Harvard China Health Partnership
The Harvard China Health Partnership (HCHP) is a school-wide initiative dedicated to advancing scholarship on China’s health system, evaluating and designing health policy interventions, and improving health care in China.
665 Huntington Ave
Building 1, Room 1210
Boston, MA 02115
Welcome
The Harvard China Health Partnership (HCHP) is a school-wide effort dedicated to improving the health and well-being of people in China, with global implications. The Partnership is built upon over four decades of deep collaborations with academic and government partners in China, and is currently led by Faculty Director Winnie Yip.
Working closely with our partner institutions, HCHP conducts high-quality and multi-disciplinary research, hosts executive education programs for health policymakers and practitioners, and welcomes visiting scholars from peer institutions across China. We also organize regular events and student seminars at the Harvard Chan School.
What We do

Meaningful Ageing
How can China ensure its rapidly ageing population not only has access to the kind of health care it needs but is also empowered to pursue meaningful lives?

Primary Health Care and Medical Impoverishment
Can improving chronic disease management at the primary care level reduce medical impoverishment in rural China?
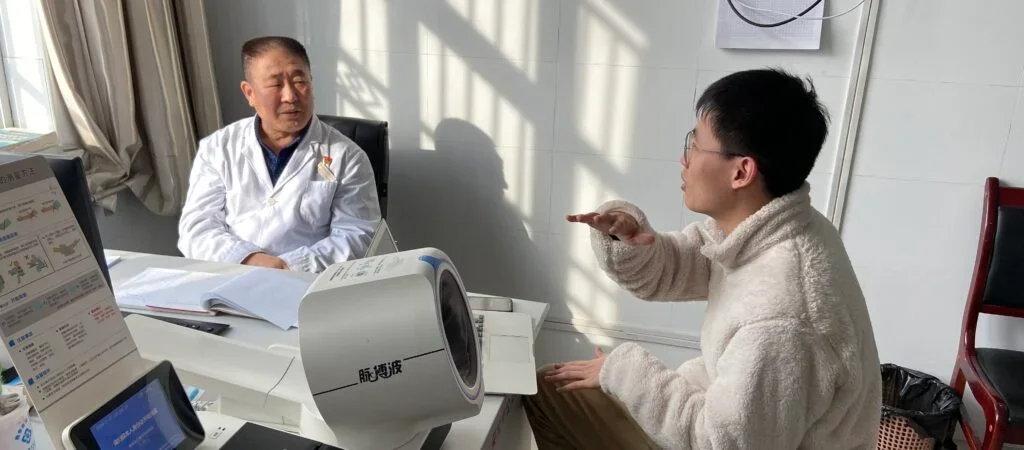
Integrated Care Pilot in Ningxia
Can a combination of provider payment, organization change, management and digital technology improve the implementation of integrated primary care in rural China?

Bureaucracy and Health Policymaking
How does bureaucratic behavior influence health policymaking and implementation in China?


