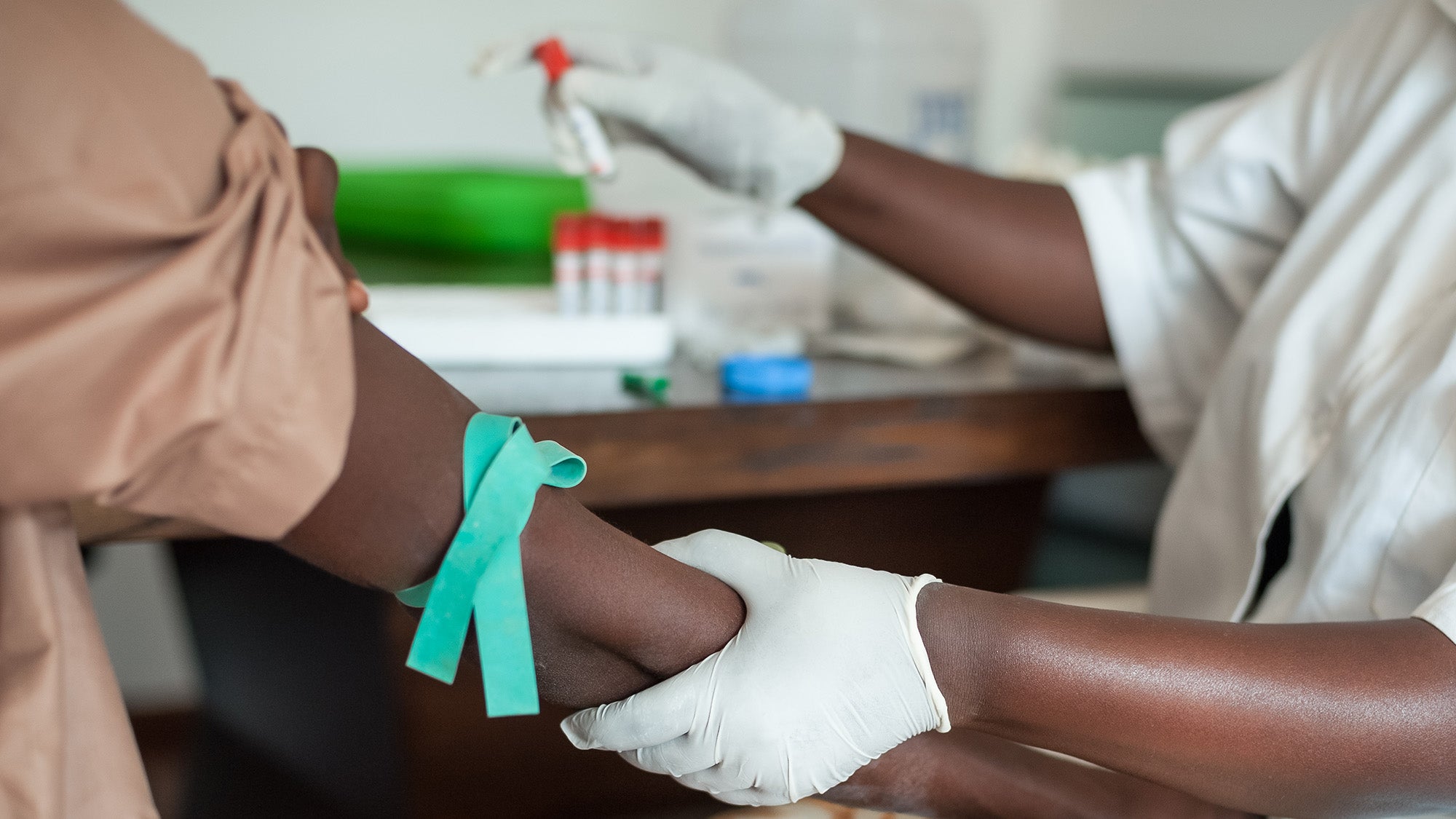
Bridging the Know-Do Gap
Ariadne Labs’ Better Evidence program brings the most up-to-date clinical knowledge to health care providers in resource-poor countries.
