[ Fall 2011 ]
Christian Benjamin, MD, MPH ’96 and Michael McCarten, DO, MPH ’99 are delivering evidence-based military medicine in Afghanistan
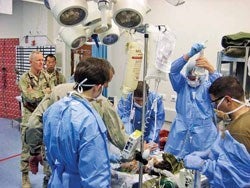
Medics roll a badly wounded U.S. soldier into the military hospital in Kandahar, Afghanistan. He has lost both legs to a roadside bomb, and his abdomen, head, and neck are torn up. The international surgical team snaps into action to clean his exposed flesh; specialists check for head trauma. A few days later, the bandaged young soldier is flown to another military hospital for more surgery, then begins his journey home to recover.
Heart-wrenching scenes like this unfold regularly at the NATO Role III Multinational Medical Unit in Kandahar. “The trauma we see here is devastating,” says U.S. Navy Capt. Michael McCarten, DO, MPH ’99, who spent a year commanding the hospital in 2010–11. “Sometimes the anatomy is unrecognizable.”
About 300 miles away, U.S. Air Force Col. Christian (“Chris”) Benjamin, MD, MPH ’96, witnessed similarly grave injuries during his year leading the Craig Joint Theater Hospital at Bagram Air Field. Equipped with operating rooms, ICU beds, laboratories, and other state-of-the-art services, these trauma centers treat both coalition forces and Afghan soldiers and civilians, including children maimed by explosives.
The hospitals boast 98 percent survival rates, and McCarten and Benjamin credit their resourceful teams and several public health strategies—such as reducing the lag time between injury and surgery—with helping save lives in the decade-long war in Afghanistan.
Lasting Lessons
Benjamin and McCarten belong to a cadre of alumni who attended Harvard School of Public Health as part of their military medicine training, most of them in its one-year MPH program. Their crew cuts may have stood out on the liberal-leaning campus, but the pair say their Harvard education has helped guide their leadership roles in combat hospitals, on military bases, and aboard aircraft carriers. Military medicine, they explain, typically involves caring for healthy young people serving in hazardous environments, such as noisy flight decks or hot engine rooms; it also involves tending to families, retirees, and veterans.
Data From the Front Lines
The value of research was one of the biggest takeaways from HSPH. “They teach you how to ask questions, analyze the data, and come up with answers that fit the situation you’re in,” recalls Benjamin, who now commands the U.S. Air Force School of Aerospace Medicine.
This attitude meshes with the self-analytical approach of the U.S. military medical system. “We are our own worst critics,” says McCarten, who was interviewed via Skype. “We understand the sacrifices these men and women have made.” In Afghanistan, he and Benjamin drew from statistics the Pentagon has collected from recent conflicts to identify best practices and improve outcomes. Take tourniquets, for example. Used for centuries to stop bleeding on the battlefield, these simple devices became controversial because they can aggravate the injury if applied incorrectly. But the timely use of tourniquets has proved essential during the wars in Iraq and Afghanistan, where homemade bombs or “improvised explosive devices” (IEDs) have led to a horrifying number of amputations.
These and other evidence-based strategies from the front lines, including cranking up the ER temperature to prevent hypothermia, have caught the attention of civilian counterparts. Indeed, Benjamin hosted visits from four renowned civilian trauma surgeons during his year in Bagram.
Infection control is a crucial public health weapon in military medicine, and hand hygiene is paramount on the Bagram and Kandahar bases. In hospitals, the routine use of antibiotics can quickly foster drug-resistant bacterial infections, a problem exacerbated in Afghanistan because many local patients are malnourished and show up with dirty, festering wounds—all factors that hinder healing and lead to longer hospital stays. Bugs such as Pseudomonas and Klebsiella are among the most stubborn and virulent antibiotic-resistant pathogens in these military hospitals—just as they are in the U.S.
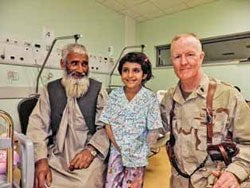
Life Expectancy: 45 Years
Amid rampant poverty, unsafe drinking water, limited access to care, and other challenges, Afghanistan has a dire health profile. The nation’s average life expectancy is 45 years and the maternal mortality rate is one of the highest in the world.
Serving in Afghanistan reminded McCarten of courses given by Michael Reich, Taro Takemi Professor of International Health Policy, and Ichiro Kawachi, chair of the Department of Social and Behavioral Sciences. These courses underscored the message that socioeconomic conditions shape health outcomes. “Looking at health systems around the world that I’ve observed in my Navy career, it’s clear that the rich get richer and the poor get poorer,” McCarten says. “My time at Harvard, and those two courses in particular, changed my politics. They were absolutely life-changing for me.”
Supporting the Wounded
As they evacuated patched-up soldiers to bigger facilities in Germany and the United States, McCarten and Benjamin knew that recovery would test their patients’ fortitude. But they say military and veterans’ hospitals have made impressive gains in providing for wounded warriors, especially those with the signature injuries from Afghanistan and Iraq: amputations, traumatic brain injury, and psychological scars.
The two doctors envision a health care system that addresses the service members’ physical, emotional, and spiritual needs and a society that supports them as they strive to rebuild their lives. As McCarten puts it, “They deserve nothing less.”
Debra Bradley Ruder is a Boston-based freelance writer specializing in health care, education, and end-of-life issues.
Photos: U.S. Air Force photo by Master Sgt. Jeromy K. Cross; courtesy of U.S. Navy Capt. Michael McCarten, DO, MPH ’99
