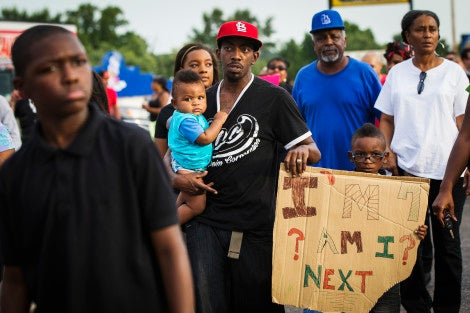In 2014, the police killings of three unarmed African-American males—Eric Garner in Staten Island, New York; Michael Brown in Ferguson, Missouri; and Tamir Rice in Cleveland, Ohio— sparked a national conversation on police brutality and on endemic racism in U.S. society. Biostatistician Melody Goodman, SM ’03, PhD ’06, assistant professor in the division of public health sciences at Washington University School of Medicine in St. Louis, focuses her work on the social risk factors behind health disparities. She spoke recently with Madeline Drexler, editor of Harvard Public Health.

Q: If you could design a public health study that illuminated the causes and effects of police-associated violence, what would you do?
A: I would do two studies. First, we don’t have consistently collected data across police departments and across states about exactly what’s happening. So I would collect surveillance data that we could monitor over time. Whenever there is an interaction between a police officer and a community member and someone gets hurt, we would ask each party and all witnesses—using a standardized data collection instrument—what happened and whether any weapons were involved. It should be mandatory that police departments collect and report these data at the local, state, and national levels.
We also don’t know how aggressive policing affects the health of African-Americans, especially men— both physical health and social well-being. So the other study would be a mixed-method, qualitative-quantitative study that compares the health effects of community policing—the model where police officers focus on building partnerships and working closely with community members to address conditions that lead to public safety issues—with the militarized police model used in many urban centers.
African-American men, and especially youths, often assume that at some point they will land in jail, even if it’s just overnight to pay a fine. To be in an environment where you don’t trust the institutions that are designed to protect and serve—police, criminal justice, medical—makes you go through life in a different way.
Q: When you saw videotapes of the deaths of Eric Garner, Michael Brown, and Tamir Rice, what was your response?
A: As an African-American woman who grew up on the south side of Jamaica, Queens, in a New York City housing project, seeing aggressive police tactics is not surprising to me. It happened all the time when I was a kid, which was at the height of the crack epidemic and the resulting “war on drugs.” This is what drove me into public health: being from a community where it’s clear how social determinants impact health outcomes.
I felt the national debate was polarizing. On the one hand, it was good that there were more discussions about what it is like to be a black youth in this country. But no one talked about the privileges that come with being a white police officer. For example, most people wanted to believe the police officers and discredit the witnesses. No one talked about the officers’ inherent biases. Even the idea that black men are perceived as threats is a bias. The killing of Tamir Rice—who was 12 years old—is a perfect example of bias.
Q: Why are we more comfortable discussing black victimization than white privilege?
A: The people who are now benefiting from white privilege didn’t set up this system, and they don’t want to be penalized for how it was set up before. It’s not that I think that they should be, but we don’t even talk about it.
I remember the first time I saw a white person curse at a police officer. I was shocked. I thought, “Here it goes, something terrible is going to happen.” But nothing happened. My mom didn’t call it “white privilege”—we didn’t have that language—but she made me aware that I could not behave like that, because of my skin color.
Or take the hashtag “#blacklivesmatter.” It’s about priorities. When I write proposals to do my disparities work, stating that blacks are underserved is not enough to pull in funding. I have to show how my work will benefit the whole community and often make an economic argument to do so.
Q: What does it say about our society that there are so few public health studies of police violence?
A: It says that we’re not allowed to question or criticize police departments. As scholars, we get criticized on a daily basis—it’s part of what we do. In the culture of policing, you are seen as either pro-police or anti-police.
I’ve told my colleagues that I wish police officers could live in an academic environment for just one year, where everything they did got critiqued. It changes your mentality about what criticism really means. I would love to be able to say, “This study of mine is not open for criticism!” But when I get feedback on a paper, it’s not that people are criticizing me as a person— they’re just trying to help me build a stronger scientific case. I’ve learned to use criticism to make my work better.
I wish police departments would open themselves up for constructive criticism. I am not saying they will enjoy it, but they will be better for it.
— Madeleine Drexler is editor of Harvard Public Health
Learn More
Florida’s ‘Stand Your Ground’ Convictions Have Racial Bias (Washington University School of Public Health)
Photo: Courtesy of Melody Goodman