By Katherina Thomas
Shevin Jacob, MPH ’03, wants desperately ill patients to receive quality care, not just diagnosis and isolation.

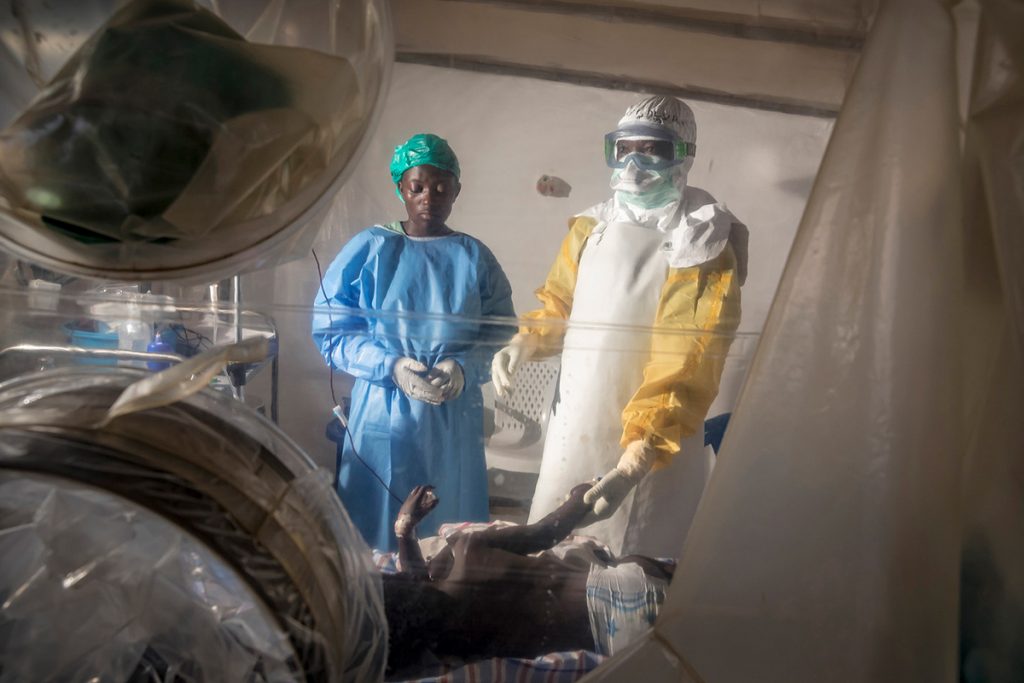
On a warm afternoon in September 2018 in Beni, Democratic Republic of Congo (DRC), Shevin Jacob, MPH ’03, leaned over a young woman severely ill with Ebola. Jacob was dressed in full personal protective equipment (PPE)—suit, gloves, yellow visor curving down over his face. Through the window at his back came glimpses of green; eastern DRC is home to misty mountain forests. He found the scene in front of him more incredible. As he treated the young woman, the patient’s mother—dressed in red and gold, a sea-blue head scarf holding her hair—was able to watch, standing just inches from her daughter, her hand tenderly pressed against a clear plastic barrier.
Jacob had treated hundreds of patients in typical Ebola treatment units (ETUs) during the 2013–2016 West Africa epidemic, which claimed more than 11,300 lives. There, ETUs were made from canvas and plywood: tented field hospitals hemmed in by orange mesh fences. Now he had an unprecedented arsenal of tools: oxygen, investigational therapeutic drugs, Bluetooth EKG monitors. Most innovative of all were the Alliance for Medical Action’s Biosecure Emergency Care Units, known as cubes. In West Africa, ETUs had concealed sick patients from sight, but in Beni the cubes have brought a dose of transparency to an illness steeped in fear.
“The mother of this patient was separated by only a centimeter of plastic wall. She could see her daughter, and her daughter could be comforted by her,” says Jacob. These see-through plastic structures have changed the way that clinicians interact with patients and their families. In a sense, doctors can now prescribe a new medicine in the fight against Ebola: human intimacy .
“In the history of Ebola outbreaks, clinical care was an afterthought. It was ‘isolate and palliate.’” —Shevin Jacob, MPH ’03

Ebola first entered public consciousness in 1976—a year after Jacob was born—when it was discovered in Yambuku, northern DRC. In the 43 years since, the virus has struck 10 countries, with isolated cases in seven more, and has punctuated an era of emerging hemorrhagic fevers, from Marburg to Lassa to Crimean-Congo hemorrhagic fever. Today, we are entering a new age of Ebola epidemics; outbreaks are hitting active war zones and densely populated urban centers, and they are lasting longer. The Beni outbreak features all three of these hazards. As of the end of April, it has infected more than 1,400 people, nearly 900 of whom have died, making it the second-largest Ebola epidemic in history.
