Protein is an essential macronutrient, but not all food sources of protein are created equal, and you may not need as much as you think. Learn the basics about protein and shaping your diet with healthy protein foods.
Jump to:
–What is protein?
–How much protein do I need?
–It’s all about the protein “package”
–Research on protein and human health
–Protein foods and the planet
–The bottom line: choosing healthy protein foods
–[Quiz] Test your protein knowledge!
What Is Protein?
Protein is found throughout the body—in muscle, bone, skin, hair, and virtually every other body part or tissue. It makes up the enzymes that power many chemical reactions and the hemoglobin that carries oxygen in your blood. At least 10,000 different proteins make you what you are and keep you that way.
Protein is made from twenty-plus basic building blocks called amino acids. Because we don’t store amino acids, our bodies make them in two different ways: either from scratch, or by modifying others. Nine amino acids—histidine, isoleucine, leucine, lysine, methionine, phenylalanine, threonine, tryptophan, and valine—known as the essential amino acids, must come from food.
How Much Protein Do I Need?
The National Academy of Medicine recommends that adults get a minimum of 0.8 grams of protein for every kilogram of body weight per day, or just over 7 grams for every 20 pounds of body weight. [1]
- For a 140-pound person, that means about 50 grams of protein each day.
- For a 200-pound person, that means about 70 grams of protein each day.
The National Academy of Medicine also sets a wide range for acceptable protein intake—anywhere from 10% to 35% of calories each day. Beyond that, there’s relatively little solid information on the ideal amount of protein in the diet or the healthiest target for calories contributed by protein. In an analysis conducted at Harvard among more than 130,000 men and women who were followed for up to 32 years, the percentage of calories from total protein intake was not related to overall mortality or to specific causes of death. [2] However, the source of protein was important.
What are “complete” proteins, and how much do I need?
“Pure” protein, whether derived from plant or animal foods, probably has similar effects on health, although the mix of amino acids can have health implications. Some proteins found in food are “complete,” meaning they contain all twenty-plus types of amino acids needed to make new protein in the body. Others are incomplete, lacking one or more of the nine essential amino acids, which our bodies can’t make from scratch or from other amino acids. Animal-based foods (meat, poultry, fish, eggs, and dairy foods) tend to be good sources of complete protein, while plant-based foods (fruits, vegetables, grains, nuts, and seeds) often lack one or more essential amino acid. Those who abstain from eating animal-based foods can eat a variety of protein-containing plant foods each day in order to get all the amino acids needed to make new protein, and also choose to incorporate complete plant proteins like quinoa and chia seeds.
It’s important to note that millions of people worldwide, especially young children, don’t get enough protein due to food insecurity. The effects of protein deficiency and malnutrition range in severity from growth failure and loss of muscle mass to decreased immunity, weakening of the heart and respiratory system, and death.
However, it’s uncommon for healthy adults in the U.S. and most other developed countries to have a deficiency, because there’s an abundance of plant and animal-based foods full of protein. In fact, many in the U.S. are consuming more than enough protein, especially from animal-based foods. [3]
It’s All About the Protein “Package”
When we eat foods for protein, we also eat everything that comes alongside it: the different fats, fiber, sodium, and more. It’s this protein “package” that’s likely to make a difference for health.
The table below shows a sample of food “packages” sorted by protein content, alongside a range of components that come with it.
