Finding Purpose in the Pandemic

Ten newly minted public health professionals, three doctoral students, and a postdoctoral scholar describe their time on the front lines of the COVID-19 crisis
EXTRA POINTS FOR SPANISH
Sofia De Arrigunaga, MPH ’20
I have lost count of the number of people who have said, “Oh, so this is what you went to school for!” when talking about the COVID-19 pandemic. As a physician, I wanted to get a macro, populationwide view on health, which led me to pursue a master’s in public health. As fate would have it, I picked a year in which the field would be spotlighted like never before in my lifetime. With that sudden attention came an unusual end to the semester and a sooner-than-expected call to action.
As soon as the pandemic became a problem in Massachusetts, I got involved in two capacities. I am part of the core founding team of Students Against COVID-19, an initiative that aims to empower young people through evidence-based information and opportunities to support vulnerable populations. As a point person for the Tackling Misinformation and Social Media teams, I create content for our Instagram presence (@students-againstcovid19). Through this endeavor, I have been reminded of the challenges of effective communication in public health and how difficult it can be to convey important messages and tackle myths.
Engaging in constructive and clear communication was even more relevant in my other role as a volunteer contact tracer for the MA COVID-19 Academic Public Health Volunteer Corps with the Massachusetts Department of Health. I never imagined I would be involved in such an essential component of controlling a public health crisis before having graduated. Through this work, I witnessed the importance of this basic, centuries-old epidemiological intervention.
The concept of contact tracing is simple, but its execution can be tedious and time-consuming. I was in charge of calling people who were diagnosed with COVID-19 and interviewing them. After asking general questions regarding their symptoms and clinical course, I asked whom they had recently been in physical contact with. I then proceeded to call those people to let them know of their potential exposure and advise them on next steps per state guidelines.
This made for some very difficult conversations. I made calls and found out the person I was looking for had passed away. I had long talks with people who were very scared. I have explained countless times how and why public health measures are effective.
I also had some incredibly gratifying calls. Some people were very grateful for having a Spanish-speaking volunteer reach out, because they felt more comfortable asking questions in their own language. Other times, I could tell people were lonely and just wanted someone to talk to. Alone in my Boston apartment after our classes moved online, I also welcomed their company and small talk. The work was very fulfilling and gave me a sense of purpose during the second half of the semester.
There was one particularly moving exchange in which an elderly woman thanked me for my time after we went over COVID information thoroughly. Her friend had passed away from the disease, and my elderly contact wanted to understand it better—she felt overwhelmed by the excessive, and sometimes conflicting, information. She asked me about myself, where I was from, and why I was volunteering to make these calls. She told me she was very proud of me for being able to distill it for her, and that I got extra points for having done it in Spanish. Before hanging up, she made me promise that I would be “careful out there,” which I continue to do after so many months
FACING THE LIMITS OF EPIDEMIOLOGY
Ruoran Li, ScD ’20
January 22, 2020
It was a Wednesday afternoon, and I had an hour to kill at the School between a group meeting and a meeting with my academic adviser. There had been a lot of talk on Chinese social media of a mysterious viral outbreak in Wuhan (“pneumonia of unknown origin,” “NOT SARS”) and some local government cover-ups, so I decided to look at the raw data in that hour, because interpreting data is the one thing I’ve been trained to do over many years of academic epidemiology training.
From the local health commissioner’s website, I extracted the reported numbers of “pneumonia cases of unknown origin” and plotted the epidemic curve over time. From those data, I discovered the rumored local government cover-up over a period of 10 days where no new cases were reported. I also noted a lot of changes in the terminology and case definition of this new disease. Although expected, given the rapid evolution of the scientific understanding of the disease, these changes would inevitably cloud our understanding of the spread of the virus.
Still, despite the noise, the story was quite clear. There was a new infectious agent spread by the respiratory route (by then, Chinese scientists had confirmed evidence of human-to-human transmission), and it had infected hundreds of people in one of the biggest transportation hubs in China.I took this plot and showed it to my adviser during our meeting. I remember pointing to the artificial suppression of case counts in early January and saying, “Imagine how many cases there are now in Wuhan that are not being reported!” My adviser offered an academic explanation: If local health officials were catching up on reporting previously unreported cases, then the true epidemic growth (the doubling time) was much slower than what was implied by the rising case counts after January 16—which meant, luckily, the outbreak was not as scary as people thought it was. I had no comeback to that suggestion, and we moved to other topics. But I knew, deep down, that I had failed to convey in that exchange the urgency I felt.
In hindsight, the conversation was the first of many of my encounters with what I feel was the systemwide tendency of many public health practitioners in the U.S. to downplay the severity and implications of COVID-19 at the beginning of the pandemic. If I may venture to guess the thought process of a U.S.-based epidemiologist faced with early COVID data, one natural line of thought would be: Because there are so many issues with raw data at this early stage of the outbreak, and because my training has made me good at finding biases within these data, how much weight can I give to what the data are showing? How much information from case counts data in China do I need in order to change my prior belief that a global calamity unseen in decades is not brewing at this moment?
Unfortunately, presenting my argument with data—and data alone—is what I had learned and what I relied on at the time. What I failed to realize back in January was that data were not the only information we had about the disease. In fact, data were not the main source of information from which I personally learned about the outbreak and realized its potential severity. So why would data be the only tool that I used when trying to translate the experience in Wuhan into the English-speaking world?