Fortunately, as these outbreaks have gained pace, so has Jacob’s work. His field experiences and singular research path have helped him work with organizations like the World Health Organization (WHO) to tackle such fast-moving crises. Before Beni, he was at the front lines of the 2013–2016 Ebola epidemic in Guinea, Sierra Leone, and Liberia, steadfastly advocating for the highest degree of bedside care. He has demonstrated that managing Ebola patients must include options for the sickest individuals: IV lines, electrolyte repletion, close monitoring, sufficient staffing ratios, and fast access to lab tests. “In the history of Ebola outbreaks, clinical care was an afterthought,” Jacob says. “It was ‘isolate and palliate,’ with minimal effort on how to improve supportive care and therefore survival.”
In March and April 2014, when the world had barely woken to the Ebola outbreak, Jacob collaborated with other clinicians on a study of Ebola patients at Donka Hospital in Guinea. Survival rates were grim, hovering near 30 percent, but his observations were clear: With optimized supportive care, patients were more likely to recover.
Sepsis: Deadly inflammation
Jacob, who received the Harvard Chan School Alumni Association’s 2018 Leadership Award in Public Health Practice, is an expert, not primarily in Ebola or other viral hemorrhagic fevers but in sepsis—a deadly medical emergency that develops when the body overreacts to another infection. The inflammatory response can be so severe and systemic that both blood pressure and platelet counts plummet, prompting a cascade of physiological failures that include loss of blood flow to vital organs like the kidneys and brain. Patients who are immunocompromised, such as those ill with HIV and tuberculosis, are at increased risk for sepsis. It is one of the most common causes of death from AIDS, particularly in sub-Saharan Africa.
Jacob’s interest in the condition began when he was studying for his MPH at the Harvard Chan School. It was 2002, in the midst of a global AIDS controversy. Some 22 million people had by then died from AIDS-related causes, and a debate raged: Should funding be steered toward treatment or prevention? Some held AIDS to be untreatable in resource-limited settings, while others, including global health pioneer Paul Farmer, were finding ways to deliver antiretrovirals to HIV patients in Haiti despite claims that it couldn’t and shouldn’t be done. Jacob and his peers launched a think tank to discuss new approaches to the conversation; among them was the idea, then still unproven, that HIV was not a direct cause of death. “At the time, the question was, ‘If patients weren’t dying from HIV, then what were they actually dying from?’”
Jacob suspected that sepsis was a common cause of HIV/AIDS-related mortality, though few studies had disaggregated the causes of death. Pinpointing the causes, he thought, would allow for targeted interventions that could save lives. Sepsis, for example, requires rapid rehydration. Jacob had found his passion: the care and management of severely ill people in resource-limited settings, initially through the lens of sepsis.
Global health’s blind spot
In the classic public health parable, fishermen who cast their nets downstream will spot someone falling downriver, gasping for life. They haul that person out, only to rescue another person, then another. Eventually, they head upstream to see what’s going on, where they discover a steep cliff edge without a safety fence. The story is often used to explain the need for public health preventive measures (upstream) in concert with clinical interventions (downstream).
Jacob offers a discomfiting sequel: At another river, this one flanked by mangroves and baked by the steady gaze of the sun, there are fences upstream—but downstream, people are still dying. “No preventive measure has 100 percent penetrance—not vaccines, not health promotion, not contact tracing,” he says. “In low-resource settings, patients are falling through the holes. It’s global health’s blind spot.”
Jacob began his sepsis work in sub-Saharan Africa 13 years ago, in 2006. He was a second-year resident in internal medicine at the University of Virginia when his mentor connected him to Makerere University, in Kampala, Uganda. Then barely 30 and a newly minted physician, he led the first-ever study of the care of septic patients in a resource-limited setting. The results from it and a subsequent study highlighted what he had suspected: that simple, affordable bedside care—high volumes of IV fluids, early monitoring—was associated with improved survival.
Yet as he continued on his academic journey, completing his fellowship in infectious diseases at the University of Washington, he found that the topic wasn’t a conventional one in research. In fact, he encountered “a sense of futility” among funders and other researchers. The sickest patients in poor countries were surely going to die anyway, they reasoned, so why not invest resources elsewhere? “Yes, there are a number of systemic issues in many African settings, and yes, some patients are going to die,” Jacob retorts, “but just because we don’t have the big bells and whistles of intensive care units in those places doesn’t mean we can’t save lives.”