Table: Comparing protein packages
![table comparing protein packages Food /[Category] Protein (g) Saturated Fat (g) Mono-unsaturated Fat (g) Poly-unsaturated Fat (g) ALA (g) Marine Omega-3 Fats (g) Fiber (g) Sodium (mg) Sirloin steak, broiled (4oz) [Red Meat] 33 4.6 4.9 0.4 0.4 0 0 66 Sockeye salmon, grilled (4oz) [Seafood] 30 1.1 2.1 1.5 0.3 1.0 0 104 Chicken, thigh, no skin (4oz) [Poultry] 28 2.7 3.9 2.0 0.1 0.1 0 120 Ham steak (4oz) [Red Meat] 22 1.6 2.2 0.5 0.5 0 0 1,439 Lentils (1 cup, cooked) [Legumes] 18 0.1 0.1 0.3 0.3 0 15 4 Milk (8oz) [Dairy] 8 3.1 1.4 0.2 0.3 O0 0 115 Almonds, dry roasted, unsalted (1oz) [Nuts] 6 1.2 9.4 3.4 0 0 3.1 1](https://www.hsph.harvard.edu/nutritionsource/wp-content/uploads/sites/30/2018/11/Screen-Shot-2018-11-08-at-3.52.40-PM.png)
To call out a few examples:
- A 4-ounce broiled sirloin steak is a great source of protein—about 33 grams worth. But it also delivers about 5 grams of saturated fat.
- A 4-ounce ham steak with 22 grams of protein has only 1.6 grams of saturated fat, but it’s loaded with 1,500 milligrams worth of sodium.
- 4 ounces of grilled sockeye salmon has about 30 grams of protein, naturally low in sodium, and contains just over 1 gram of saturated fat. Salmon and other fatty fish are also excellent sources of omega-3 fats, a type of fat that’s especially good for the heart.
- A cup of cooked lentils provides about 18 grams of protein and 15 grams of fiber, and it has virtually no saturated fat or sodium.
Powdered protein can come from a variety of sources, including eggs, milk (e.g., casein, whey), and plants (e.g., soybeans, peas, hemp). Some protein powders contain protein from multiple sources; for instance, a vegan option might include protein derived from peas, pumpkin seeds, sunflower seeds, and alfalfa. Like other dietary supplements, protein powders are not regulated by the U.S. Food and Drug Administration for safety. They can often contain non-protein ingredients, including vitamins and minerals, thickeners, added sugars, non-caloric sweeteners, and artificial flavoring. If you choose to consume protein powder, it is important to read the nutrition and ingredient labels beforehand, as products may contain unexpected ingredients and large amounts of added sugars and calories.
Learn more about protein powders and other workout supplementsResearch on Protein and Health
Available evidence indicates that it’s the source of protein (or, the protein “package”), rather than the amount of protein, that likely makes a difference for our health. You can explore the research related to each disease in the tabs below, but here’s the evidence-based takeaway: eating healthy protein sources like beans, nuts, fish, or poultry in place of red meat and processed meat can lower the risk of several diseases and premature death.
Heart disease
Research conducted at the Harvard Chan School of Public Health has found that eating even small amounts of red meat—especially processed red meat—on a regular basis is linked to an increased risk of heart disease and stroke, and the risk of dying from cardiovascular disease or any other cause. [4-6] Conversely, replacing red and processed red meat with healthy protein sources such as beans, soy foods, nuts, fish, or poultry seems to reduce these risks. One of the reasons why plant sources of protein are related to lower risk of cardiovascular disease compared to protein from red meat and dairy is because of the different types of fat in these protein packages. Plant-based protein sources are more unsaturated, which lowers LDL cholesterol—an established risk factor for heart disease. Also, plant sources contain no cholesterol. Other factors are likely to contribute to the lower risk, but this is a key factor.
- One investigation followed 120,000 men and women in the Nurses’ Health Study and Health Professionals Follow-Up Study for more than two decades. For every additional 3-ounce serving of unprocessed red meat the study participants consumed each day, their risk of dying from cardiovascular disease increased by 13%. [5]
- Processed red meat was even more strongly linked to dying from cardiovascular disease—and in smaller amounts: every additional 1.5 ounce serving of processed red meat consumed each day (equivalent to one hot dog or two strips of bacon) was linked to a 20% increase in the risk of cardiovascular disease death.
- Cutting back on red meat could save lives: the researchers estimated that if all the men and women in the study had reduced their total red and processed red meat intake to less than half a serving a day, one in ten cardiovascular disease deaths would have been prevented.
