Verguet Lab
Projects under Stéphane Verguet
Stéphane Verguet is an Associate Professor of Global Health in the Department of Global Health and Population at the Harvard T.H. Chan School of Public Health and a core faculty member of Harvard University’s Center for Health Decision Science. His research concerns health systems, health economics, and priority setting, with significant contributions toward incorporating dimensions of equity into the economic evaluation of health policies and priority setting through the modeling of health benefit packages and intersectoral interventions, via applied economic evaluations. He has co-chaired the Analytics & Metrics Community of Practice of the Research Consortium for School Health & Nutrition since 2021 and has contributed to the World Bank’s Disease Control Priorities since 2009, most recently as a lead editor for the Universal Health Coverage volume of its fourth edition. He was also a Commissioner of The Lancet Global Health 2050 Commission. Verguet has degrees from the University of California, Berkeley, and the École Polytechnique and was previously on the faculty of the University of Washington.
Projects
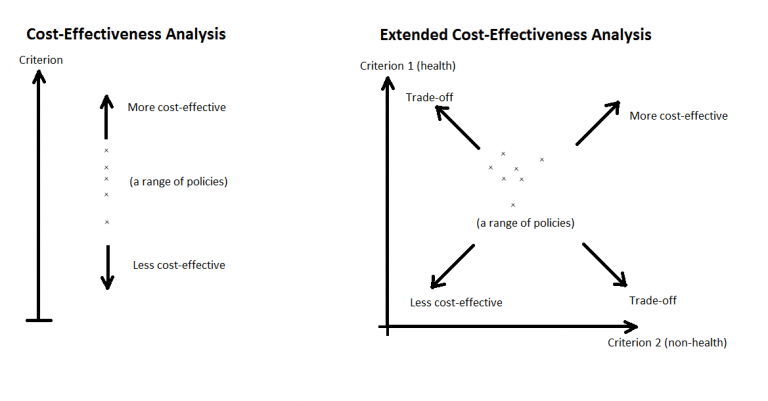
Extended Cost-Effectiveness Analysis (ECEA) is a form of quantitative economic analysis that assesses the health and financial impact of health policies. It is an expansion of cost-effectiveness analysis, which compares the relative costs and gains in health outcomes (in the form of years of life saved, premature deaths averted, quality- or disability-adjusted life years gained/averted, etc.) of interventions. ECEA also includes non-health benefits such as financial risk protection and distributional consequences like equity in the economic evaluation of health policies. This enables health policy makers to take into account multiple criteria and make trade-offs among competing demands (see Figure 1).
The fundamental aim of health policies is to improve health outcomes (e.g. reduction in premature mortality and morbidity) at the population level. However, health policies can provide other benefits, extending to other sectors than the sole health sector. An important non-health benefit of such policies is the provision of financial risk protection (FRP), or the reduction of individuals’ and households’ impoverishment; in addition to improved health equity among the population by providing progressive redistribution of the health benefits and impoverishment averted (see Figure 2).
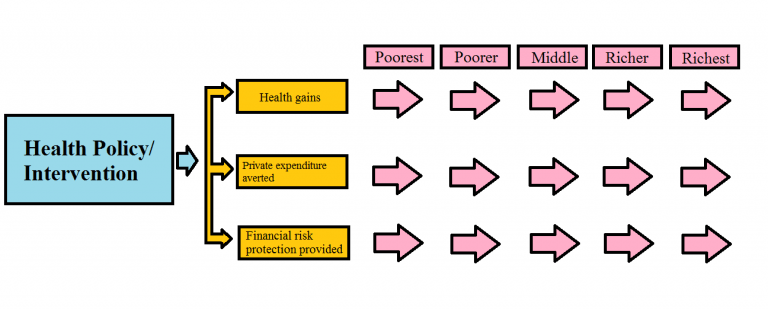
ECEA presents the assessment of health policy in three domains: 1) health gains, 2) private expenditures averted, and 3) FRP; all per population subgroup (e.g. income quintile, geographical setting). Additionally, with the total costs of the policy assessed, we can calculate the outcomes of health gains and financial protection per dollar expenditure. In this respect, using ECEA, every policy/intervention can be placed in a two-dimensional space by 1) health benefits per dollar expenditure and 2) FRP per dollar expenditure (Figure 1). Policy makers can then visually compare different policies/interventions, taking into account multiple criteria in the decision-making process.