His trips to Uganda, where he had sparked growing interest in managing sepsis, grew more and more frequent. One of his earliest collaborators there was an accomplished pediatric physician, Nathan Kenya-Mugisha, then the director of Masaka Regional Referral Hospital, who would later become the acting director general of the Uganda ministry of health. In a country where one in five newborn deaths is due to sepsis, Kenya-Mugisha didn’t subscribe to the conventional wisdom that researching the condition was a futile exercise.
“At that time, there wasn’t a lot of specialist knowledge about sepsis in Uganda, and we needed it,” says Kenya-Mugisha. “This research has now translated into policy and practice.” It would probably not have happened without such long-standing dedication from Jacob. While many foreign researchers fly in and out, Jacob’s work is intimately bound to the long-term act of caring.
Kenya-Mugisha adds: “After the on-duty senior doctors went home, sometimes Shevin would stay the whole night with interns and medical students. He just couldn’t leave his patients, even though he wasn’t on duty.” Kenya-Mugisha used to tease Jacob. “When do you sleep?” he’d say. Thirteen years on, he still asks Jacob the same question.
Shaped by values of service and compassion
In conversation, Jacob broaches his work with passion, bringing infectious ardor to everything he says, enthusiastic but never effusive. He rarely, however, alights on himself—his interest is impact, not image, and a warmth and modesty course through his interactions.
He grew up in the southern suburbs of Chicago, as the middle child between two sisters. His parents—his father, a retired OB-GYN, and his mother, who raised him and his siblings—held respect, acts of service, and compassion in high regard, imbuing the family with a clear moral compass. “They drove a strong ethical stance,” he says.
Jacob attended majority white, Catholic schools, coming home to treasured stories of his parents’ childhoods and ancestry in Kerala, India—like heirlooms, the tales were passed down through generations. His grandfather, P.J. Sebastian, featured prominently in their tapestry; he was an eminent lawyer, social activist, and freedom fighter who was repeatedly imprisoned for speaking out against injustices under the occupation of the British Raj. “Though he died before we were born, his story influenced the lives of my sisters and me in a major way,” Jacob says. His older sister is now a nurse practitioner and public health practitioner; his younger sister, a teacher. All three have “spent time working and living in low- and middle-income countries, wanting to carry the torch that he passed onto us in fighting for social justice.” As an undergraduate at St. Louis University, Jacob and his roommate ran the school’s Amnesty International chapter.
Jacob came to the Harvard Chan School for his MPH while in medical school at Oregon Health & Science University. “Harvard Chan gave me the theoretical foundation to develop the tools for navigating challenging public health situations in the real world,” he says, adding, “It’s an incredible place because it’s this nexus of all the people you’ve been wanting to meet. I have the greatest set of friends from that time. They’re some of my dearest friends, though we were only together for nine months.”
He keeps in touch with them from Uganda, where he has lived and worked since 2006. At the Infectious Diseases Institute at Makerere University, Jacob is the team lead for the Global Health Security Department and advises on a portfolio that includes outbreak preparedness and response, antimicrobial resistance, and laboratory systems strengthening. He holds an academic position at the Liverpool School of Tropical Medicine, United Kingdom, where he is senior clinical lecturer in sepsis research, and an affiliate position at the University of Washington.
He also maintains involvement with Walimu, the nonprofit organization he founded in 2010 with other research doctors, as its medical director. Walimu—the Swahili word for “teachers”—was born out of the philosophy that quality care in resource-limited settings can be delivered to the most severely ill patients through training and post-training reinforcement of front-line health workers.
A peripatetic life comes with challenges, but Jacob’s greatest influences—medicine, his family—have given him a sturdy map. The drive for improved supportive care is his true north. Meanwhile, his house in Kampala, Uganda’s capital, is his haven. Kampala is a mixed palette; green with foliage, gray with concrete, blue with Lake Victoria, which sits among the city’s seven hills. It may be one of the most polluted cities in Africa—boda boda bikes and matatu minibuses weave through the city’s tight roadways—but Jacob still wakes to birdsong: the alarm clock call of the hadada ibis, the maniacal cry of the eastern gray plantain eater.
By now a longtime resident of Uganda, Jacob has been accorded a deeper level of respect not often granted to foreign researchers. “He has a feeling for Uganda, an attachment to people here, for saving lives here,” says Kenya-Mugisha, who is now the executive director of Walimu. “Many people come here with a research agenda, but when their project is complete, that’s it. Shevin isn’t aloof in that way; he closely works with Ugandan health workers, always contributing, always building capacity.”