- In another study of 43,000 men that looked at both amount and sources of protein found that intake of total protein was minimally associated with heart disease risk, but intake of protein from red meat was associated with higher risk. [7]
Diabetes
Again, the source of protein matters more than protein quantity when it comes to diabetes risk. Eating more red meat predicts a higher risk of type 2 diabetes, while consuming nuts, legumes, and poultry is related to lower risk.
- A 2011 study found that people who ate diets high in red meat, especially processed red meat, had a higher risk of type 2 diabetes than those who rarely ate red or processed meat. [12] For each additional serving a day of red meat or processed red meat that study participants ate, their risk of diabetes rose 12% and 32%, respectively. Investigators also found that replacing a serving of red meat with one serving of nuts, low-fat dairy products, or whole grains each day was associated with an estimated 16% to 35% lower risk of type 2 diabetes.
- A related study also found that people who started eating more red meat than usual were had a 50% higher risk of developing type 2 diabetes during the next four years, and researchers also found that those who reduced red meat consumption had a 14% lower risk of type 2 diabetes over a 10-year follow-up period. [13]
- How meat is cooked may also affect type 2 diabetes risk. In a study that tracked the health of over 289,000 men and women, researchers found that individuals who most frequently ate red meats and chicken cooked at high temperatures were 1.5 times more likely to develop type 2 diabetes, compared to those who ate the least. There was also an increased risk of weight gain and developing obesity in the frequent users of high-temperature cooking methods, which may have contributed to the development of diabetes. Of note, this research demonstrated that cooking methods might contribute to diabetes risk beyond the effects of meat consumption alone. [14] Learn more about this study.
- More evidence that the source of protein matters comes from a 20-year study that looked at the relationship between low-carbohydrate diets and type 2 diabetes in women. Low-carbohydrate diets that were high in vegetable sources of fat and protein were associated with a lower risk of type 2 diabetes. [15] But low-carbohydrate diets that were high in animal sources of protein or fat did not show this benefit.
- For type 1 diabetes (formerly called juvenile or insulin-dependent diabetes), proteins found in cow’s milk have been implicated in the development of the disease in babies with a predisposition to the disease, but research remains inconclusive. [16,17]
Cancer
When it comes to cancer, once again, the source of protein seems to matter more than quantity.
- In the Nurse’s Health Study and the Health Professionals Follow-Up Study, every additional serving per day of red meat or processed red meat was associated with a 10% and 16% higher risk of cancer death, respectively. [5]
- In October 2015, the World Health Organization (WHO)’s International Agency for Research on Cancer (IARC) concluded that consumption of processed meat is “carcinogenic to humans,” and that consumption of red meat is “probably carcinogenic to humans.” [18] The IARC Working Group (comprised of 22 scientists from ten countries) reached these conclusions from an evaluation of over 800 studies.
- Conclusions were primarily based on the evidence for colorectal cancer. Data also showed positive associations between processed meat consumption and stomach cancer, and between red meat consumption and pancreatic and prostate cancer.
- A 2014 study also found a link between high consumption of red meat during adolescence and premenopausal breast cancer, while higher intakes of poultry, nuts, and legumes were associated with lower risk. Using data on the health of 89,000 women (aged 24 to 43) followed over a 20-year period, researchers found a 22% higher risk of breast cancer in those who ate 1.5 servings of red meat per day while in high school, compared to those who only had one serving per week. Each additional daily serving of red meat seemed to increase the risk of breast cancer by another 13%. [19]
- How meat is cooked may also have implications for cancer risk. High-temperature grilling creates potentially cancer-causing compounds in meat, including polycyclic aromatic hydrocarbons and heterocyclic amines. Learn about tips for healthy grilling.
Premature death
- In 2016, researchers reviewed protein intakes of more than 131,000 women and men from the Nurses’ Health Study and Health Professionals Follow-up Study. After tracking their diets for up to 32 years, the authors found that a higher intake of red meat, especially processed versions (sausage, bacon, hot dogs, salami), was linked to a modestly higher risk of death, while a higher protein intake from plant foods carried a lower risk. [2] Learn more about this study.