And as with many Mandarin-speaking colleagues, the realization that I had failed to convey something marked the beginning of my early crusade to translate across language barriers, cultural barriers, political barriers, and, most important, social media barriers.
Social media was the one place where I found refuge from my own data-doubting instinct, a place that has been the most dominant feature of my epidemiological training. Especially in late January and February, Mandarin social media sites were where I saw the suffering of real people in China from an uncontrolled epidemic (the virus was spreading in a largely uncontrolled way before late January). Human suffering that was not just from becoming infected with the virus, but also from the overwhelmed hospital capacity, from uncoordinated local NGO and government responses, and from family separations. Human suffering that the Western media were either unaware of or ignoring then.
The next several months were a blur to me. With the help of so many mentors, colleagues, and friends, we published some underutilized data in Chinese social media that highlighted the hospital capacity issues (a preprint and then a paper). Some Western media finally took notice, just when people started to realize the pandemic would come to them. And I graduated with a doctor of science in epidemiology.
••••
Five years earlier, I had sent my doctoral application essay to dozens of infectious-disease epidemiology programs around the world and received an acceptance letter from the Harvard Chan School. My essay included the following sentence: “Having experienced the 2003 SARS outbreak firsthand whilst living in Guangdong province, where the virus originated, I have a profound interest in surveillance, outbreak detection, crisis response and public health communication.”
Looking back, I realize that I had unrealistic ideas that studying epidemiology would help one combat an epidemic, as if epidemiologists could come to the rescue in an emergency using the toolkits that were taught in graduate schools. Now I realize that notion is quite naive.
If I were to write a personal statement now, would I mention SARS or today’s coronavirus, SARS-CoV-2? Maybe I would observe that we are sometimes very good at using our epidemiological training to justify our preexisting biases and turn a blind eye to other ways of gathering information. Looking forward, I hope to relearn some basic epidemiology—and this time, be more mindful not only of its advantages but also of its limitations.
“I often found myself delivering bad news over the phone to family members who never had the opportunity to say goodbye to their loved ones. The anguish in their voices and their cries will echo in my mind for the remainder of my days.”—Matt Moll, MPH ’20
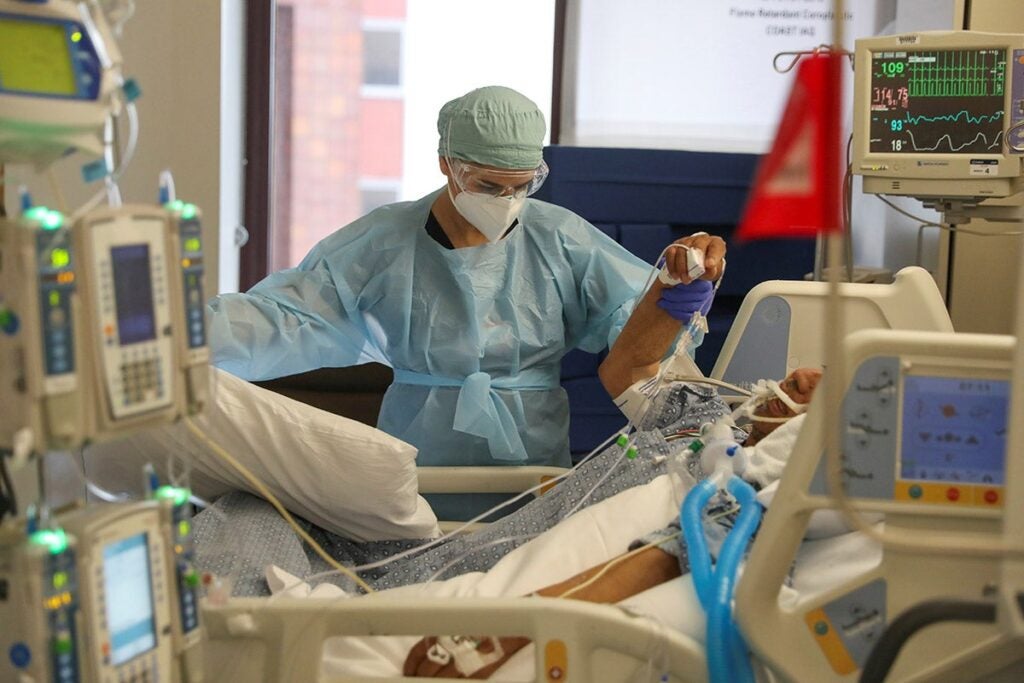
WITNESS IN THE ICU
Matt Moll, MPH ’20
My journey into public health came through medicine. As a medical resident at Boston Medical Center, which serves low-income and underresourced communities in Boston, I saw firsthand how social determinants are intertwined with all aspects of health and disease. During my pulmonary and critical care fellowship at Brigham and Women’s Hospital (BWH), I decided to study chronic obstructive pulmonary disease because it is a common condition that disproportionately afflicts minority and disadvantaged populations. In that context, I entered the quantitative methods MPH program at the Harvard Chan School and graduated in May.