“He eagerly and doggedly pushes against dichotomies of care delivery for patients in different settings,” adds Jacob’s close friend and colleague Ian Crozier, also an infectious-diseases physician, “while his considerable on-ground African experience brings a pragmatism that avoids that windmill tilting that sometimes comes with unfettered enthusiasm.”
“Nothing happens in a vacuum,” says Jacob. Meaningful collaboration within African contexts “requires an investment. Just because you’re from some ivory tower doesn’t mean you will have more expertise. People know a lot about their own setting.”
“There are moments of light and darkness that happen within an Ebola outbreak,” says Shevin Jacob, “and sometimes the moments of light are shattered.”
Moments of light and darkness
Jacob remembers the day he flew into Freetown, Sierra Leone’s capital. It was July 31, 2014, and the sky hung heavy. It often does during the rainy season, but that day seemed more overcast than most: Sheik Humarr Khan had died from Ebola two days earlier and was to be buried. Khan was Sierra Leone’s leading virologist, an acclaimed Lassa fever researcher who was leading the fight against Ebola in the eastern city of Kenema. Jacob was part of a WHO team—working on an unpaid contract, expenses-only—brought in to help succeed him.
Jacob arrived to harrowing scenes. Kenema was badly hit, and 22 health workers at Khan’s hospital were by then among the dead. Nurses and physician’s assistants were not being paid and many had gone on strike. The makeshift Ebola ward was packed with about 80 patients—some confirmed with the disease, some under observation, many not properly triaged. There weren’t enough gum boots or gloves, let alone enough staff, and the government had begun to draft nursing students, who were frightened and unprepared. As the health system buckled, death tightened its grip; corpses were bagged and hauled through waiting areas, as suspected patients looked on. “It was a horrible situation,” says Jacob.
Among his colleagues on that mission were John Schieffelin, an infectious-diseases physician from Tulane University, and a British nurse, Will Pooley. It soon became clear that they needed more help. The hospital’s health workers were dying, their photographs coating a cream-colored wall. As the wall thickened with taped-up tributes, staff numbers thinned. Distraught, Jacob made some calls. First on his list was Ian Crozier. Would he come? Jacob asked. Crozier flew in.
“There are moments of light and darkness that happen within an Ebola outbreak,” Jacob says, “and sometimes the moments of light are shattered, when the patient you may have made a connection with or you’ve been really fighting for ends up having a bad outcome.”
He remembers one patient in particular, a 2-year-old boy. Known as Baby Borbor, he came into the unit with his mother. She tested positive, but although the toddler’s bloodwork was clear, his family was afraid to come for him; stigma was spreading as fast as the virus. With nowhere for him to go, the team opted to admit him; a decision that Jacob says he would not make today. “He was on the same bed as his mom, seemingly unfazed by the horrors around him,” he says. “He was everybody’s hope in a dark period.”
When Baby Borbor’s mother died, the medical team didn’t know what to do. There were no firm guidelines, no precedents to follow. Jacob made the call: They would set up a temporary crib for him away from any patient traffic and test him again after five days. The results: negative. Overjoyed, the team moved him to the nurses station, where they took turns between shifts playing with him. Only then did the toddler grow feverish and irritable. “We retested him and he was positive,” says Jacob. “We were gutted. He succumbed to his illness a week later, in the very same ward where his mother had died.”
Exhausted from such pendulous swings, Jacob flew to London for a weekend of rest before his planned return to Uganda. Then he got the first phone call: Pooley, the nurse, had tested positive for Ebola—his exposure traced to Baby Borbor—and was being evacuated to London (he would survive). Public Health England quarantined Jacob, though he was asymptomatic. The U.S. embassy put up Jacob in a safe house, where for the first time in weeks, he was “forced to sit still with my thoughts.” He found it “punitive and isolating”—the very feelings he is trying to prevent or allay in his own Ebola patients. Meanwhile, he learned that another team member in Sierra Leone had died from Ebola.
Jacob’s quarantine was lifting when he got a call from Crozier. “He said he had a fever and he’d had a really rough night.” So began the six-week nightmare that saw Crozier become an unwitting Ebola celebrity, evacuated in a Gulfstream G-III jet to Emory University Hospital in Atlanta. He was so critically ill that he was placed on a ventilator and, as end-stage Ebola ravaged his kidneys, dialysis.
Jacob and Crozier knew each other from Uganda, but their friendship was, as Crozier puts it, “forged in the fire of Ebola.” Jacob flew home to Kampala, from whence he pitched in with clinical advice, supporting Crozier’s parents and brother. “I was getting sicker and sicker … My body was trying to die, but Shevin was absolutely present—without ever being physically present at Emory,” Crozier says. “He had such a huge experience in caring for Ebola patients in West Africa, and he quietly played a remarkable role in my own care, to the point where he pretty much became a member of my core clinical team.”