Bone health
- Digesting protein releases acids into the bloodstream, which the body usually neutralizes with calcium and other buffering agents. As a result, early research theorized that eating lots of protein requires a lot more calcium – which may be pulled from bone. A 2009 systematic review found that this doesn’t appear to happen. [20]
Weight control
The same healthy protein foods that are good choices for disease prevention may also help with weight control. Again, it’s the source of protein that matters.
- Researchers at the Harvard Chan School of Public Health followed the diet and lifestyle habits of over 120,000 men and women for up to 20 years, looking at how small changes contributed to weight gain over time. [21]
- Those who ate more red and processed meat over the course of the study gained more weight, about one extra pound every four years, while those who ate more nuts over the course of the study gained less weight, about a half pound less every four years.
- A subsequent detailed analysis of this cohort also found that eating red meat, chicken with skin, and regular cheese was associated with greater weight gain. Yogurt, peanut butter, walnuts and other nuts, chicken without skin, low-fat cheese, and seafood was associated with less weight gain. [22]
- Another study showed that eating around one daily serving of beans, chickpeas, lentils or peas can increase fullness, which may lead to better weight management and weight loss. [23]
There’s no need to go overboard on protein. Though some studies show benefits of high-protein, low-carbohydrate diets in the short term (such as the paleo diet), avoiding fruits and whole grains means missing out on healthful fiber, vitamins, minerals, and other phytonutrients.
Other considerations involving protein
- Specific proteins in food and the environment are involved in food allergies, which are overreactions of the immune system (take gluten and celiac disease, for example).
- Medical journals are also full of reports linking allergic responses to specific protein sources with a variety of conditions (breathing problems, chronic digestive issues, etc.). Eggs, fish, milk, peanuts, tree nuts, and soybeans cause allergic reactions in some people.
- Individuals diagnosed with certain diseases (such as kidney and liver disease) need to monitor their protein intake according to their physician’s guidelines.
- You may have also heard that the use of antibiotics in the production of animal-based foods has contributed to the emergence of “superbugs,” or strains of bacteria resistant to currently available antibiotics. In 2016, the FDA announced a voluntary program to limit the routine use of antibiotics in food production (such as giving antibiotics to healthy animals to help them grow faster). [24] As a consumer, you may want to find products “raised without antibiotics” if you plan on eating meat. Some companies feature this language on the packaging, others don’t.
People who eat just two servings of red meat per week may have an increased risk of developing type 2 diabetes compared to people who eat fewer servings, and the risk increases with greater consumption, according to a new study led by researchers from Harvard T.H. Chan School of Public Health. They also found that replacing red meat with healthy plant-based protein sources, such as nuts and legumes, or modest amounts of dairy foods, was associated with reduced risk of type 2 diabetes.
Read moreProtein Foods and the Planet

Just as different foods can have differing impacts on human health, they also have
differing impacts on the environment. Agriculture is a major contributor of greenhouse gas (GHG) emissions globally, the accumulation of which is driving climate change at a rate unprecedented in human history. However, not all foods have an equal impact. Production of animal-based foods tends to have higher GHG emissions than producing plant-based foods—and dairy and especially red meat (particularly beef, lamb, and goat) stand out for their disproportionate impact.