More broadly, the added dimension of assessment outside of the health sector is not limited to financial benefits, but could also include educational, agricultural, environmental benefits, to name a few. ECEA not only can assess the equity between different income quintiles, but also the disaggregation of any type, geographically and demographically.
Below is a selection of recently published ECEA studies:
| Topic | Policy instrument | Country | Publication(s) |
| Expanding surgical access | Task sharing, public finance | Ethiopia | [2] |
| Home-based neonatal care package | Public finance | India | [3,4] |
| Diarrhea and pneumonia treatment | Public finance | Ethiopia | [5-8] |
| Human papillomavirus vaccination to prevent cervical cancer | Public finance | China | [9] |
| Universal coverage for mental, neurological, and substance use disorders | Public finance | Ethiopia, India | [10-13] |
| Selected ECEAs for cardiovascular diseases | Public finance of interventions, tobacco taxation, regulation of salt | China, Ethiopia, South Africa | [14-16] |
| Motorcycle helmet laws | Regulation | Vietnam | [17] |
| Use of liquefied petroleum gas and other clean energy sources in household | Commodity subsidy | India | [18] |
| Postponing adolescent parity | Education | India, Niger | [19] |
| Tuberculosis treatment | Universal public finance; policies to improve ease of borrowing for treatment costs | India | [20] |
| Measles vaccine | Conditional cash transfers | Ethiopia | [21] |
| Universal immunization | Public finance | India | [22] |
| Water and sanitation | Clean piped water and improved sanitation | India | [23] |
| Tobacco | Taxation | China, Lebanon, Armenia | [16, 24-25] |
| Rotavirus vaccine | Public finance | India, Ethiopia, Malaysia | [5,26] |
*This list is adapted from: Verguet and Jamison. 2018. Chapter 8. Health policy analysis: applications of extended cost-effectiveness analysis (ECEA) methodology in DCP3. In: Jamison DT, Nugent R, Gelband H, Horton S, Jha P, Laxminarayan R, eds. Disease Control Priorities. Volume 9: Disease control priorities, improving health and reducing poverty. Washington, DC: World Bank 2018.
References
- Verguet, S., Kim, J.J. and Jamison, D.T., 2016. Extended cost-effectiveness analysis for health policy assessment: a tutorial. Pharmacoeconomics, 34(9), pp.913-923. https://link.springer.com/article/10.1007/s40273-016-0414-z
- Shrime, M.G., Verguet, S., Johansson, K.A., Desalegn, D., Jamison, D.T. and Kruk, M.E., 2015. Task-sharing or public finance for the expansion of surgical access in rural Ethiopia: an extended cost-effectiveness analysis. Health policy and planning, 31(6), pp.706-716. https://academic.oup.com/heapol/article/31/6/706/1749643/Task-sharing-or-public-finance-for-the-expansion
- Ashok, A., Nandi, A., and Laxminarayan, R. (2016). The Benefits of a Universal Home-Based Neonatal Care Package in Rural India: An Extended Cost-Effectiveness Analysis. In Disease Control Priorities, Third Edition (Volume 2): Reproductive, Maternal, Newborn, and Child Health, pg 335 – 344. https://elibrary.worldbank.org/doi/abs/10.1596/978-1-4648-0348-2_ch18
- Nandi, A., Colson, A.R., Verma, A., Megiddo, I., Ashok, A. and Laxminarayan, R., 2015. Health and economic benefits of scaling up a home-based neonatal care package in rural India: a modelling analysis. Health policy and planning, 31(5), pp.634-644. https://academic.oup.com/heapol/article/31/5/634/2355739/Health-and-economic-benefits-of-scaling-up-a-home
- Verguet, S., Murphy, S., Anderson, B., Johansson, K.A., Glass, R. and Rheingans, R., 2013. Public finance of rotavirus vaccination in India and Ethiopia: an extended cost-effectiveness analysis. Vaccine, 31(42), pp.4902-4910. http://www.sciencedirect.com/science/article/pii/S0264410X13009389