Looking back on his critical role in Crozier’s recovery, Jacob is characteristically gracious. “He’s my buddy,” he says. On a couple of occasions, Jacob didn’t think Crozier would make it through the night. He wrestled not only with heartache but with guilt as well, having been the one to ask Crozier to come to Kenema in the first place. But he knew the sentiment was misplaced. “Ian had wanted to be there and wouldn’t have changed that, despite eventually getting infected.”
Crozier’s recuperation was long and excruciating, with post-Ebola complications including memory loss and, curiously, a change in color to one of his eyes, a condition caused by lingering viral particles in his ocular tissue. But as Crozier turned the corner, the outbreak continued to rage through West Africa, and it was exacting a psychological toll on Jacob. The ache of Ebola is heavy, cumulative; for survivors and responders, it lingers long after the pathogen has gone. “I don’t think I felt like my usual self until a year after the outbreak ended,” Jacob says. He returned to vipassana meditation, a practice he’d learned before medical school. He threw himself into work. But the greatest healer, he says, was the informal “Ebola veterans club,” comprising clinicians and other responders, where he found camaraderie and a sense of shared experience. And those with whom Jacob has maintained close relationships have one thing in common. “We’ve all galvanized around the same issue: the need for improved supportive care.”
“Just because we don’t have the big bells and whistles of intensive care units in those places doesn’t mean we can’t save lives.”
The future of supportive care
When Jacob entered his 40s, he began to measure his life in decades. “I want to look back at the end of this decade and say I’ve done something that I feel I can walk away from,” he says. “But I’m not there yet.” Yet his work is now contributing to a new era of more meaningful care for patients with sepsis, Ebola, and other life-threatening conditions in resource-constrained settings.
Jacob is spearheading crosscutting efforts to stem sepsis deaths across sub-Saharan Africa, and his calls for improved patient care and diagnostics are no longer falling on such deaf ears. Through his work at Liverpool School of Tropical Medicine and the African Sepsis Alliance, a network of clinicians and researchers across 15 African countries dedicated to improving quality of care for sepsis, he is building research capacity, developing standardized guidelines, and rolling out pilot programs to improve treatment outcomes.
As the outbreak continues to ravage eastern DRC, Jacob is part of a WHO clinical team working to apply universal standards of care to Ebola. The virus, to him, is a symptom of the same persistent empathy gap that separates the poor from the rich, one that favors isolation over connection, leaving critically ill patients with the wrong-colored passports to die.
In September 2018, a strange twist of fate took Jacob and Crozier to Beni, where for two weeks they reunited on the same close-knit WHO Ebola team they had been part of four years earlier in Kenema. It was a different time, a different context, and much had changed since West Africa. There was improved patient monitoring, adjacent labs, investigational therapeutics, new technology. But they also met greater challenges: PPE now meant not just masks and gowns but also helmets and flak jackets to shield them from ongoing attacks by the Allied Democratic Forces, a rebel group that has been active in the region for decades. During that trip, Crozier marked the four-year anniversary of his high-profile diagnosis, Jacob saw in his 43rd birthday, and the world observed 42 years of Ebola. “It was a profound moment for us, to have that strange reunion in a strange place,” he says.
Perhaps it wasn’t so strange after all. In Beni, following years of dedication working to flip isolation paradigms for the desperately ill, Jacob saw the early fruits of his and his colleagues’ labor. “I think it’s amazing to see it growing into something robust from a seed we had planted before,” he says.
If Ebola is a crisis of human connection, then meaningful supportive care—and those like Jacob who offer it—is an antidote. And if anything represents the progress made, it is the single-patient transparent cubes. Like many supportive care mechanisms, they are simple but powerful, restoring humanity to moments so easily stripped of them.
Crozier captured the poignant interaction between mother and daughter—nothing but love and plastic between them—in a photograph. Fittingly, Jacob is in the picture too, though nearly obscured by his protective gear.
“There’s been a real evolution from the West Africa outbreak, and there’s still a long way to go,” Jacob says, “but isn’t it incredible? That picture has never happened in the history of outbreaks before.”
Katherina Thomas writes about global health and infectious diseases, with a focus on human connections and health inequities in Ebola outbreaks. She was the founding editor of Ebola Deeply, a platform created to provide deeper and more contextual information about the 2013–2016 West Africa Ebola epidemic.
Photos: Kent Dayton, AP/Al-hadji Kudra Maliro, Panos/Svenn Torfinn