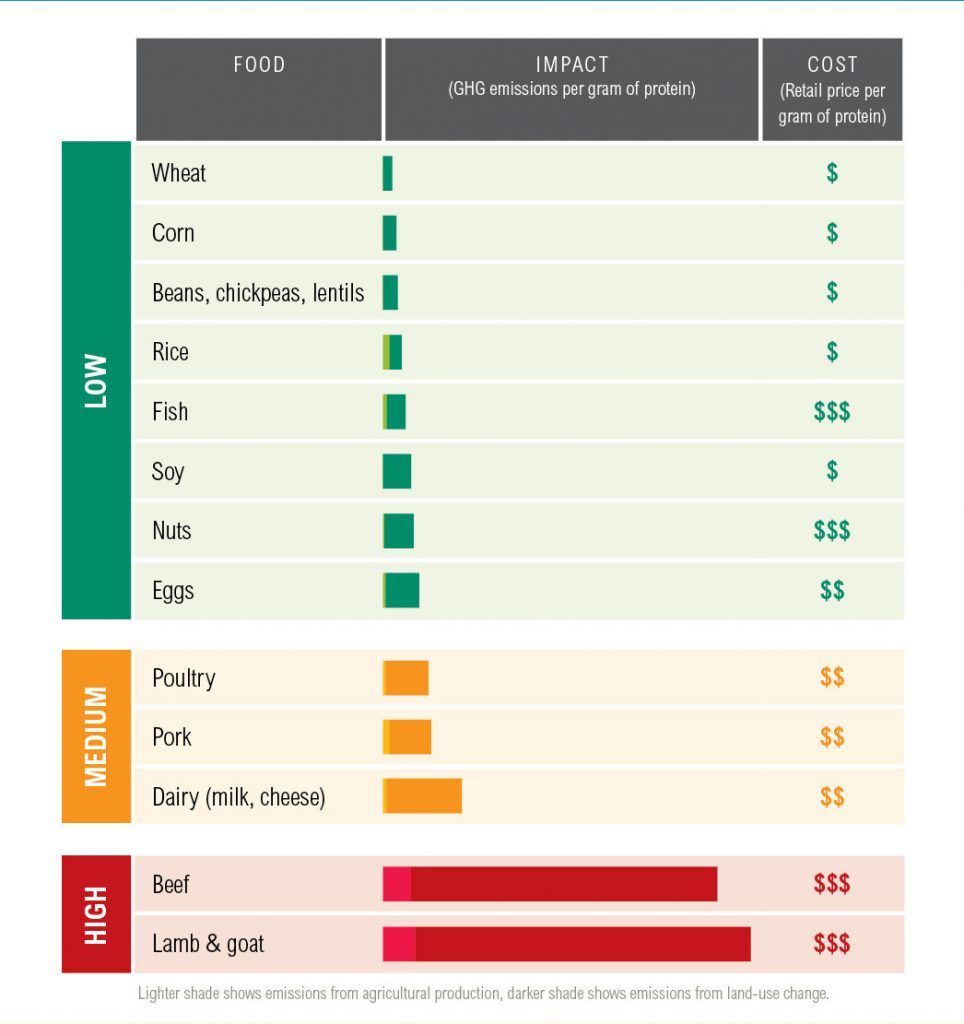
- Source: World Resources Institute, www.wri.org/proteinscorecard
To give you an idea, this “scorecard” from the World Resources Institute illustrates the differing GHG emissions per gram of protein from both animal and plant-based protein foods. [25] Making just one pound (454 grams) of lamb generates five times more GHGs than making a pound of chicken and around 30 times more than making a pound of lentils. [26] In the U.S. alone, beef accounts for 36% of all food-related GHG emissions. [27] Beyond emissions, it’s also important to note that food production places an enormous demand upon our natural resources, as agriculture is a major contributor to deforestation, species extinction, and freshwater depletion and contamination.
Bottom Line
Protein is a key part of any diet. The average person needs about 7 grams of protein every day for every 20 pounds of body weight. Because protein is found in an abundance of foods, many people can easily meet this goal. However, not all protein “packages” are created equal. Because foods contain a lot more than protein, it’s important to pay attention to what else is coming with it. That’s why the Healthy Eating Plate encourages choosing healthy protein foods.
Building off this general guidance, here are some additional details and tips for shaping your diet with the best protein choices:
- Get your protein from plants when possible. Eating legumes (beans and peas), nuts, seeds, whole grains, and other plant-based sources of protein is a win for your health and the health of the planet. If most of your protein comes from plants, make sure that you mix up your sources so no “essential” components of protein are missing. The good news is that the plant kingdom offers plenty of options to mix and match. Here are some examples for each category:
- Legumes: lentils, beans (adzuki, black, fava, chickpeas/garbanzo, kidney, lima, mung, pinto etc.), peas (green, snow, snap, split, etc.), edamame/soybeans (and products made from soy: tofu, tempeh, etc.), peanuts.
