AIDS at 40: Gearing up for the endgame of a global scourge

June 3, 2021—On June 5, 1981, the CDC published the first official report of the disease that would come to be known as AIDS. In recent interviews, four researchers from Harvard T.H. Chan School of Public Health reflected on the successes and failures of the global response, and the work left to do to finally end the disease.
Lessons from a global disease
Phyllis Kanki, Mary Woodard Lasker Professor of Health Sciences
I’ve spent the majority of my career working on HIV—starting when I was a graduate student at the School soon after the virus was discovered. This disease is unique in the way that it impacted the whole globe—with a different biology and epidemiology in different parts of the world. We had certain populations at risk in the U.S., but really different ones in Africa and Asia. Many valuable public health lessons came out of the response: how the stigma of disease can impact individual health and societal responses; differences in health disparities locally and globally; the importance of engaged government leaders to impact policy; and the role of communities in useful interventions.
There were huge population segments and geographic regions of the world—largely poor—that had the greatest disease burden, and that also lacked access to treatments when they became available. I was glad to be part of the response that helped provide treatments and save millions of lives. I ran the School’s PEPFAR (President’s Emergency Plan For AIDS Relief) program in Botswana, Nigeria, and Tanzania. In each of those countries, we formed independent non-governmental organizations that took over the program when the School’s grants wound down, including the Botswana Harvard Partnership, AIDS Prevention Initiative in Nigeria (APIN), and MDH (Management and Development for Health), in Tanzania. I still work with APIN and I’m very proud of its accomplishments. It operates more than 570 clinics in Nigeria, and has provided treatment and prevention to more than 250,000 patients. Its scientists have also engaged in significant operational research that has been useful to the field.
We’re approaching the end of the HIV/AIDS epidemic, but we’re not there yet. We need to stay committed to achieving prevention and treatment goals to ensure that it is not with us forever. Ten years from now, I’m hoping that it will be a very unusual, rare disease, and that everyone who does have it will be able to access medications that work and allow them a high quality of life. It may be that a vaccine will come along that will decrease the numbers, but it’s likely that there will still be people on treatment. So, we have to continue to improve the treatments that we have to make them more tolerable and effective.
‘On the ropes’
Roger Shapiro, associate professor of immunology and infectious diseases
When I started working on HIV/AIDS in the mid-1990s, the problem seemed so enormous that it was difficult to contemplate how it might end. We could see all the challenges, but could only begin to imagine the scientific breakthroughs in treatment. Many experts predicted that large-scale distribution of antiretroviral therapy (ART) throughout the developing world wasn’t possible. I am grateful every day that this was not the case, and that ART was able to help us turn the tide of the epidemic. Now, more than 25 million people living with HIV receive ART, which is threefold higher than in 2009. Even high-prevalence countries such as Botswana, where I work, are meeting treatment goals. But we still need to do better. I thought that by now prevention and vaccine efforts would have shown more progress than they have, and I am frustrated that we still see new generations impacted by HIV.
Over the past 40 years, HIV/AIDS has changed public health. The community voices that brought attention to the epidemic in its early years accelerated the whole process for performing clinical trials in the middle of an epidemic, and for shrinking the timelines while maintaining scientific integrity. The legacy of this activism can be seen up to the present in our more accelerated response to performing research during the COVID-19 pandemic.
In the next ten years, new long-acting antiretrovirals could improve both treatment and prevention—and make a big difference if we apply them strategically. PrEP (pre-exposure prophylaxis medication) with long-acting agents should be targeted at 16-24 year olds to break the cycle of transmission for the next generation. We can also dramatically reduce pediatric HIV if we can accelerate research into using long-acting agents for pregnant and breastfeeding women, and possibly as prophylactic agents in infants. I don’t think HIV/AIDS will be gone in 2031, but we’ll have it on the ropes.
The gap between science and policy
Kunjal Patel, SD ’06, senior research scientist in the Department of Epidemiology
I immigrated to the U.S. from Zambia in 1985, when I was in third grade, and high school health class was the first time I heard about HIV/AIDS. I started learning more about it when I was in my MPH program at Yale, and I became fascinated. For an infectious disease, it required understanding of intersecting domains of health science—infectious disease transmission dynamics, prevention, treatment, adherence, and social and behavioral science. As an epidemiologist, I thought it was a goldmine. And then, I attended a lecture by the epidemiologist Sir Richard Doll, where he lamented that science often didn’t lead to effective policy. One thing he mentioned was that many studies had shown that needle exchange programs were really effective at reducing HIV transmission among injection drug users. But still, federal programs would not fund them. That made me so angry. I saw how much work there still was to do, from bench science to policy, and that really solidified my interest in tackling this epidemic.
At Harvard Chan School, I was lucky to have the late George Seage as a mentor in my doctoral program. Through him, I started working in pediatric HIV, and was able to contribute to the development of the Pediatric HIV/AIDS Cohort Study (PHACS). Now, I lead and serve as the senior epidemiologist on study teams across this and other pediatric HIV cohort studies. The work is informing perinatal and pediatric guidelines for people with HIV and will continue to inform guidelines as our population ages. We work very closely with our community of participants and caregivers to make sure that we really understand the lived experience of the participants we’re studying. There are so many other things going on in our participants’ lives besides their treatment outcomes. Their HIV doesn’t define them.
I think it’s amazing that over the last 40 years, HIV has gone from a death sentence to a chronic illness. In terms of prevention and treatment, we have great tools in our toolbox. But getting them implemented is still a problem. Part of addressing this is doing better at meeting people where they are, particularly those who may feel distrustful of the health care system. In the fight to eliminate HIV, this last stage will be the hardest. We’re going to need to get more creative, more innovative.
