting populations around the world through outstanding teaching and research. Our expertise includes health systems and economics, global nutrition, maternal and child health, infectious and non-communicable diseases, and humanitarian studies and population ethics.
665 Huntington Avenue
Building 1, 11th and 12th Floors
Boston, MA 02115
Who We Are
We are a community of students, researchers, educators, and practitioners from around the world who work together to produce powerful ideas that improve the lives and health of people everywhere.
Our programs and projects span the globe, and we offer several opportunities for students to take an international travel course. Through distinctive teaching and exceptional research, we strive to advance global health and population studies.
We have long-standing and widely recognized research excellence in fields such as maternal and child health, nutrition, decision science, behavioral economics and implementation sciences, health systems, and population bioethics, humanitarian studies, and human rights.
Through our master’s and doctoral degrees, the Department of Global Health and Population is home to students developing expertise in areas such as health systems design, management, and evaluation; health economics; global infectious and non-communicable diseases; and humanitarian studies and population ethics.
What Sets Us Apart
We have a global footprint with faculty, researchers, and staff present in all regions of the world. Our department is renowned for its unique and diverse background, and we have welcomed students and fellows from most countries in the world.
Our alumni are part of a strong network of public health experts working to devise, implement, and evaluate effective strategies that improve the lives of millions of people around the globe. Our students and fellows have become ministers of health, leaders in national and international public health organizations, and scholars in academic institutions.

‘The beauty of public health is its interconnectedness’
Disha Ganjegunte, SM ’25, brings positive energy and action to international fieldwork and public health advocacy.
1st
Department of population sciences in any school of public health
25
Countries represented among our students
19
Research initiatives, centers, partnerships, and training programs
Our department features plenty of opportunities to engage in cross-Harvard collaboration.
Students traveled abroad to participate in the Harvard Amazon Rainforest Immersion, a ten day course in Brazil offered by David Rockefeller Center for Latin American Studies and the Salata Institute for Climate and Sustainability.
This is one of the many opportunities to study abroad and learn from our faculty in a hands on environment. Learn more about our winter semester courses in Chile, Brazil and Japan.
Department Chair
Degree Programs
Master of Science – Global Health and Population
Prepares individuals to advance global health research and reduce the burden of disease, especially in the world’s most vulnerable populations
Master of Public Health – Global Health
Provides students with the intellectual foundation and specialized skills they need to lead change and make a difference in communities around the world
Doctor of Philosophy – Population Health Sciences
Equips students with the research and analytical tools needed to tackle a wide range of complex, large-scale public health issues
Related Links