- Nuts and Seeds: almonds, pistachios, cashews, walnuts, hazelnuts, pecans, hemp seeds, squash and pumpkin seeds, sunflower seeds, flax seeds, sesame seeds, chia seeds.
- Whole Grains: kamut, teff, wheat, quinoa, rice, wild rice, millet, oats, buckwheat,
- Other: while many vegetables and fruits contain some level of protein, it’s generally in smaller amounts than the other plant-based foods. Some examples with higher protein quantities include corn, broccoli, asparagus, brussels sprouts, and artichokes.
Simple strategies for creating filling, delicious, and even budget-friendly plant-based dishes.
- Upgrade your sources of animal protein. Considering the protein package is particularly important when it comes to animal-based foods:
- Generally, poultry (chicken, turkey, duck) and a variety of seafood (fish, crustaceans, mollusks) are your best bet. Eggs can be a good choice, too.
- If you enjoy dairy foods, it’s best to do so in moderation (think closer to 1-2 servings a day; and incorporating yogurt is probably a better choice than getting all your servings from milk or cheese).
- Red meat—which includes unprocessed beef, pork, lamb, veal, mutton, and goat meat—should be consumed on a more limited basis. If you enjoy red meat, consider eating it in small amounts or only on special occasions.
- Processed meats, such as bacon, hot dogs, sausages, and cold cuts should be avoided. Although these products are often made from red meats, processed meats also include items like turkey bacon, chicken sausage, and deli-sliced chicken and ham. (Processed meat refers to any meat that has been “transformed through salting, curing, fermentation, smoking, or other processes to enhance flavor or improve preservation.” [18])
Looking to reduce red and processed meats, but unsure where to start? Here are a few approaches to cutting-back while keeping your meals satiating and flavorful. Simply find your “starting point” and move forward with the strategies that work for you:
Assess how often you eat red meat, and see if one of these strategies can help you find a way to cut back a bit.
If you’re thinking of a meal that features red meat, see if you can replace it with a better option, like poultry or seafood.
This approach boosts healthy plant-based foods like beans, nuts, whole grains, and other veggies, while still providing ways to incorporate some of your favorite animal-based foods.
Test your protein knowledge!
Ready to see how much you know about protein and healthy protein foods? Try this 10 question quiz to find out:
References
- National Academies of Medicine. Dietary Reference Intakes for Energy, Carbohydrate, Fiber, Fat, Fatty Acids, Cholesterol, Protein, and Amino Acids (Macronutrients).
- Song M, Fung TT, Hu FB, Willett WC, Longo VD, Chan AT, Giovannucci EL. Association of animal and plant protein intake with all-cause and cause-specific mortality. JAMA internal medicine. 2016 Oct 1;176(10):1453-63.
- Fehrenbach KS, Righter AC, Santo RE. A critical examination of the available data sources for estimating meat and protein consumption in the USA. Public health nutrition. 2016 Jun;19(8):1358-67.
- Bernstein AM, Sun Q, Hu FB, Stampfer MJ, Manson JE, Willett WC. Major dietary protein sources and risk of coronary heart disease in women. Circulation. 2010 Aug 31;122(9):876-83.
- Pan A, Sun Q, Bernstein AM, Schulze MB, Manson JE, Stampfer MJ, Willett WC, Hu FB. Red meat consumption and mortality: results from 2 prospective cohort studies. Archives of internal medicine. 2012 Apr 9;172(7):555-63.
- Bernstein AM, Pan A, Rexrode KM, Stampfer M, Hu FB, Mozaffarian D, Willett WC. Dietary protein sources and the risk of stroke in men and women. Stroke. 2011 Jan 1:STROKEAHA-111.