Getting past fear
Antón Castellanos Usigli, DrPH ’22, Cheng Fellow
I don’t remember exactly when I first heard about HIV. But I do remember growing up as a gay teenager and fearing it, even though I practiced safe behaviors. For a lot of men who have sex with men, this fear shapes your first sexual experiences. Unfortunately, a lot of sex education uses fear and shame as behavioral motivators—creating more stigma for a population that is already stigmatized.
This made me angry as a teenager, so I became an advocate for comprehensive sexuality education in my high school in Mexico—the first step in what would become my career. My public health work is now focused in supporting my community to gain access to high quality sexual health services. When I was working at a hospital in Brooklyn a few years ago, I was asked to help bring more young gay and bisexual men into the clinic to get HIV/STI testing and Pre-Exposure Prophylaxis (PrEP) [HIV prevention medication]. Traditional outreach methods weren’t working, so I decided to try reaching out in the space where men talk to each other about sex—dating apps. And it worked. We brought in around a hundred new clients every year with this approach. I’m currently working to expand this initiative in other contexts across the US.
I’m so grateful to the generation of HIV/AIDS activists in the ’80s and ’90s who demanded that the government address the epidemic and the homophobia that was driving the silence and the stigma around it, and who fought for access to lifesaving medications. They really are a unique example of a global health movement. There was so much passion, so much strength that the community drew from itself. In many public health programs, we tend to think about how the negative things a population faces influence their health. But we rarely speak about the strengths of a community. I think that the early days of the HIV epidemic really reflect the importance of the social support that we can give each other.
Of course, things have changed quite a lot since the early days of the epidemic. But there’s still so much work to do. We need to innovate more and increase access to sexual health services and education. We need to listen to people’s stories, have honest, positive conversations about combining sexual pleasure with safety—and move away from an approach to sexual education that relies on fear.
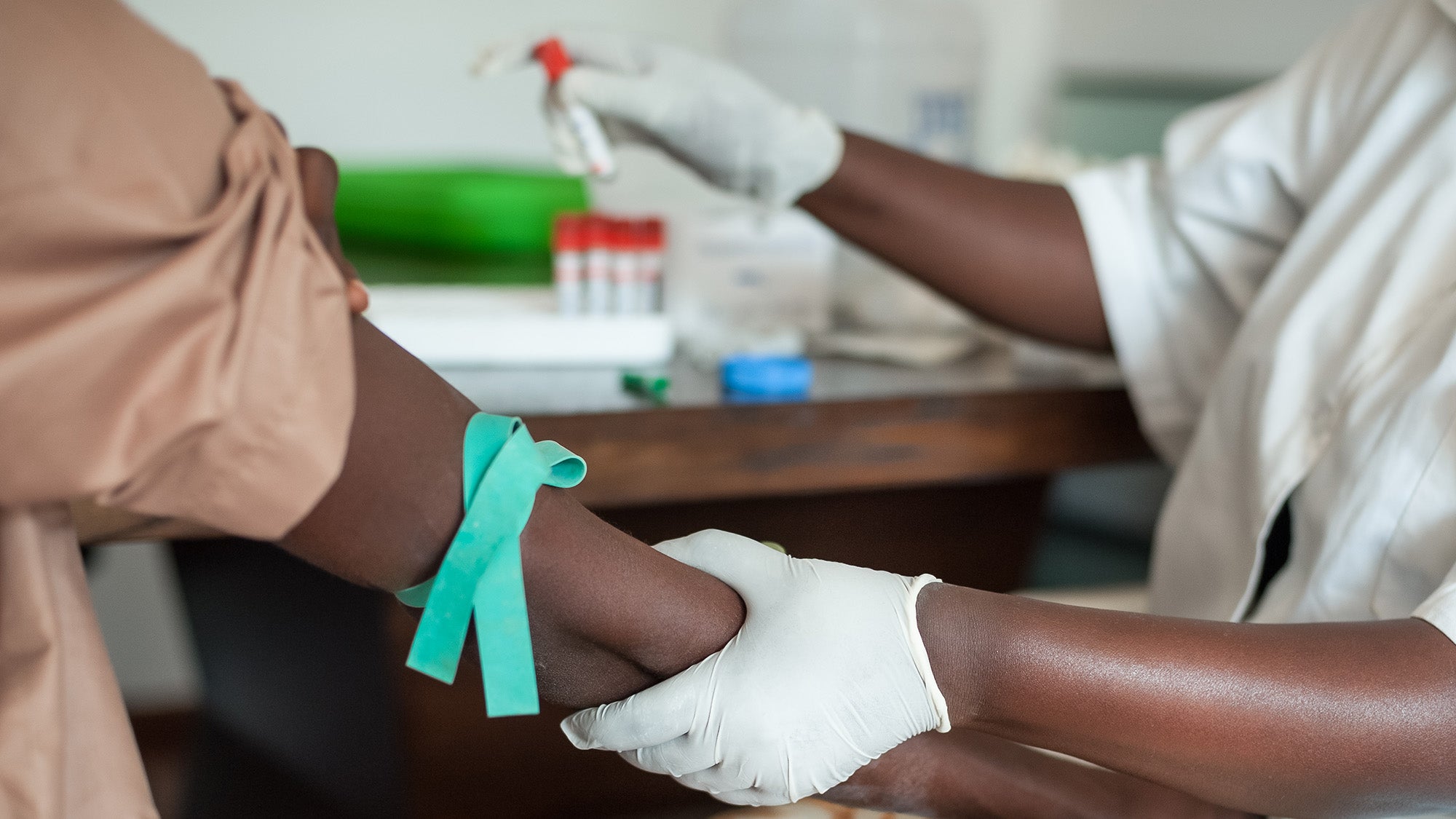
Photo: Shutterstock