- Johansson, K.A., Memirie, S.T., Pecenka, C., Jamison, D.T. and Verguet, S., 2015. Health gains and financial protection from pneumococcal vaccination and pneumonia treatment in Ethiopia: results from an extended cost-effectiveness analysis. PloS one, 10(12), p.e0142691. http://journals.plos.org/plosone/article?id=10.1371/journal.pone.0142691
- Pecenka, C.J., Johansson, K.A., Memirie, S.T., Jamison, D.T. and Verguet, S., 2015. Health gains and financial risk protection: an extended cost-effectiveness analysis of treatment and prevention of diarrhoea in Ethiopia. BMJ open, 5(4), p.e006402. http://bmjopen.bmj.com/content/5/4/e006402
- Verguet, S., Pecenka, C., Johansson, K.A., Memirie, S.T., Friberg, I.K., Driessen, J.R. and Jamison, D.T., 2016. Health Gains and Financial Risk Protection Afforded by Treatment and Prevention of Diarrhea and Pneumonia in Ethiopia: An Extended Cost-Effectiveness Analysis. Reproductive, Maternal, Newborn, and Child Health. In Disease Control Priorities (third edition): Volume 2, Reproductive, Maternal, Newborn, and Child Health, edited by R. Black, R. Laxminarayan, M. Temmerman, and N. Walker. Washington, DC: World Bank. https://www.ncbi.nlm.nih.gov/books/NBK361923/
- Levin, C.E., Sharma, M., Olson, Z., Verguet, S., Shi, J.F., Wang, S.M., Qiao, Y.L., Jamison, D.T. and Kim, J.J., 2015. An extended cost-effectiveness analysis of publicly financed HPV vaccination to prevent cervical cancer in China. Vaccine, 33(24), pp.2830-2841. http://www.sciencedirect.com/science/article/pii/S0264410X15002418
- Chisholm, D., Johansson, K.A., Reykar, N., Megiddo, I., Nigam, A., Strand, K.B., Colson, A., Fekadu, A. and Verguet, S., 2016. Universal health coverage for mental, neurological, and substance use disorders: an extended cost-effectiveness analysis. In Disease Control Priorities (third edition): Volume 4, Mental, Neurological, and Substance Use Disorders, edited by V. Patel, D. Chisholm, T. Dua, R. Laxminarayan, and M. Medina-Mora. Washington, DC: World Bank. https://www.ncbi.nlm.nih.gov/books/NBK361946/
- Johansson, K.A., Strand, K.B., Fekadu, A. and Chisholm, D., 2016. Health Gains and Financial Protection Provided by the Ethiopian Mental Health Strategy: an Extended Cost-Effectiveness Analysis. Health policy and planning, 32(3), pp.376-383. https://academic.oup.com/heapol/article/2907867
- Megiddo, I., Colson, A., Chisholm, D., Dua, T., Nandi, A. and Laxminarayan, R., 2016. Health and economic benefits of public financing of epilepsy treatment in India: An agent‐based simulation model. Epilepsia, 57(3), pp.464-474. http://onlinelibrary.wiley.com/doi/10.1111/epi.13294/full
- Raykar, N., Nigam, A. and Chisholm, D., 2016. An extended cost-effectiveness analysis of schizophrenia treatment in India under universal public finance. Cost Effectiveness and Resource Allocation, 14(1), p.9. https://resource-allocation.biomedcentral.com/articles/10.1186/s12962-016-0058-z
- Watkins, D.A., Olson, Z.D., Verguet, S., Nugent, R.A. and Jamison, D.T., 2015. Cardiovascular disease and impoverishment averted due to a salt reduction policy in South Africa: an extended cost-effectiveness analysis. Health policy and planning, 31(1), pp.75-82. https://academic.oup.com/heapol/article/31/1/75/2363529
- Verguet, S., Olson, Z.D., Babigumira, J.B., Desalegn, D., Johansson, K.A., Kruk, M.E., Levin, C.E., Nugent, R.A., Pecenka, C., Shrime, M.G. and Memirie, S.T., 2015. Health gains and financial risk protection afforded by public financing of selected interventions in Ethiopia: an extended cost-effectiveness analysis. The Lancet Global Health, 3(5), pp.e288-e296. http://www.sciencedirect.com/science/article/pii/S2214109X14703468
- Verguet, S., Gauvreau, C.L., Mishra, S., MacLennan, M., Murphy, S.M., Brouwer, E.D., Nugent, R.A., Zhao, K., Jha, P. and Jamison, D.T., 2015. The consequences of tobacco tax on household health and finances in rich and poor smokers in China: an extended cost-effectiveness analysis. The Lancet Global Health, 3(4), pp.e206-e216. http://www.sciencedirect.com/science/article/pii/S2214109X15700951