In early March, I saw my first case of COVID-19 while working at a local community hospital near Boston. The patient was a 63-year-old man with diabetes mellitus and hypertension. He was struggling to breathe, and his oxygen requirements were escalating. That night, I saw more fear and panic than I had ever seen in a hospital. Seasoned ICU (intensive care unit) nurses were scared, and staff members were refusing to perform studies. Subsequently, I saw the ICUs fill up with COVID-19 patients in a matter of weeks. I had never seen anything spread so fast, and in the blink of an eye, the entire world had changed.
I felt it necessary to temporarily forgo my research and instead contribute to the pandemic efforts. Clinically, the early days were horrifying; we did not know what to expect, whether we would run out of personal protective equipment (PPE), or how well the PPE we did have would work. Many health care staff, including myself, moved away from home to protect their loved ones. Looking back, the worst part of these first weeks was that we did not let families visit. I often found myself delivering bad news over the phone to family members who never had the opportunity to say goodbye to their loved ones. The anguish in their voices and their cries will echo in my mind for the remainder of my days.
I also joined the BWH COVID-19 Critical Care Guidelines Committee, serving as the hematology section editor for covidprotocols.org—one of the earliest open-source guides for clinical care of COVID-19 ICU patients. The guide represents the collaborative, selfless work of more than 100 BWH health care workers. It was here that my public health training became paramount, as I needed to quickly digest and critically evaluate a deluge of scientific literature and work with expert hematologists at BWH to develop clinically relevant guidelines for COVID-19 ICU patients.
As we learned from our patients, individuals with COVID-19 may be particularly prone to developing blood clots. Using skills I gained at the Harvard Chan School, I worked with physician Jean Connors in the BWH division of hematology to evaluate the effectiveness of our anticoagulation strategy. Based on time-to-event analyses, we found that COVID-19 ICU patients appear to exhibit a state of elevated inflammation, which predisposes them to blood clots. We then increased the dose of prophylactic anticoagulation (blood-thinning medications) and are evaluating whether this change has been effective.
I am extremely grateful for my education at the Harvard Chan School. One thing I wish I had spent more time learning about, however, is advocacy. COVID-19 has put the spotlight on existing health disparities in our country, and in the setting of George Floyd’s murder, it is clear that systemic racism is a public health crisis. The Harvard Chan School houses a wealth of human and intellectual resources. Treating patients, writing guidelines, and performing scientific research during this pandemic have highlighted to me the importance of the work done by faculty, postdocs, students, and alumni—we are needed more than ever!

MANAGING AN OLYMPIAN EFFORT
Eric Coles, DrPH ’20
Frustration inspired me to get involved in the COVID-19 response. I submitted my dissertation for a doctor of public health (DrPH) degree at the Harvard Chan School the same week in March that social distancing began and workplaces closed in Massachusetts. I then began studying the news. Clinicians, mainly doctors but also a few nurses, were everywhere, writing opinion pieces, being quoted as experts in stories, and being hailed for their part in the response to COVID-19.
But I felt COVID-19 was a public health crisis, not just a clinical one, and needed a public health response. Watching clinicians lead the response was like an engineer watching a physicist build a bridge. I longed to see public health experts lead.
A serendipitous email was my door into the volunteer response. Well before COVID, I was planning a conference of DrPH alumni with some other members of the nascent DrPH Coalition. Unfortunately for public health, the DrPH degree is underappreciated and under-utilized. Over a year ago, my DrPH classmates and I started connecting with DrPH students in other programs around the country. We’ve since contacted about 30 programs and plan to incorporate a nonprofit to elevate the identity of the DrPH and advocate for public health.
We were planning on holding a conference in April about how DrPH alumni were working in local public health. While emailing speakers about the change to a virtual conference, we asked about ways to volunteer. One speaker connected my classmate Cris Alonso and me with the COVID-19 Academic Health Department Consortium, which had been recently tasked by the Massachusetts governor’s COVID-19 Command Center to organize public health volunteers to support local boards of health. They were looking for volunteers, and we were looking to respond.
Things moved rapidly from there. My first email with the consortium was on a Tuesday in late March. By that Friday, we had a team structure, and by Sunday we spoke with our first local board of health about utilizing our volunteers. Our volunteer model was vital. We identified a team lead who would be the single point of contact with the board of health and a group of volunteers, essentially acting as a project manager. From my connection with the DrPH Coalition, I found about 20 DrPH students and alumni from the Harvard Chan School and Boston University who could serve as the initial team leads. The DrPH program emphasizes both leadership and research, which proved to be a perfect combination.
Time was a blur from March 30 through April 11. I met with around 40 local boards of health and their team leads to conduct a rapid needs assessment. There were some dire situations. Some boards of health had a handful of staff and dozens of new cases each day that needed to be contact-traced. Others were making calls 10 hours a day and yet still couldn’t keep up with the cases. I felt the relief in their voices when they realized there was support. Based on their stated needs, I would grab names from our database of nearly 2,000 volunteers and give a list to the team lead, who managed the project from there.
The volunteers were wonderful. When I checked in a few weeks later, the team leads would talk about “their” local board of health and “their” volunteers. Everyone made the project their own and developed connections with the public health director or nurse. The volunteers produced great work—making thousands of calls, creating dozens of infographics, translating material into over 10 languages, and managing social media accounts.