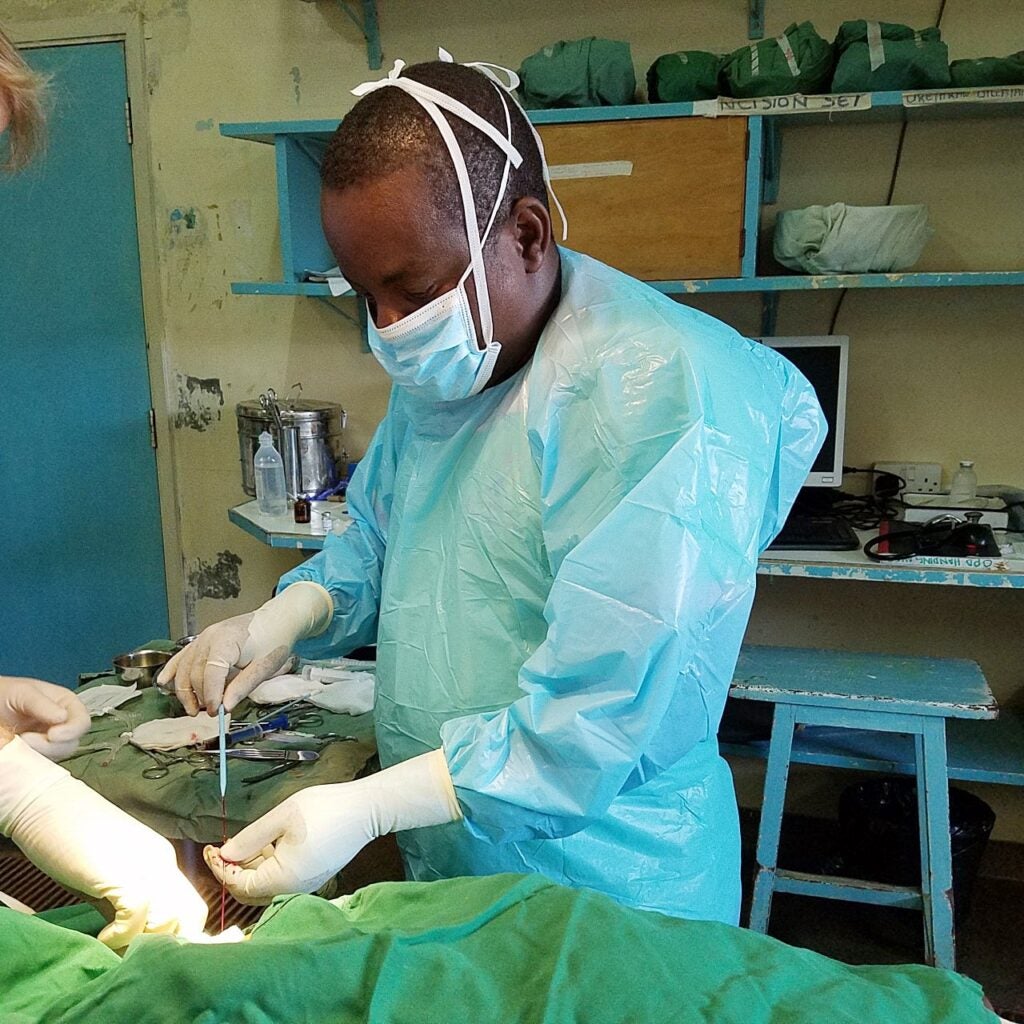
A surgeon at Rwinkwavu Hospital in Rwanda
A pickup truck slowly negotiated a red dirt road in the savannah of eastern Rwanda, hours from the capital city of Kigali. Seated in front of the jostling vehicle, a young internist at Boston’s Brigham and Women’s Hospital was carrying a hidden treasure. It was 2009, and Rebecca Weintraub was headed for Rwinkwavu Hospital, a rural district facility built on the side of a steep hill in one of the poorest areas of the East African nation. She was traveling light, with just a few changes of clothes, a stethoscope, a laptop, and a DVD.
In Boston, Weintraub was accustomed to working in a world-class institution chockablock with advanced technology and highly trained subspecialists. On the unpaved stretch of road approaching Rwinkwavu, she says, “You realize that you are isolated from the infrastructure and expertise of a tertiary care hospital.” When she arrived at her destination, she found a women’s ward, a men’s ward, a pediatrics ward, and an emergency ward, each packed with three rows of 10 to 12 beds in which patients awaited triage, suffering from an array of yet-to-be-diagnosed conditions.
Weintraub’s treasure: the DVD. She slid it into her laptop. The screen lit up with one of the most comprehensive diagnostic and treatment guides in medicine. Called UpToDate, the software is produced by Wolters Kluwer, a global information services company for clinicians. Physicians clustered around Weintraub. Together, they commenced rounds, moving in a knot from one bed to another, starting with the sickest patients. A group of nurses joined in the teaching rounds.