- Olson, Z., Staples, J.A., Mock, C., Nguyen, N.P., Bachani, A.M., Nugent, R. and Verguet, S., 2016. Helmet regulation in Vietnam: impact on health, equity and medical impoverishment. Injury prevention, 22(4), pp.233-238. http://injuryprevention.bmj.com/content/22/4/233
- Pillarisetti, A., Jamison, D.T. and Smith, K.R., 2017. Household Energy Interventions and Health and Finances in Haryana, India: An Extended Cost-Effectiveness Analysis. In Disease Control Priorities (third edition): Volume 7, Injury Prevention and Environmental Health, edited by C. N. Mock, O. Kobusingye, R. Nugent, and K. R. Smith. Washington, DC: World Bank. http://dcp-3.org/node/2506
- Verguet, S., Nandi, A., Filippi, V. and Bundy, D.A., 2016. Maternal-related deaths and impoverishment among adolescent girls in India and Niger: findings from a modelling study. BMJ open, 6(9), p.e011586. http://bmjopen.bmj.com/content/6/9/e011586
- Verguet, S., Laxminarayan, R. and Jamison, D.T., 2015. Universal public Finance of tuberculosis treatment in India: an extended cost‐effectiveness analysis. Health economics, 24(3), pp.318-332. http://onlinelibrary.wiley.com/doi/10.1002/hec.3019/full
- Driessen, J., Olson, Z.D., Jamison, D.T. and Verguet, S., 2015. Comparing the health and social protection effects of measles vaccination strategies in Ethiopia: An extended cost-effectiveness analysis. Social Science & Medicine, 139, pp.115-122. http://www.sciencedirect.com/science/article/pii/S0277953615003500
- Megiddo, I., Colson, A., Chisholm, D., Dua, T., Nandi, A. and Laxminarayan, R., 2016. Health and economic benefits of public financing of epilepsy treatment in India: An agent‐based simulation model. Epilepsia, 57(3), pp.464-474. http://onlinelibrary.wiley.com/doi/10.1111/epi.13294/full
- Nandi, A., Megiddo, I., Ashok, A., Verma, A. and Laxminarayan, R., 2017. Reduced burden of childhood diarrheal diseases through increased access to water and sanitation in India: A modeling analysis. Social Science & Medicine, 180, pp.181-192. http://www.sciencedirect.com/science/article/pii/S0277953616304853
- Salti, N., Brouwer, E. and Verguet, S., 2016. The health, financial and distributional consequences of increases in the tobacco excise tax among smokers in Lebanon. Social Science & Medicine, 170, pp.161-169. http://www.sciencedirect.com/science/article/pii/S0277953616305883
- Postolovska, I., Lavado, R.F., Tarr, G. and Verguet, S., 2017. Estimating the Distributional Impact of Increasing Taxes on Tobacco Products in Armenia. http://documents.worldbank.org/curated/en/604501492414938391/Estimating-the-distributional-impact-of-increasing-taxes-on-tobacco-products-in-Armenia-results-from-an-extended-cost-effectiveness-analysis
- Loganathan, T., Jit, M., Hutubessy, R., Ng, C.W., Lee, W.S. and Verguet, S., 2016. Rotavirus vaccines contribute towards universal health coverage in a mixed public–private healthcare system. Tropical medicine & international health, 21(11), pp.1458-1467. http://onlinelibrary.wiley.com/doi/10.1111/tmi.12766/full
The Disease Control Priorities-Ethiopia (DCP-E) project, sponsored by the Bill & Melinda Gates Foundation and implemented by the Harvard T.H. Chan School of Public Health and the University of Bergen, brings evidence and methods of priority setting and health economics closer to policy decision-making in Ethiopia.
Key Objectives
To achieve this purpose, three objectives are important:
- To develop health economic evaluation and priority setting capacity in Ethiopia.
- To provide input, through research and evidence, to the revision of the essential health services package for Ethiopia.
- To establish a process to support health priority setting in Ethiopia, including assessing the cost-effectiveness of selected health sector interventions, packages, and delivery platforms.