This experience opened my eyes to local public health. I am embarrassed to admit that I did not know the “10 essential public health services” beforehand. I had never considered working in local public health. I now see why. Much of local public health is anachronistic. The 10 essential services were written 25 years ago. The key services are engineering-focused, such as inspecting and registering construction, or clinical-focused, such as infectious-disease surveillance.
Social determinants of health, which was the focus of my dissertation, are not mentioned in the 10 essential services. There is little on health inequities and racism. I was also disappointed to see that local public health does not get involved in other policy conversations, such as around housing, food, transportation, employment, and economic policy. Yet these policies create the social determinants of health, which are widely considered to shape more than half of someone’s health status. Local public health is not addressing the major causes of health. It is a problem I would like to change.
My efforts in Massachusetts opened other doors to get involved in the COVID response. I am now the acting public health officer for a small Native American tribe in California, called Tule River. They have similar needs to those I encountered when I started volunteering in Massachusetts: contact-tracing capacity, data analysis, and policy research.
In my volunteer position in Massachusetts, I felt like the Olympic Committee organizing the games: My job was to get public health professionals onto the field to show their talents. We need more public health expertise to resolve this pandemic, rather than relying solely on clinicians. I hope the volunteers I helped put into the field are the start of such an effort.
HOPE DURING A HOPELESS TIME
Amy Bantham, DrPH ’20
I defended my doctoral research on March 9, the last in-person defense before the process was moved online on March 10. I had planned to spend the week celebrating and relaxing before I flew to San Diego to present my research at a conference. Instead, I watched anxiously as public schools were closed, my conference was canceled, and the world turned upside down. I sat on the couch for a few days feeling sad about my derailed plans and then decided that was enough. After all, my doctor of public health program provided me with public health and leadership skills and expertise. It was time to lead.
A fellow DrPH classmate, Eric Coles, approached me about being part of a volunteer initiative. He and another classmate, Cris Alonso, were calling on DrPH students and alumni to lead teams helping local public health departments with their COVID-19 responses. Through the DrPH Coalition, and in collaboration with the Massachusetts Department of Public Health and the Massachusetts Health Officers Association, the needs of local public health departments were identified, and public health student and alumni volunteers were recruited to help meet those needs.
I wanted to get started immediately, and Eric recommended that serving as a team lead would have the most immediate impact. That is how I became a team lead for Avon, a small town in eastern Massachusetts, and for Somerville, the city I have called home for the past 13 years.
Our Avon team of five volunteers was one of the first teams on the ground, and we spent the month of April checking in on the health and well-being of residents with confirmed cases, as well as their contacts. Part of our role was monitoring people’s symptoms, answering their questions about symptoms and length of quarantine/isolation, and providing them accurate, up-to-date information as knowledge of the virus evolved.
Our Somerville team of 25 volunteers was a key partner in implementing the city’s plan to control the spread of COVID-19 through testing, tracing, and safe isolation. On April 27, the mayor and the health department announced a citywide testing initiative, available for free for all Somerville residents. Between April 30, the first day we made calls, and the end of June, we reached out to almost 7,000 Somerville residents with their test results. We supported the hard work of a team of public health nurses and reached residents with important information about their test results and the length of time they needed to quarantine or isolate. We connected residents to city services, such as food, housing, and utility assistance, and helped them obtain letters confirming test results so they could return to work. Our team also fielded questions about the accuracy of the diagnostic testing and the availability of antibody testing. In one memorable instance, our volunteers ensured that a resident experiencing severe symptoms was connected to emergency medical services.
I was inspired by the level of engagement from public health students and alumni across Massachusetts. Within 24 hours, 700 volunteers responded to the initial call to action, and almost 2,000 in total signed up to be a part of the public health volunteer corps. I was continually amazed by the commitment of the volunteers on my teams, who juggled school, work, and family to always make the time to contact the people on their lists. I was impressed by the local public health departments, which, despite limited resources, work around the clock to protect the health of their residents. This volunteer work gave me hope during a time that has often felt so hopeless—hope that, through public health expertise, accurate information, and teamwork, we will find our way out of this crisis.
“This volunteer work gave me hope during a time that has often felt so hopeless—hope that, through public health expertise, accurate information, and teamwork, we will find our way out of this crisis.” —Amy Bantham, DrPH ’20
A FOCUS ON PANDEMIC LONELINESS
Kasley Killam, MPH ’20
A long personal and professional journey of exploring human connection led me to a field that has become very relevant during the coronavirus pandemic. I began my career 10 years ago by studying mental health and positive psychology—the science of attributes and habits that help individuals and communities thrive. The data, I found, consistently showed that one of the most robust sources of health and well-being is strong relationships.
Excited to have research supporting what I knew anecdotally to be true, I started putting it into action, bridging academia and the general public. For instance, I created a mobile app to promote empathy and kindness through simple, evidence-based steps that users could take, and I made physician-patient relationships a pillar of a health care entrepreneurship program I worked on.
Five years later, researchers and mainstream media started talking about unusually high rates of loneliness across the country. Because of my background, I knew that just as good relationships can make people healthy and happy, the absence of these connections can lead to disease, depression, and death. By day, I was leading community engagement and strategic partnerships at Verily, a spinoff of Google focused on health tech and innovation. But by night and on weekends, I couldn’t stop thinking about social health: the dimension of well-being that comes from connection and belonging.