- Preis SR, Stampfer MJ, Spiegelman D, Willett WC, Rimm EB. Dietary protein and risk of ischemic heart disease in middle-aged men–. The American journal of clinical nutrition. 2010 Sep 29;92(5):1265-72.
- Halton TL, Willett WC, Liu S, Manson JE, Albert CM, Rexrode K, Hu FB. Low-carbohydrate-diet score and the risk of coronary heart disease in women. New England Journal of Medicine. 2006 Nov 9;355(19):1991-2002.
- Appel LJ, Sacks FM, Carey VJ, Obarzanek E, Swain JF, Miller ER, Conlin PR, Erlinger TP, Rosner BA, Laranjo NM, Charleston J. Effects of protein, monounsaturated fat, and carbohydrate intake on blood pressure and serum lipids: results of the OmniHeart randomized trial. JAMA. 2005 Nov 16;294(19):2455-64.
- Jenkins DJ, Wong JM, Kendall CW, Esfahani A, Ng VW, Leong TC, Faulkner DA, Vidgen E, Greaves KA, Paul G, Singer W. The effect of a plant-based low-carbohydrate (“Eco-Atkins”) diet on body weight and blood lipid concentrations in hyperlipidemic subjects. Archives of internal medicine. 2009 Jun 8;169(11):1046-54.
- Lagiou P, Sandin S, Lof M, Trichopoulos D, Adami HO, Weiderpass E. Low carbohydrate-high protein diet and incidence of cardiovascular diseases in Swedish women: prospective cohort study. BMJ. 2012 Jun 26;344:e4026.
- Pan A, Sun Q, Bernstein AM, Schulze MB, Manson JE, Willett WC, Hu FB. Red meat consumption and risk of type 2 diabetes: 3 cohorts of US adults and an updated meta-analysis–. The American journal of clinical nutrition. 2011 Aug 10;94(4):1088-96.
- Pan A, Sun Q, Bernstein AM, Manson JE, Willett WC, Hu FB. Changes in red meat consumption and subsequent risk of type 2 diabetes mellitus: three cohorts of US men and women. JAMA internal medicine. 2013 Jul 22;173(14):1328-35.
- Pan A, Sun Q, Bernstein AM, Manson JE, Willett WC, Hu FB. Changes in red meat consumption and subsequent risk of type 2 diabetes mellitus: three cohorts of US men and women.JAMA internal medicine. 2013 Jul 22;173(14):1328-35.
- Halton TL, Liu S, Manson JE, Hu FB. Low-carbohydrate-diet score and risk of type 2 diabetes in women–. The American journal of clinical nutrition. 2008 Feb 1;87(2):339-46.
- Åkerblom HK, Vaarala O, Hyöty H, Ilonen J, Knip M. Environmental factors in the etiology of type 1 diabetes. American journal of medical genetics. 2002 May 30;115(1):18-29.
- Vaarala O, Ilonen J, Ruohtula T, Pesola J, Virtanen SM, Härkönen T, Koski M, Kallioinen H, Tossavainen O, Poussa T, Järvenpää AL. Removal of bovine insulin from cow’s milk formula and early initiation of beta-cell autoimmunity in the FINDIA pilot study. Archives of pediatrics & adolescent medicine. 2012 Jul 1;166(7):608-14.
- Bouvard V, Loomis D, Guyton KZ, Grosse Y, El Ghissassi F, Benbrahim-Tallaa L, Guha N, Mattock H, Straif K. Carcinogenicity of consumption of red and processed meat. The Lancet Oncology. 2015 Dec 1;16(16):1599-600.
- Farvid MS, Cho E, Chen WY, Eliassen AH, Willett WC. Adolescent meat intake and breast cancer risk. International journal of cancer. 2015 Apr 15;136(8):1909-20.
- Darling AL, Millward DJ, Torgerson DJ, Hewitt CE, Lanham-New SA. Dietary protein and bone health: a systematic review and meta-analysis–. The American journal of clinical nutrition. 2009 Nov 4;90(6):1674-92.