Key Activities
The project trains Ethiopian researchers and policymakers in health economics, decision sciences and priority setting. The training will enable them to generate an evidence base for designing, developing and implementing essential health services for the Federal Ministry of Health, and to help revise Ethiopia’s current essential health services package.
Some train as Master students, some as PhD students, while others receive in-service, profession development, and short-course training. The data generated by the student research provides the basis for evidence-based decision-making and priority setting.
Publications
- Assebe, L. F., Belete, W. N., Alemayehu, S., Asfaw, E., Godana, K. T., Alemayehu, Y. K., Teklu, A. M., & Yigezu, A. (2021). Economic evaluation of Health Extension Program packages in Ethiopia. PLOS ONE, 16(2), e0246207. https://doi.org/10.1371/journal.pone.0246207
- Eregata, G. T., Hailu, A., Stenberg, K., Johansson, K. A., Norheim, O. F., & Bertram, M. Y. (2021). Generalised cost-effectiveness analysis of 159 health interventions for the Ethiopian essential health service package. Cost Effectiveness and Resource Allocation, 19(1), 2.https://doi.org/10.1186/s12962-020-00255-3
- Eregata, G. T., Hailu, A., Geletu, Z. A., Memirie, S. T., Johansson, K. A., Stenberg, K., Bertram, M. Y., Aman, A., & Norheim, O. F. (2020). Revision of the Ethiopian Essential Health Service Package: An Explication of the Process and Methods Used. Health Systems & Reform, 6(1), e1829313. https://doi.org/10.1080/23288604.2020.1829313
- Bigelow, B., Desalegn, D., Salomon, J., & Verguet, S. (2019). Modeling hospital operations: Insight from using data from paper registries in the obstetrics ward at a hospital in Addis Ababa, Ethiopia. BMJ Global Health 4(3):e001281. https://gh.bmj.com/content/4/3/e001281
- Memirie, S, Tolla, M., Desalegn, D., Hailemariam, M., Norheim, O., Verguet, S., & Johansson, K. (2019). A cost-effectiveness analysis of maternal and neonatal health interventions in Ethiopia. Health Policy and Planning, 34(4), 289-297. https://academic.oup.com/heapol/article/34/4/289/5491503
- Memirie, S.T., Metaferia, Z.S., Norheim O.F., Levin C.E., Verguet S., Johansson K.A. (2017). Household expenditures on pneumonia and diarrhea treatment in Ethiopia: a facility-based study. BMJ Global Health 1:e000166. https://gh.bmj.com/content/2/1/e000166
- Tolla, M., Norheim, O., Verguet, S., Bekele, A., Amenu, K., Abdisa, S., & Johansson, K. (2017). Out-of-pocket expenditures for prevention and treatment of cardiovascular disease in general and specialised cardiac hospitals in Addis Ababa, Ethiopia: A cross-sectional cohort study. BMJ Global Health 2(2):e000280. https://gh.bmj.com/content/2/2/e000280
- Memirie, S.T., Verguet, S., Norheim, O.F., Levin, C., Johansson, K.A. (2016). Inequalities in utilization of maternal and child health services in Ethiopia: the role of primary health care. BMC Health Services Research 16:51. https://bmchealthservres.biomedcentral.com/articles/10.1186/s12913-016-1296-7
- Tolla, M.T., Norheim, O.F., Memirie, S.T., Abdisa, S.G., Ababulgu, A., Jerene, D., Bertram, M., Strand, K., Verguet, S., Johansson K.A. (2016). Prevention and treatment of cardiovascular disease in Ethiopia: a cost-effectiveness analysis. Cost Effectiveness and Resource Allocation 14:10. https://resource-allocation.biomedcentral.com/articles/10.1186/s12962-016-0059-y
- Verguet, S., Memirie, S.T., Norheim, O.F. (2016). Assessing the burden of medical impoverishment by cause: a systematic breakdown by disease in Ethiopia. BMC Medicine 14:164. https://bmcmedicine.biomedcentral.com/articles/10.1186/s12916-016-0697-0
- Johansson, K.A., Memirie, S.T., Pecenka, C., Jamison, D.T., Verguet, S. (2015). “Health Gains and Financial Protection from Pneumococcal Vaccination and Pneumonia Treatment in Ethiopia: Results from an Extended Cost-Effectiveness Analysis.”PLoS ONE 10 (12):e0142691. https://doi.org/10.1371/journal.pone.0142691