Motivated by this urgency, I started writing articles and giving talks about social health. I organized local events to crowdsource solutions for isolation and facilitate friendships among neighbors of different generations. I joined the board of a nonprofit whose programs fostered community and reduced loneliness among older adults. This work culminated in the decision to focus on this topic full time.
In August 2019, I moved from San Francisco to Boston to earn a master’s degree, specializing in social and behavioral sciences at the Harvard T.H. Chan School of Public Health. Once there, I dove even deeper and thought strategically about multilevel, multisector approaches to reweaving our fragmented cultural fabric.
Then the pandemic hit. With required quarantines, suddenly this issue was at the top of everyone’s mind. Physical isolation was necessary to avoid COVID-19, but I knew that social connection was also necessary to address the simultaneous public health crisis of loneliness. The irony was clear: Emotional support from others can protect you from getting sick, studies have shown, but physical contact with others during this time can literally make you sick.
With my expertise relevant in a new way, I spent the first few months of the pandemic writing articles for Scientific American and Psychology Today, being interviewed on podcasts and news outlets, and collaborating on a statewide task force and national coalition to prevent and reduce loneliness. Meanwhile, I finished my degree, graduating virtually with my peers spread out around the world.
It was a surreal time, holding the melancholy of grief in one hand and the fulfillment of service in the other.
That brings me to today. As a realist, I am worried that the coronavirus pandemic could exacerbate the loneliness epidemic. I will be paying close attention to the data that comes out on this in the months and years to come.
But as an optimist, I have to believe that some benefits will emerge, too. People are being more intentional about social connection as a direct result of the coronavirus. We are prioritizing relationships, meeting neighbors for the first time, and reconnecting with old friends. We are also innovating and reimagining the roles that technology, urban design, workplaces, and other sectors play in our social health. These are both promising trends.
No matter how long the pandemic persists, my hope is that we will collectively hold on to the new appreciation we have developed for our relationships. Moving forward, we must leverage the momentum of these times to proactively shape our culture around social well-being
HOW QUICKLY THE “NORMAL” CAN CHANGE
Eva Rumpler, SM ’20
When reflecting back on the first months of the COVID-19 pandemic, the thing that strikes me most is the speed at which things changed.
In the early days of January, I texted one of my best infectious-disease–loving friends, “Did you read about the new virus in China?” and quickly followed up with, “Oh, forget about it, there’s no human-to-human trans-mission.” A month later, the virus was all we could talk about. After another month, the Harvard Chan School had closed down, and I was sitting on a plane headed back home to France.
I first realized that the novel coronavirus epidemic was going to become a serious problem outside of China when my adviser suggested I postpone my project on antimicrobial resistance and start working on the new virus. I had followed the unfolding of the epidemic in Wuhan with a lot of interest but had little to no involvement.
For me, advocating social distancing and infectious-disease–control measures to my family and friends was one early response to this pandemic. As my understanding of the severity of this pandemic quickly grew, so did a huge gap between my level of worry and that of my family, especially at the beginning of the crisis. I spent hours negotiating with my 87-year-old grandma living near the epicenter of the epidemic in France, trying to persuade her to limit her exposures. I had expected to be a much more experienced public health practitioner by the time I started providing unsolicited advice, warnings, and interdictions to my family. Still, I hoped my informed opinions would be taken into consideration more seriously. I was wrong on all counts.

Reading the Imperial College report that showed that reaching herd immunity by letting the virus circulate was ethically inconceivable, because it would cost an impossibly high number of lives, was one of the most memorable moments of the beginning of the pandemic. Never had I been this emotional while reading a scientific report. Realizing that lockdown measures would need to be implemented almost continuously until a vaccine would become available was exceptionally sobering, sad and scary.
TRANSFORMING A HOSPITAL
Nancy Haff, MPH ’20
“I am down two chief residents. Looking to see if you have the bandwidth to help out for the next few days.” So read the text I received from my medical residency program director the morning of March 17, the beginning of the COVID-19 surge in Boston. A few hours later, I was in the department of medicine office at Massachusetts General Hospital (MGH), grateful for the opportunity to see how I could help.
Several of the recent chief residents who had returned to pitch in quickly found needs and dove in. My former co-chief, Nino Mihatov, and I arrived just as the hospital was beginning to transition an oncology unit to a COVID floor. Two days later, a rising number of cases dictated that a neurology and neurosurgery floor be converted as well. While helping these floors transition to caring for patients experiencing COVID-19, we noted the hundreds of ways in which a floor had to change its operations to take care of patients with this new disease. We didn’t have many answers, but we collected questions, issues, and common threads to discuss with content experts and leadership.
We quickly realized that accommodating the surge in COVID admissions required extraordinary interdisciplinary collaboration and rapid operational changes. With representation from nursing and operations management, we formed a team to help convert entire floors to COVID units going forward. Our team applied the knowledge gained from opening the first two floors to generate an operational checklist and floor-opening process that we then used to convert a total of 12 COVID floors between March 18 and April 24, the MGH inpatient peak.
That first month felt fast paced, overwhelming, exhausting, exhilarating, and inspiring all at the same time, and our involvement was only the smallest sliver of MGH’s massive response to COVID. Although I learned and relearned so many lessons during that time, I’ll share two that most relate to my training at the Harvard Chan School: the Plan Do Study Act (PDSA) mindset and the power of observation.