- Mozaffarian D, Hao T, Rimm EB, Willett WC, Hu FB. Changes in diet and lifestyle and long-term weight gain in women and men. New England Journal of Medicine. 2011 Jun 23;364(25):2392-404.
- Smith JD, Hou T, Ludwig DS, Rimm EB, Willett W, Hu FB, Mozaffarian D. Changes in intake of protein foods, carbohydrate amount and quality, and long-term weight change: results from 3 prospective cohorts–. The American journal of clinical nutrition. 2015 Apr 8;101(6):1216-24.
- Li SS, Kendall CW, de Souza RJ, Jayalath VH, Cozma AI, Ha V, Mirrahimi A, Chiavaroli L, Augustin LS, Blanco Mejia S, Leiter LA. Dietary pulses, satiety and food intake: A systematic review and meta‐analysis of acute feeding trials. Obesity. 2014 Aug;22(8):1773-80.
- Food and Drug Administration. FDA’s Strategy on Antimicrobial Resistance – Questions and Answers. https://www.fda.gov/animalveterinary/guidancecomplianceenforcement/guidanceforindustry/ucm216939.htm. Accessed on 11/6/2018.
- World Resources Institute. Protein Scorecard. https://www.wri.org/resources/data-visualizations/protein-scorecard. Accessed on 11/6/2018.
- Culinary Institute of America and Harvard T.H. Chan School of Public Health. Menus of Change: 2016 Annual Report. http://www.menusofchange.org/
- Heller MC, Keoleian GA. Greenhouse gas emission estimates of US dietary choices and food loss. Journal of Industrial Ecology. 2015 Jun;19(3):391-401.
- Guasch-Ferré M, Satija A, Blondin S, Janiszewski M, Emlen E, O’Connor L, Campbell W, Hu F, Willett W, Stampfer M. Meta-Analysis of Randomized Controlled Trials of Red Meat Consumption in Comparison With Various Comparison Diets on Cardiovascular Risk Factors. Circulation. 2019 Apr 1;139(15):1828-45.
*Disclosures: Dr. Hu has received research support from the California Walnut Commission. Dr. Campbell reported receiving research support from the National Institutes of Health (T32 Fellowship for Lauren O’Connor), the American Egg Board – The Egg Nutrition Center, The Beef Checkoff Program, The National Dairy Council, The Pork Checkoff Program, and the Barilla Group. Dr. Campbell also reported serving on the 2015 Dietary Guidelines Advisory Committee. Dr. Satija is an employee of Analysis Group, Inc. The other authors declare no conflicts.
Terms of Use
The contents of this website are for educational purposes and are not intended to offer personal medical advice. You should seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The Nutrition Source does not recommend or endorse any products.








![table comparing protein packages Food /[Category] Protein (g) Saturated Fat (g) Mono-unsaturated Fat (g) Poly-unsaturated Fat (g) ALA (g) Marine Omega-3 Fats (g) Fiber (g) Sodium (mg) Sirloin steak, broiled (4oz) [Red Meat] 33 4.6 4.9 0.4 0.4 0 0 66 Sockeye salmon, grilled (4oz) [Seafood] 30 1.1 2.1 1.5 0.3 1.0 0 104 Chicken, thigh, no skin (4oz) [Poultry] 28 2.7 3.9 2.0 0.1 0.1 0 120 Ham steak (4oz) [Red Meat] 22 1.6 2.2 0.5 0.5 0 0 1,439 Lentils (1 cup, cooked) [Legumes] 18 0.1 0.1 0.3 0.3 0 15 4 Milk (8oz) [Dairy] 8 3.1 1.4 0.2 0.3 O0 0 115 Almonds, dry roasted, unsalted (1oz) [Nuts] 6 1.2 9.4 3.4 0 0 3.1 1](https://www.hsph.harvard.edu/nutritionsource/wp-content/uploads/sites/30/2018/11/Screen-Shot-2018-11-08-at-3.52.40-PM.png)