- Pecenka, C., Johansson, K., Memirie, S., Jamison, D., Verguet, S. (2015). Health gains and financial risk protection: An extended cost-effectiveness analysis of treatment and prevention of diarrhoea in Ethiopia. BMJ Open 5(4):006402. https://bmjopen.bmj.com/content/bmjopen/5/4/e006402.full.pdf
- Verguet, S., Olson, Z.D., Babigumira, J.B., Desalegn, D., Johansson, K.A., Kruk, M.E., Levin, C.E., Nugent, R.A., Pecenka, C., Shrime, M.G., Memirie, S.T., Watkins, D.A., Jamison, D.T. (2015). Health gains and financial risk protection afforded by public financing of selected interventions in Ethiopia: An extended cost-effectiveness analysis. The Lancet Global Health, 3(5), E288-E296. https://www.sciencedirect.com/science/article/pii/S2214109X14703468?via%3Dihub
- Verguet, S., Murphy, S., Anderson, B., Johansson, K., Glass, R., & Rheingans, R. (2013). Public finance of rotavirus vaccination in India and Ethiopia: An extended cost-effectiveness analysis. Vaccine, 31(42), 4902-4910. https://doi.org/10.1016/j.vaccine.2013.07.014
- Essential Health Services Package of Ethiopia. Federal Democratic Republic of Ethiopia, Ministry of Health. Essential Health Services Package of Ethiopia. Addis Ababa: Federal Democratic Republic of Ethiopia, Ministry of Health; 2019. https://www.hsph.harvard.edu/stephane-verguet/wp-content/uploads/sites/1834/2020/09/Essential_Health_Service_Package_Ethiopia_2019_0.pdf
Project Overview
The Disease Control Priorities-Ethiopia (DCP-E) project, sponsored by the Bill & Melinda Gates Foundation and implemented by the Harvard T.H. Chan School of Public Health and the University of Bergen, brings evidence and methods of priority setting and health economics closer to policy decision-making in Ethiopia.
Key Objectives
- To develop health economic evaluation and priority setting capacity in Ethiopia.
- To provide input, through research and evidence, that supports the revision of Ethiopia’s essential health services package.
- To support health priority setting in Ethiopia, including cost-effectiveness assessments of health sector interventions, packages, and delivery platforms.
Key Activities
The DCP-E project trains Ethiopian researchers and policymakers in health economics, decision sciences, and priority setting. Training enables participants to generate an evidence base that will inform the development, design, and implementation of essential health services, as well as recommendations for revisions to Ethiopia’s current essential health services package.
Some participants train as Master- or PhD-level students, while others receive in-service professional development and short-course training. The data generated by DCP-E research provides a foundation for evidence-based decision-making and priority setting in Ethiopia.
Download the Essential Health Services Package of Ethiopia.
Policy Briefs
- Moving towards universal health coverage in Ethiopia: A guide for revision of the essential health services package
- Reducing premature mortality in Ethiopia: Identifying where extra effort is needed
- Catastrophic out-of-pocket expenditure related to seeking health services for cardiovascular disease in Ethiopia
- Estimating cancer incidence to improve cancer control programs and coverage in Ethiopia
- The Potentially large health and financial risk protection benefits of universal public finance
- Economic burden of malaria for rural households in Ethiopia
- Prevention and treatment of cardiovascular disease in Ethiopia: A cost-effectiveness analysis
- Household out-of-pocket expenditures on childhood pneumonia and diarrhea
- A cost-effectiveness analysis of maternal and neonatal health interventions in Ethiopia
- Health gains and financial protection provided by scaling up neuropsychiatric services in Ethiopia: A cost effectiveness analysis
- Measuring progress towards universal health coverage: National and subnational analysis in Ethiopia