Just before the pandemic struck, in my final semester at the Harvard Chan School, I was taking a course taught by Don Goldman (professor of immunology and infectious diseases and epidemiology) on quality improvement. In the first few weeks, we covered Plan Do Study Act cycles. Although I had to change my class schedule shortly after the outbreak, I soon realized that my daily work in the COVID response was an immediate application of these principles. Because knowledge and best practices evolved quickly, as we all learned about this new disease, every action we took had to be rapidly evaluated and revised. Inpatient COVID volume rose daily, and we often needed to act immediately, choosing the action that made the most sense given what we knew at the time. When that didn’t work or information changed, we’d try again, and again. The analogy we’d often cite was that of building a plane while flying it. There was so much to learn and adapt, and the only way to do that was to bring a PDSA mindset to everything we did.
My respect for the power of observation gradually emerged from daily virtual COVID calls that we set up with the floors to rapidly disseminate information and answer questions. Nearly every day, we had a guest on the call to talk about a new initiative. For example, providers quickly noted that a large percentage of patients experiencing COVID-19 were Spanish-speaking. Within two weeks, the diversity and equity teams established a group of Spanish-speaking providers who were on call day and night to help teams communicate with patients and families.
Meanwhile, several medical residents noted that many patients did not have the resources to safely isolate at home. So they created discharge kits that were sent home with patients in need that contained soap, hand sanitizer, masks, and information about how to protect their families. Several teams recognized that many patients did not have their own devices, such as smartphones or tablets, to connect with family, and no visitors were permitted. From this observation, Patient Connect devices, or iPads with Zoom, were deployed to the units so patients could virtually visit with their families.
These disparate topics share a common theme. In each case, individual people taking care of patients noticed something—a trend, a need—and acted on it in a grassroots way to improve care. Individuals identified and helped address so many inequities that had always existed but became vividly apparent as COVID surged. Throughout the pandemic response, it became clear to me how powerful individual observations and a PDSA mindset can be in effecting change. If a centuries-old institution can pivot to address COVID-19—as it had for the 1918 flu and the polio epidemics of the 1940s and 1950s—then by coming together and addressing head-on inequities and urgent clinical needs, imagine what else we can accomplish.
“Working as a contact tracer illustrated what I didn’t learn in school: how understaffed and underresourced health departments are. They are charged with our nation’s most important task—keeping residents safe and healthy every day—but many are equipped with less than one full-time professional to do so.” —Claire McGlave, MPH ’20
LISTENING, PROVIDING COMPANIONSHIP, SOLVING PROBLEMS
Claire McGlave, MPH ’20
The field of public health has recognized health dispari-ties as a paramount issue for decades. The coronavirus pandemic has forced the rest of the world to pay attention. My experience as a contact tracer for the MA COVID-19 Academic Public Health Volunteer Corps brought home to me these disparities and taught me more about public health than I had learned in school. We mobilized 700 students in just two weeks to help local boards of public health with their pandemic response efforts, especially contact tracing.
Contact tracing is an essential part of a pandemic response. It is part public health work, part education, part social work, and part just plain talking to people. Maybe that combination is what public health is at its heart: a multidisciplinary practice of keeping people healthy and informed. This practice requires diverse skills, ranging from a deep understanding of the community to appropriate and accessible methods of education.
My time as a contact tracer in Boston demonstrated the intimidating reality of getting sick, and how unprepared we were—and still are—to respond to this public health crisis. I spoke with a woman who took her husband to the hospital because he had a fever, which resulted in an unexpected three-week isolation and hospital stay. Produce packers reported returning to work after testing positive for COVID-19 because their jobs—and in turn, their families—depended on it. I talked to abuelitas (grandmothers) who had been alone for three weeks, who would spend hours telling me about each of their grandchildren. I spent an evening on the phone with a woman figuring out how she could get diapers delivered for her children.
This job is social: It’s listening, keeping people company, and problem solving through an impossibly scary time. I am proud to be part of a group of volunteers who could effectively deliver these services because we live in the communities we serve. Our intimate knowledge of our communities enabled us to surmount crucial roadblocks, such as people’s lack of internet or the inability to successfully isolate in a crowded home.
A few weeks after I started working as a contact tracer, I tested positive for COVID-19. I did not experience any symptoms, and I have the immense privilege of being able to work from home. Despite taking a multitude of precautions, I contracted the virus. What scared me most was how easily I could have gone around shedding virus, with no idea I was doing so. This realization motivated me to clearly communicate the seriousness of COVID-19, because many people don’t feel the direct effects and are therefore not motivated to take precautions.
Working as a contact tracer illustrated what I didn’t learn in school: how understaffed and underresourced health departments are. They are charged with our nation’s most important task—keeping residents safe and healthy every day—but many are equipped with less than one full-time professional to do so. The health disparities that threaten our communities are reflected in health department capacity, because their funding comes primarily from property taxes. This means that the municipalities with the most serious public health needs (often lower-income cities and towns) have the fewest resources to respond to the pandemic.