Some of the patients’ diseases the doctors knew well: malaria, HIV/AIDS, tuberculosis. Others were more baffling or unfamiliar. Full-body swelling with massive, painful tumors. Seizures stemming from undiagnosed epilepsy in patients who had been told that their symptoms were psychiatric in origin. Warning signs of heart attack and stroke. Uncontrolled bleeding from injuries. Weintraub helped the physicians diagnose these cases and devise treatment plans.
And Weintraub was herself a student. One 16-year-old was afflicted with a condition that Weintraub, with more than a decade of training, had never encountered: Pott’s disease, a form of end-stage tuberculosis that attacks the spine. “I was reading along with everyone else,” she says. “We were able to refer the patient. Within 48 hours, we had air-evac’d him to India to see a neurosurgeon.”
Over the next few days, guided by UpToDate, “We covered a diverse set of topics,” Weintraub says, from oncology to neurology to rheumatology. “As soon as I turned on my computer, the clinicians were immediately interested. They were excited, eager, engaged, curious, because this is a phenomenal tool in the midst of decision making. And their ability to navigate it was immediate.”
That’s when Weintraub had an insight: “We can scale this.” The more providers who had UpToDate, the more lives would be saved and suffering averted.

Rebecca Weintraub, Director, Better Evidence Program (right) with Peter Bonis, Chief Medical Officer of Clinical Effectiveness, Wolters Kluwer Health
Returning to Boston, Weintraub and other global health physicians met with leaders of Wolters Kluwer, including Denise Basow (now president and chief executive officer of the clinical effectiveness business unit) and Peter Bonis (now chief medical officer of clinical effectiveness). The company had already been making UpToDate donations through organizations and individual requests, but found that process needed to be more transparent. The group learned that simply making a donation did not necessarily translate into providers adopting the service—and thus did not have the desired impact. Basow and Bonis enthusiastically agreed with Weintraub’s proposal on how to scale up and drive adoption in low-resource settings.
“We had a mission-driven organization that wanted to provide UpToDate to those who needed it. Rebecca introduced herself as a social entrepreneur. She knew how to scale up and drive adoption with boots on the ground and had an organization to back her up,” recalls Bonis. “We were two sides of the same coin. We each offered what the other didn’t. A partnership was born immediately.”
As was a small revolution in global health: the Better Evidence program. Originally under the auspices of Harvard University’s Global Health Delivery Project, Better Evidence is now housed at Ariadne Labs, a joint health-systems-innovation center of Brigham and Women’s Hospital and the Harvard T.H. Chan School of Public Health.