- Supporting decision makers to save lives: Cost-effectiveness analyses for priority setting in Ethiopia
- Public financing of malaria interventions in Ethiopia: Health gains and financial risk protection
- Spatial distributions and characteristics of HIV clusters in Ethiopia
Publications
- Assebe, L. F., Negussie, E. K., Jbaily, A., Tolla, M. T. T., & Johansson, K. A. (2020). Financial burden of HIV and TB among patients in Ethiopia: A cross-sectional survey. BMJ Open, 10(6), e036892. https://doi.org/10.1136/bmjopen-2020-036892
- Assebe, L. F., Kwete, X. J., Wang, D., Liu, L., Norheim, O. F., Jbaily, A., Verguet, S., Johansson, K. A., & Tolla, M. T. (2020). Health gains and financial risk protection afforded by public financing of selected malaria interventions in Ethiopia: An extended cost-effectiveness analysis. Malaria Journal, 19(1), 41–41. PubMed. https://doi.org/10.1186/s12936-020-3103-5
- Blanchet, K., Alwan, A., Antoine, C., Cros, M. J., Feroz, F., Amsalu Guracha, T., Haaland, O., Hailu, A., Hangoma, P., Jamison, D., Memirie, S. T., Miljeteig, I., Jan Naeem, A., Nam, S. L., Norheim, O. F., Verguet, S., Watkins, D., & Johansson, K. A. (2020). Protecting essential health services in low-income and middle-income countries and humanitarian settings while responding to the COVID-19 pandemic. BMJ Global Health, 5(10). https://doi.org/10.1136/bmjgh-2020-003675
- Kiros, M., Dessie, E., Jbaily, A., Tolla, M. T., Johansson, K. A., Norheim, O. F., Memirie, S. T., & Verguet, S. (2020). The burden of household out-of-pocket health expenditures in Ethiopia: Estimates from a nationally representative survey (2015–16). Health Policy and Planning, czaa044. https://doi.org/10.1093/heapol/czaa044
- Memirie, S. T., Desalegn, H., Naizgi, M., Nigus, M., Taddesse, L., Tadesse, Y., Tessema, F., Zelalem, M., & Girma, T. (2020). Introduction of birth dose of hepatitis B virus vaccine to the immunization program in Ethiopia: An economic evaluation. Cost Effectiveness and Resource Allocation, 18(1), 23. https://doi.org/10.1186/s12962-020-00219-7
- Ying, R., Fekadu, L., Schackman, B. R., & Verguet, S. (2020). Spatial distribution and characteristics of HIV clusters in Ethiopia. Tropical Medicine & International Health, 25(3), 301–307. https://doi.org/10.1111/tmi.13356
- Eregata, G. T., Hailu, A., Memirie, S. T., & Norheim, O. F. (2019). Measuring progress towards universal health coverage: National and subnational analysis in Ethiopia. BMJ Global Health, 4(6), e001843. https://doi.org/10.1136/bmjgh-2019-001843
- Johansson, K. A., Tolla, M. T., Memirie, S. T., Miljeteig, I., Habtemariam, M. K., Woldemariam, A. T., Verguet, S., & Norheim, O. F. (2019). Country contextualisation of cost-effectiveness studies: Lessons from Ethiopia. BMJ Global Health, 4(6). https://doi.org/10.1136/bmjgh-2018-001320
- Memirie, S. T., Tolla, M. T., Desalegn, D., Hailemariam, M., Norheim, O. F., Verguet, S., & Johansson, K. A. (2019). A cost-effectiveness analysis of maternal and neonatal health interventions in Ethiopia. Health Policy and Planning, 34(4), 289–297. https://doi.org/10.1093/heapol/czz034
- Norheim, O. F. (2019). Priority Setting on the Path to UHC: Time for Stronger Institutions and Stronger Health Systems: Response to Recent Commentaries. International Journal of Health Policy and Management, 8(8), 511–513. https://doi.org/10.15171/ijhpm.2019.39
- Memirie, S. T., Habtemariam, M. K., Asefa, M., Deressa, B. T., Abayneh, G., Tsegaye, B., Abraha, M. W., Ababi, G., Jemal, A., Rebbeck, T. R., & Verguet, S. (2018). Estimates of Cancer Incidence in Ethiopia in 2015 Using Population-Based Registry Data. Journal of Global Oncology, 4, 1–11. https://doi.org/10.1200/JGO.17.00175
- Norheim, O. F. (2018). Disease Control Priorities Third Edition Is Published: A Theory of Change Is Needed for Translating Evidence to Health Policy. International Journal of Health Policy and Management, 7(9), 771–777. https://doi.org/10.15171/ijhpm.2018.60