Our public health system—which purportedly maintains healthy environments for everyone—requires revamping and redistribution. If we do not take this cause seriously, despite all the progress and innovation in our country, we will not be able to guarantee access to the quality of life that every human deserves. As we continue to address this pandemic, it is our responsibility as public health professionals to both create and advocate for work that moves us toward equitable access to good health and well-being. Try having conversations with an abuelita about missing her granddaughter’s first words, or not being allowed to care for loved ones who are ill. You’ll think the same thing.
SEEING THE PANDEMIC THROUGH A HUMANITARIAN LENS
Jessica Schiff, SM ’21
I first heard of the new coronavirus when I was in Lebanon for a humanitarian negotiations Wintersession course in early January. When I came down for breakfast one morning, the international news was reporting multiple cases of a new pneumonia-like illness in China. At the time, I thought nothing of it. I didn’t comprehend that the coronavirus would be a worldwide catastrophe until a few weeks later, when the virus continued to spread and countries were shutting down. Even after the World Health Organization declared COVID-19 a pandemic, I struggled to understand the gravity of the situation until I saw things in Boston being impacted.
COVID-19 provided a firsthand opportunity to apply the skills I have learned in my first year of graduate school. My research project to evaluate climate change implications on humanitarian programming was reworked within days to focus on the humanitarian response to the COVID-19. We shifted our research question to understand how humanitarian organizations used strategic public health methods in their response plans. Working on this project highlighted a nuanced issue that I hadn’t thought about when considering public health strategies: Public health measures could result in deviations from the international human rights framework, which in turn have public health implications.
For example, the public health policies and measures implemented to protect population health during COVID-19, such as closing international borders, restricting movement, and restricting humanitarian access, can violate basic human and refugee rights to security and safety and the right to seek asylum in other countries. Some states do not want to provide COVID-19-related care for refugee populations, because they do not see it as their responsibility. But the exclusion of entire populations of people can have potentially disastrous public health consequences.
I also knew that I wanted to help my local community. When Massachusetts Governor Charlie Baker announced the formation of the MA COVID-19 Academic Public Health Volunteer Corps, I immediately signed up to volunteer. I was placed on a team to assist with contact tracing for Taunton, Massachusetts, in collaboration with the local board of public health. Individuals I contacted were not always open to sharing critical information, which made my job as a volunteer more difficult. Some didn’t feel it was their place to share information about their contacts and had concerns about privacy; others did not trust me when I said I was volunteering with the state. Yet there were others who were very open and shared every detail and contact they had.
I remember speaking with a person who had been battling COVID-19 for weeks, with symptoms that waxed and waned and resulted in health complications. Listening to that person—who was young, like myself—recount their experience reminded me that the virus carried the potential for severe consequences, and that the façade of protection I felt from being young and healthy was just that: a façade. No one is truly protected from COVID-19, and the conversation helped reinforce the importance of wearing a mask and practicing social distancing. The volunteering experience opened my eyes to the various perspectives people hold regarding COVID-19, personal privacy, and public health, but it also helped me realize that most people were willing to put aside their concerns if it meant helping curb the spread of COVID-19.
From Burned-Out Nurse to Passionate Public Health Advocate
Katie Klatt, MPH ’21
I am a nurse, but at some point I realized that I didn’t want to be one anymore. In fact, that’s why I came to the Harvard Chan School—to change my career path. I felt ready to take a step in making a larger-scale impact, to move out of patient care and into the world of management. When the pandemic hit, it meant a lot of undesirable implications for me: an urgent demand for nurses and imposed isolation of an extrovert. Then I myself contracted COVID-19. I had just moved to Boston for school and felt very alone and very confined in my tiny room. For a hot second, I wanted to wallow in misery, be sick, ignore classes, and just be sad.
During those moments of self-pity, it was hard to remember all of the people who had it worse than me—those who have lost jobs, been hospitalized, lost loved ones. Empathy wasn’t easy, as the world felt like it was crashing around me. But as I sat in my room for days on end, I had a lot of time with myself—highly unusual for me. And the strangest thing happened. The more intimate I became with myself, the more I realized that I have a natural tendency towards joy. I couldn’t sit in sadness for very long without my mind automatically filtering it with a lightness and general delight—which is a strange thing to say as I sat alone in my room for two weeks with a 103-degree fever.
This magical realization about myself ultimately led to another that we all probably know: Joy is infectious. As I started to recover and join the growing crowd of lucky ones who survived, I realized that this innate energy I have could be used in a productive way. I thought I had left nursing behind, but my nursing skills provided an avenue to bring my energy to help others in a tangible way, to connect to the cause. Once I was cleared of the virus, I found myself in the middle of the semester on the infection-control team as a nurse at Boston Emergency Medical Services.
This experience revived in me the empathy I thought I had lost from the severe nursing burnout I had experienced even before the pandemic hit. I’m thankful that I now have the opportunity to both share my own story and connect with others in their own dark hours, whether as health care workers or COVID-19 patients. My new role provides a glimpse into the actions of selfless people, like an emergency medical technician (EMT) who rushed into a situation sans-PPE (personal protective equipment) because they mistook a radio call as a coworker in distress. But it is also a reminder that you never really know the hard decisions people have to face, like EMTs who cannot isolate from vulnerable family members in a large household.