Quality of care is as important as access
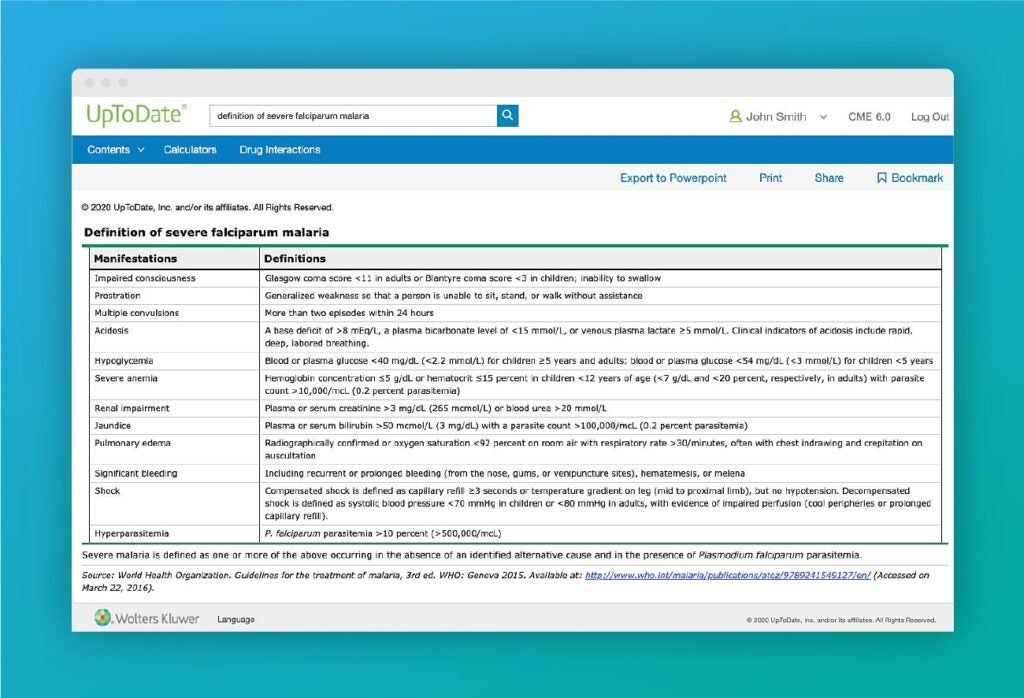
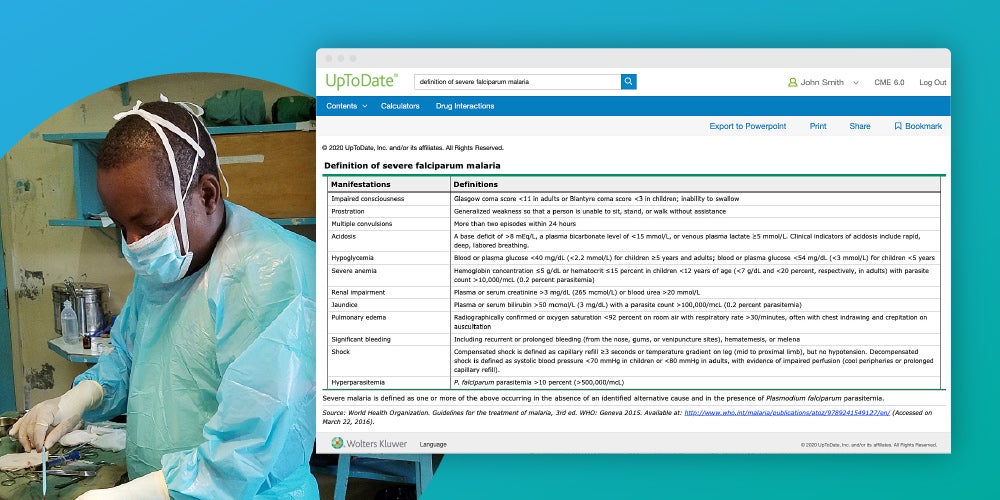
UpToDate’s page describing the symptoms of malaria caused by the parasite Plasmodium falciparum, which accounts for the vast majority of malaria infections worldwide. Malaria killed an estimated 405,000 people globally in 2018.
For health care providers everywhere, keeping up with current science is a formidable task. More than 2.5 million new research articles are published annually. A 2019 article in BMJ Open—co-authored by Weintraub, who directs Better Evidence, and Julie Rosenberg, the program’s assistant director— described the problem. Over the previous three years alone, they wrote, more than 16,000 unique clinical studies had posted new results on ClinicalTrials.gov—more facts than any one person could ever keep up with, let alone retain.
In low- and middle-income countries (LMICs), where the median per-capita health spending is $100, the challenge of keeping up with clinical advances is even more daunting. Health care providers often lack access to journals and other resources, because the price of such subscriptions is out of reach. Yet unlike their counterparts in high-income countries, physicians in LMICs care for more patients with a broader range of complaints—from infectious diseases such as malaria and tuberculosis to a rising caseload of noncommunicable diseases such as cancer, diabetes, and stroke. The shortage of specialist colleagues makes the job even more difficult. Rwanda, for example, had until recently only 15 anesthesiologists, 25 obstetricians, and no neurologists—for an entire country of some 12 million people.
To compensate for these shortfalls, many doctors end up resorting to sources of information that are often unreliable, such as Google, YouTube, and Wikipedia. As a result, millions of patients every year receive inaccurate or delayed diagnoses and substandard care.
In global health, the failure to translate what is known to work into the care that patients receive is dubbed the “know-do gap”—and it may be the biggest hurdle to achieving health equity around the world. According to a 2018 report from the Lancet Global Health Commission, “Poor-quality care is now a bigger barrier to reducing mortality than insufficient access.”
Weintraub’s insight about scalability was in line with the vision of Atul Gawande, MPH ’99, professor in the Department of Health Policy and Management at the Harvard Chan School, a surgeon at Brigham and Women’s Hospital, and founder and chair of Ariadne Labs. At Ariadne, Gawande’s aim has been to develop simple, scalable solu- tions to improve health care delivery at critical moments in people’s lives—such as during childbirth, surgery, or end of life—by changing habitual clinical practices.