- Memirie, S. T., Metaferia, Z. S., Norheim, O. F., Levin, C. E., Verguet, S., & Johansson, K. A. (2017). Household expenditures on pneumonia and diarrhoea treatment in Ethiopia: A facility-based study. BMJ Global Health, 2(1), e000166. https://doi.org/10.1136/bmjgh-2016-000166
- Tolla, M. T., Norheim, O. F., Verguet, S., Bekele, A., Amenu, K., Abdisa, S. G., & Johansson, K. A. (2017). Out-of-pocket expenditures for prevention and treatment of cardiovascular disease in general and specialised cardiac hospitals in Addis Ababa, Ethiopia: A cross-sectional cohort study. BMJ Global Health, 2(2). https://doi.org/10.1136/bmjgh-2016-000280
- Memirie, S. T., Verguet, S., Norheim, O. F., Levin, C., & Johansson, K. A. (2016). Inequalities in utilization of maternal and child health services in Ethiopia: The role of primary health care. BMC Health Services Research, 16. http://dx.doi.org.ezp-prod1.hul.harvard.edu/10.1186/s12913-016-1296-7
- Tolla, M. T., Norheim, O. F., Memirie, S. T., Abdisa, S. G., Ababulgu, A., Jerene, D., Bertram, M., Strand, K., Verguet, S., & Johansson, K. A. (2016). Prevention and treatment of cardiovascular disease in Ethiopia: A cost-effectiveness analysis. Cost Effectiveness and Resource Allocation, 14(1), 10. https://doi.org/10.1186/s12962-016-0059-y
- Verguet, S., Memirie, S. T., & Norheim, O. F. (2016). Assessing the burden of medical impoverishment by cause: A systematic breakdown by disease in Ethiopia. BMC Medicine, 14(1), 164. https://doi.org/10.1186/s12916-016-0697-0
- Driessen, J., Olson, Z. D., Jamison, D. T., & Verguet, S. (2015). Comparing the health and social protection effects of measles vaccination strategies in Ethiopia: An extended cost-effectiveness analysis. Social Science & Medicine, 139, 115–122. https://doi.org/10.1016/j.socscimed.2015.06.018
- Johansson, K. A., Memirie, S. T., Pecenka, C., Jamison, D. T., & Verguet, S. (2015). Health Gains and Financial Protection from Pneumococcal Vaccination and Pneumonia Treatment in Ethiopia: Results from an Extended Cost-Effectiveness Analysis. PLOS ONE, 10(12), e0142691. https://doi.org/10.1371/journal.pone.0142691
- Pecenka, C. J., Johansson, K. A., Memirie, S. T., Jamison, D. T., & Verguet, S. (2015). Health gains and financial risk protection: An extended cost-effectiveness analysis of treatment and prevention of diarrhoea in Ethiopia. BMJ Open, 5(4). https://doi.org/10.1136/bmjopen-2014-006402
- Verguet, S., Olson, Z. D., Babigumira, J. B., Desalegn, D., Johansson, K. A., Kruk, M. E., Levin, C. E., Nugent, R. A., Pecenka, C., Shrime, M. G., Memirie, S. T., Watkins, D. A., & Jamison, D. T. (2015). Health gains and financial risk protection afforded by public financing of selected interventions in Ethiopia: An extended cost-effectiveness analysis. The Lancet Global Health, 3(5), e288–e296. https://doi.org/10.1016/S2214-109X(14)70346-8
Video Links
Team Members
 Lelisa Fekadu Assebe |  Alemayehu Hailu |  Kjell Arne Johansson |
 Mizan Kiros |  Solomon Memirie |  Ole Frithjof Norheim |
 Mieraf Taddesse |  Getachew Teshome |  Stéphane Verguet |
 Seblewongel Yigletu |
Health System Modeling (HSM) is an area of research where dynamic mathematical models can be designed to describe, predict, and quantitatively capture the functioning of health systems and their components.
- Verguet, S., Feldhaus, I., Jiang Kwete, X., Aqil, A., Atun, R., Bishai, D., Cecchini, M., Guerra Junior, A.A., Habtemariam, M.K., Jbaily, A., Karanfil, O., Kruk, M.E., Haneuse, S., Norheim, O.F., Smith, P.C., Tolla, M.T., Zewdu, S., Bump, J. (2019). Health system modelling research: Towards a whole-health-system perspective for identifying good value for money investments in health system strengthening. BMJ Global Health, 4(2), E001311. https://gh.bmj.com/content/4/2/e001311
For more information please visit:
https://www.hsph.harvard.edu/health-system-modeling-initiative/