April 25, 2016 — Projects led by Harvard T.H. Chan School of Public Health students—one that trains Indian girls as peer health educators and another that aims to use technology to allow patients and their loved ones to interact with their hospital care in real-time—were among the 10 finalist teams in this year’s President’s Challenge.
Now in its fifth year, this competition gives students from across the University and others the chance to turn their venture ideas into fully-formed businesses. Finalists receive funding, mentorship, and access to the resources of the Harvard Innovation Lab (i-lab). A grand prize pool of $100,000 was split between the winning team and three runners up April 25 at the Challenge’s Demo Day showcase.
Peer education program Girls Health Champions was one of the runners up and the team received $10,000.

Girls Health Champions
Priya Shankar, MPH ’16, first visited India on a service trip when she was 13, and the experience launched a commitment to serving girls and women that became a driving force in her life for the next 14 years. She has been back to the country more than 20 times since then, first as a volunteer teacher and later as a Fulbright Scholar researching maternal and child health and nutrition policy.
Over the years, Shankar—who will also receive an MD next spring from Boston University School of Medicine—observed how some of the country’s societal norms can negatively affect a women or girls’ health and opportunities, from menstrual taboos that keep girls home from school to the belief that husbands have the right to beat their wives. Topics like these are often not addressed in schools or discussed between parents and children. But Shankar believed that if girls were given the information they could teach and support each other.
She developed Girls Health Champions, a peer-to-peer health curriculum that was piloted at an all-girls school in India in January. The initiative was conducted with the support of Harvard Chan’s Maternal Health Task Force and the Public Health Research Institute of India.
Eighteen girls were randomly selected to serve as “Champions” from a group of 68 ninth-grade students participating in the program. They spent a week learning the curriculum, which included nutrition and anemia, mental health and gender-based violence, menstruation and reproductive anatomy, and reproductive health, and then taught it to their classmates. All of the students were tested on their knowledge of the material before and after the program was implemented. At the start, the Champions scored 55% and the rest of the class scored 68%; at the end, they all scored 96%.
Shankar and her teammate and fiancé Ricky Sharma, a Harvard Kennedy School student and financial professional, plan to roll out the program to 10 to 20 more schools in India this summer and will study whether the training has any long-term effects on the girls’ health, self-esteem, and leadership. They hope to build a sustainable program in which each group of Champions trains the next year’s class of Champions, and plan to focus on girls in grades 8 to 10. They ultimately hope to expand the program to other developing countries.
While Girls Health Champions is the culmination of many years of work, Shankar credits the support she has received at Harvard Chan—particularly from Ana Langer, professor of the practice of public health and head of the School’s Women and Health Initiative, and Gordon Bloom, lecturer in health policy and management and director of the Social Entrepreneurship Collaboratory at Harvard, with helping her turn her idea into reality.
She’s still amazed at the program’s success. “As I watched the first class the girls taught, I couldn’t believe it. They did an amazing job and they were so brave. That was the moment when I said that this is a real thing and it can work.”
Patient-centered app

Physician Joe Fitchett, DrPH ’18, loved his work on the health care frontlines at St. Thomas’ Hospital in London, where he trained in internal medicine and infectious diseases, but he often found himself frustrated by old-fashioned and inefficient administrative systems. Much of each ward’s key logistical information—such as medications to administer or number of available beds—was still recorded in paper notebooks and on the whiteboards posted at nurses’ stations. Even when computer systems were available, there were no ways to share information and progress with patients and their loved ones.
Fitchett wants to seamlessly blend technology into hospital culture. When he came to Harvard Chan last year to study infectious disease epidemiology, he brought along a project he started developing in London with friend Ben Thomas, a business analyst. Thomas was in and out of the hospital over several years for a knee injury and saw firsthand the asymmetry in information between hospital staff and patients. He and Fitchett reasoned that there must be a way to allow patients and their loved ones to view, follow, and interact with their hospital care.
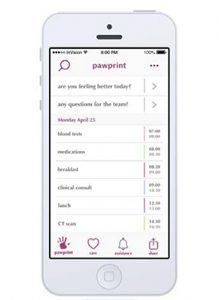
Fitchett and Thomas’ platform, pawprint, is a mobile and tablet app that channels data from hospital servers and the cloud into a patient’s handheld device. The pawprint app enables patients to know what is happening in real-time and access personalized information to understand their hospital care, free up staff to deliver quality care, and allow loved ones who cannot be in the hospital to follow and connect remotely. The technology will be tested and implemented in London and Boston.
Fitchett and Thomas hope to combine the software with a high-tech version of the well-known patient identification wristband. Tracking technology in each wristband and on each bed would communicate with a central hospital dashboard, allowing staff to quickly see that a patient is in another part of the hospital getting a test or that a bed is now available. It will also be connected to the pawprint app that staff can use to enter and view tasks that need to be completed for each patient.
Moving forward, Fitchett hopes to find more ways to tap technology to improve public health. He said that he has been inspired by work at the School in this area, such as using Big Data to track epidemics.
In the meantime, he’s enjoyed the opportunity to learn from his fellow President’s Challenge competitors, as well as the mentors at the i-lab. “It’s been amazing to work with peers and get different perspectives and approaches. We’re absolutely delighted and humbled to have this opportunity.”
This story was updated with competition results on April 26.
Photos: (1) courtesy of Priya Shankar; (2) courtesy of Harvard iLab; (3) Sarah Sholes; (4) courtesy of Joe Fitchett