A new learning paradigm
Better Evidence was launched in 2009, with the goal of bridging the know-do gap. Wolters Kluwer, along with Weintraub and her colleagues at the Global Health Delivery Project, with support from Brigham and Women’s Division of Global Health Equity, have brought free UpToDate subscriptions to more than 20,000 qualified health professionals in some 150 countries. The program has since expanded to 21 medical schools and affiliated training facilities in sub-Saharan Africa. Among the professionals who have received the subscriptions: physicians, medical students, nurses, midwives, pharmacists, and even medical school librarians.
UpToDate synthesizes the latest clinical evidence in forms that are easily actionable, including text, charts, photos, and illustrations. No longer confined to a DVD, it is now available online and for download on any digital device, including a tablet or smartphone. Its content is authored by leading physicians and distilled into graded, evidence-based recommendations. Continuous publication means it is always current. More than 200 studies have shown that UpToDate use improves diagnostic accuracy, lowers mortality, and reduces hospital readmissions. In the U.S., as of February 2018, 90 percent of teaching medical institutions and every one of the top 20 medical schools subscribed to the service.
The ubiquity of UpToDate reflects a new paradigm in medical education: de-emphasizing the passive presentation of material by a human lecturer and instead promoting online problem-solving skills and the ability to find information and adapt it to the clinical situation at hand.
In Rwinkwavu Hospital and every other place that the Better Evidence team has visited, physicians were primed to adopt the new digital tool. “People found us through word of mouth,” says Rosenberg. “They’re the positive outliers, the early adopters who are seeking to improve their practice.”
Adds Weintraub: “They were already digitally savvy, because they had been connecting to the internet for personal reasons for a long time. In Rwanda, getting a medical degree is a five-year process that begins at age 18 or 19. We were working with 23-year-old men and women who had a high level of motivation, a strong sense of self-efficacy and problem solving. There was no need for orientation.” But it is not just young clinicians who have embraced UpToDate—providers as old as 80 have subscribed.
According to Weintraub, UpToDate fits well in the current ethos of global health. “I always think of conversations from our mentors who developed global missions around essential medicines, essential diagnostics,” she says. “I view this as essential evidence.”
Better Evidence has collected countless stories from physicians attesting to UpToDate’s impact. A doctor in India described how vital information on COVID-19 was critical to planning and to preparing the workforce for the pandemic. A doctor in South Africa described halting an outbreak of chickenpox in a maternity ward. Another in Tanzania saved a newborn suffering from respiratory distress and heart problems. In Nepal, physicians changed their antibiotic prescription protocols to reduce drug resistance. In Afghanistan, where a new mother complained of stomach pains and assured her physicians that she could not possibly be pregnant again, doctors concluded that she was suffering from a ruptured ectopic pregnancy—and performed emergency surgery that saved her life.
Weintraub says she is inspired daily by the feedback she gets from Better Evidence beneficiaries. Typical is a 2018 note she received from a provider in Uganda: “This past October, we had a patient arrive with high fever and general body aches, soon followed by skin bruising and epistaxis. We used Better Evidence to look at the possible differential diagnosis and suspected hemorrhagic fever. We had no experience with this disease before, and would not have recognized it without the help of the tool. The Ugandan authorities were alerted—and arrived quickly. This case was finally diagnosed as the first case of Crimean-Congo Hemorrhagic Fever (CCHF) in Uganda in the past 4 years. Following the quick diagnosis, the source of the infection was traced, and an epidemic was prevented.”
Knowledge is self-empowerment
According to Rosenberg, access to UpToDate’s wealth of specialty information has enabled doctors to “practice beyond their normal scope and expand what they can do. That increases job satisfaction, because they feel like they have what they need to practice at the top of their game.” That, in turn, means less brain drain and burnout. It also means lower health care costs.
But the benefits extend even further. “We found that professionals sometimes use what they learn on UpToDate to advocate for better policy or to demand that the country purchase different drugs or acquire new supplies,” says Rosenberg. In Egypt, doctors persuaded the ministry of health to purchase UpToDate for all public health care facilities. “This informs policy, practice, and guidelines that countries are creating,” says Rosenberg. “While this does not take the place of official World Health Organization (WHO) recommendations, it allows the evidence to turn into action much faster.”
