 Making Health Care Work Better Through Reforms to Health Care Organization and Public and Private Provision
Making Health Care Work Better Through Reforms to Health Care Organization and Public and Private Provision
Analyzing the organization of provision
Policy Strategies to Address Pluralistic Health Care Markets
Other approaches to reforms in health care organization
IHSP has been developing new approaches to analyzing the performance of health care through better understanding of health care organization, with a particular focus on ambulatory care. Prof. Peter Berman is collaborating with colleagues Profs. Hsiao, Roberts, and Reich at HSPH on a comprehensive approach to health sector reform. This approach involves planning changes to five health system “control knobs” – one of which is organization. Prof. Berman and Roberts have developed the concepts of “macro” and “micro” organization of health care, as shown in the following figure:
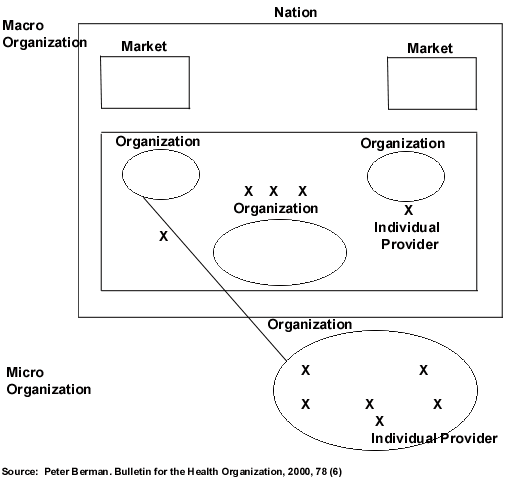
Macro organization refers to the structure and functioning of the provider market, while micro organization refers to the characteristics internal to health care providers, both individuals and larger providers like hospitals.
Analyzing the organization of provision
IHSP has been developing new methods for analyzing the organization of health care provision, the first step in designing and implementing reforms to change organization. Guidelines for the assessment of the role of private health care providers, (Publication Link: DDM No. 9. Assessing the Private Sector: Using Non-Government Resources to Strengthen Public Health Goals) were developed through USAID’s Data for Decision Making Project. They were used to carry out two national private health care assessments, one in Kenya, (Publication Link: DDM No. 20. Kenya: Non-Governmental Health Care Provision) and one in Zambia, (Publication Link: DDM No. 19, Zambia: Non-Governmental Health Care Provision). These studies showed that private providers are a major source of services for many important health problems in African countries with diverse markets, like Kenya and that they are rapidly emerging in countries where they have been banned, as in Zambia. A regional conference in Africa reviewed these and other studies and called from much more systematic efforts in Africa to understand the emerging private sector and develop new regulation and financing strategies in response, (Publication Link: DDM No. 21.1. Conference Report Summaries: Private Providers Contributions to Public Health in Four African Countries, Nairobi, Kenya, November 28, 1994 – December 1, 1994).
A more comprehensive methodology has now been developed by Prof. Berman and applied in studies in Egypt and Poland. In Egypt, an analysis at the national level of the organization of ambulatory care provision highlighted the important role of private physician practices in meeting acute health care needs nationally. It also showed that government hospitals play a larger role in ambulatory care services that government health centers and clinics, despite the widespread development of these facilities in recent years, (Publication Link: DDM No. 82. Understanding the Supply Side: A Conceptual Framework for Describing and Analyzing the Provision of Health Care Services With an Application to Egypt).
In Poland, a “provider market analysis” highlighted the large role now played by private providers in Krakow, Poland’s second largest city. This study also provided for the first time a comprehensive picture of the public and private ambulatory care market, which will in the future be financed by Poland’s new social health insurance system, (Publication Link: DDM No.73. Provision of Ambulatory Health Services in Poland: A Case Study from Krakow).
Policy Strategies to Address Pluralistic Health Care Markets
How should governments respond to diversity in the macro organization of health care? Prof. Berman and Mukesh Chawla have explored this question in a study developing a model for improving resource allocation in public spending that explicitly looks at the role of private provision of priority services. The model uses information on both the demand and supply of health care to assess under when government use of public money to finance private providers would be more cost-effective in improving health than expanding public provision.1 An application of the model analyzes this question in relation to expanding coverage with ante-natal care in Egypt. The results suggest that financing private providers may be more cost-effective than improving the quality of public providers in expanding coverage, (Publication Link: A Methodology for Optimal Allocation of Government Budget to Maximize Health Coverage: The Case of Antenatal Care in Egypt). This work was financed by USAID through the Partnerships for Health Reform project.
Other approaches to reforms in health care organization
IHSP researchers have also looked at the implementation of new organization strategies in developing countries. A five country analysis (Kenya, Zimbabwe, India, Indonesia, and Ghana) of experience with giving government hospitals greater autonomy showed that autonomy programs in lower income countries are difficult to implement. Governments are often reluctant to provide true authority to hospitals in key areas like personnel and function that would enable them to operate more efficiently and to be more responsive to community needs. (Publication Link: DDM No. 32-2. Recent Experiences with Hospital Autonomy in Developing Countries — What Can We Learn?). Dr. Paul Campbell of IHSP has also led an effort to adapt managed care concepts to Zimbabwe’s non-profit medical aid schemes, which are struggling with stagnant finances and the rising costs associated with emerging diseases, (Publication Link: DDM No. 84. Applying Managed Care Concepts and Tools in Zimbabwe).
Please click here for more information on Decentralization in Making Health Care Work Better.
Berman, Peter., et al.,”A Model for Analyzing Strategic Use of Government Financing to Improve Health Care Provision.”1 Major Applied Research 4, Technical Paper 1, Abt Associates Inc., 1999
Click here to return to the IHSP Research home page.