Such transformations dispel the misconceptions and prejudices that health professionals in affluent nations may harbor about providers in resource-starved countries. “People assume that physicians in LMICs are not practicing with the same standards,” says Rosenberg. “But everyone’s trying their best. They want to do as well as they can by their patients, no matter where they are.”
Indeed, Better Evidence users in LMICs have contributed crucial front-line knowledge to expand and refine UpToDate’s global health content on topics ranging from Ebola, HIV, and severe malaria to child malnutrition, snakebites, and arthropod-borne viruses that cause encephalitis. As Weintraub explains, “Clinical expertise is sitting geographically afar from where UpToDate is being edited—with clinicians who are close to the presentation of the disease. It is a reminder that there’s tremendous expertise that’s globally distributed. And any piece of software gets better when you have more people using and contributing to the platform.”
Weintraub adds that this global process of continually tweaking content “is at the intersection of clinical medicine and public health. Diagnostic inaccuracy and suboptimal treatment are probably the reason why we have antibiotic resistance and why we miss pandemics.”
Consider the 2014–2016 Ebola virus epidemic in West Africa—the largest Ebola outbreak in history, with 28,616 cases and 11,310 deaths across Guinea, Liberia, and Sierra Leone. In March 2014, WHO reported the first known cases in a rural region of southeastern Guinea and officially declared an epidemic.
But as a Better Evidence study of clickstream data from UpToDate later found, providers in the Ebola- affected regions had been conducting searches on Ebola 100 days before WHO reported its first case—suggesting that UpToDate has a place in public health surveillance. “It’s a vital signal to use in addition to epidemiologic modeling,” says Weintraub. “Front-line providers are sensitive signal nodes for epidemics.”
Justice Warriors
Both Weintraub and Rosenberg view WARRIORS UpToDate as a first step in bringing evidence-based diagnostic assistance to the places that need it most—a step toward more equitable care around the world. Weintraub would like to see such tools embedded in WHO and ministry of health protocols, just like other clinical checklists. “A physician checks the evidence, certifies the diagnosis with the evidence, and the patient asks for and receives confirmation that the evidence was checked.”
Other tools coming into use or in the pipeline include products that connect isolated primary care providers to specialists, either digitally or through online networks—in a kind of virtual consultation—and visual encyclopedias to sharpen diagnosis and treatment. On the hardware side, drones are now delivering essential products to hard-to-reach health facilities.
The biggest innovation, however, may not be technological but philosophical. Philanthropies underwrite the Better Evidence program, and Wolters Kluwer has supplied more than an estimated $7 million worth of in-kind donations, in the form of subscriptions. Yet until recently, many public health professionals distrusted the idea of such public-private partnerships. “For so many years in public health and global health, we’ve shunned the private sector. We turned our heads the other way and said, ‘You’re part of the problem of inequity, you’re part of the problem of corporate greed,’” says Rosenberg. “What’s innovative is bridging that gap.”
But changing her colleagues’ mindsets hasn’t been easy, Rosenberg concedes. “We need to convince our academic friends and philanthropic donors that this is a valid initiative, a proven intervention, just like any drug that we may distribute. In the same way that a pharmaceutical company may donate medicine to save lives, this tool saves lives.” She adds: “In any corporate social responsibility project, there are going to be benefits to a company. Otherwise, why would they do it? But that’s not the worst thing in the world. There has to be something in it for every stakeholder involved. Global health is not a zero-sum game. Benefits to one partner need not come at the expense of another.”
Access to UpToDate is not a panacea for the deep- rooted problems of delivering quality care in LMICs. “It doesn’t take away the need for well-trained, empa- thetic, caring providers who know how to act quickly in an emergency, how to scale up, how to triage cases. UpToDate will not solve the health care workforce crisis and shortage,” says Rosenberg. “It’s an immediate solu- tion for immediate needs.”
“I think of health equity as lowering the fence for everyone, so that more people can thrive,” adds Weintraub. “My theory of change for Better Evidence has been: If we can equip the provider with the essential evidence they need, we will be able to expand their scope and quality of practice, especially those caring for the most vulnerable populations. And that, in and of itself, will lead to greater demand for the drugs and diagnostics and other elements in health care systems that these providers are ready and prepared to offer. It will create a generational effect.
“We’ve learned from experiences in the midst of pandemics and epidemics that local providers are the justice warriors. This is an essential piece of gear to help them in their mission.”
— Madeline Drexler is editor of Harvard Public Health.