It has become obvious to me by witnessing the hardships faced during the pandemic that COVID-19 is fundamentally intertwined with the greater outcry of humanity around the country and around the world. The year 2020 has provided no shortage of events that highlight the stark inequalities in our systems, from the pandemic to the Black Lives Matter movement. I’m starting to see that as I work to remedy my own ignorance, my public health responsibility might be to use my newfound energy to educate myself and others on the power structures that reinforce racism—the very same structures responsible for the inequities of COVID-19. The public is finally coming around to what we have known all along: Public health matters.
In a small way, I used COVID-19 to change my own life narrative. I now see the uncertainty that was ushered in by COVID-19 as an opportunity for change. Personally, I can see myself getting involved in creating new ways for public health to take a seat at the table and have a voice in higher-level decision making. On a larger scale, as public health professionals, we all have the responsibility to use this inflection point to spread the public health principles that are fundamental to our world and advocate for equity, human dignity, and safety as central pillars of any organization or activity. COVID-19 has given public health a new platform. Now we must use it.
HEEDING THE CALL TO ACTION
Ta-wei Lin, DrPH ’21
My wife and I were in Taiwan when the first case of COVID-19 was confirmed on the island in January. At that time, the number of individuals infected by the novel coronavirus in China had just passed 500, and countries across the globe began reporting their first cases. l felt that the possibility that this would become a global pandemic was remote. Fast forward to the end of September: The number of confirmed cases of COVID-19 has approached 30 million worldwide, including some 7 million here in the U.S.
The reality of COVID-19 did not personally affect me until this past March, when the decision was made to close Harvard campuses. It was around that time that the virus claimed its first life in Massachusetts. I felt a growing urge to put my public health training to use. This is when I was introduced to the MA COVID-19 Academic Public Health Volunteer Corps.
The corps is a collaborative partnership between the Massachusetts Department of Public Health and academic institutions across the state, with the goal of bridging the gap between public health academia and practice. Its primary focus is to provide support to local public health departments, many of which lack the resources to mount an effective pandemic response. With the help of leadership from doctor of public health candidates Cris Alonso, DrPH ’21, and Eric Cole, DrPH ’20, the volunteer corps deployed 777 public health students and professionals to local health departments across Massachusetts. In April and May alone, these volunteers provided 6,430 hours of service in the form of contact tracing, case management, communications, translation, data analysis, GIS mapping, and other public health services.
I remember the first phone conversation that I had with the local health department of a large city. We spoke with the deputy director of finance, who had no medical or public health experience whatsoever but was called in to play a key role in organizing the public health response. The medical team was composed of just two public health nurses and a rotating team of school nurses making phone calls around the clock to try to keep up with the rapidly rising number of confirmed cases and their close contacts. I remember them saying, “We’ll take all the help we can get.” Local health departments are tasked with incredibly important duties to promote and protect the health of their communities but are rarely provided sufficient resources to meet them. I was glad that we were there to help fill that gap.
My experience as an Academic Public Health Volunteer Corps team leader has reinforced three key lessons. First, that practice is the purpose of public health, a call to action that FXB Center for Health and Human Rights Director Mary Bassett and other public health leaders have made to bridge the divide between academia and public health practice. For students and researchers, this is often easy to forget.
Second, public health is local, even in the midst of a global pandemic. Each local health department that we worked with had its own set of circumstances and challenges. Statewide and national public health responses must be able to understand and address the unique needs at the local level in order to be effective.
Third, the longstanding structures of systemic racism continue to place a disproportionate burden of disease and poor health on communities of color. COVID-19 is no exception, with Hispanic or Latino residents of Massachusetts accounting for over 22 percent of confirmed cases while making up only 12.4 percent of the population. In our work advancing public health and health equity, we must play a more vocal role in dismantling systems of oppression that harm us all.
I am proud of the work that Academic Public Health Volunteer Corps continues to do to for our local communities. It has played a vital role in our statewide response to COVID-19 and serves as an important reminder that collectively we can make a difference.
A SECOND FULL-TIME JOB
Maryam Khalid, DrPH ’20
This spring I was working with Ariadne Lab’s Primary Health Care team, and the day of our team retreat at Brigham and Women’s Hospital, 60 ambulances were rushed to the hospital from the local Biogen Conference. This was the start of Massachusetts’ COVID-19 outbreak. A few weeks prior, I had attended talks at the Harvard Chan School on COVID-19 when it was still an epidemic, and chatter at work indicated it was just a matter of time before the United States would be hit.
I was consumed by the news and following COVID-19 cases. In March, when the disease began to exponentially spread in Massachusetts, my DrPH colleagues and I met (virtually). We wanted to make an impact and put our training to use. While our place in the system was not as clear-cut as that of our physician counterparts, we knew there were ways we could fill major gaps. Fourteen schools and programs of public health came together with the Massachusetts Department of Public Health to form an Academic Health Department Consortium (AHD), with the goal of bridging practice-based governmental and academic public health. At the request of Governor Baker and the COVID-19 Command Center, the consortium called on the academic community to support local boards of health in their pandemic response.
Two of my peers, Eric Coles, DrPH ’20, and Cris Alonso, DrPH ’21, began to spearhead the initiative’s student volunteer response, and within a week we had roughly 2,000 volunteers. They worked in the background with the consortium; with Harvard Medical School’s IT team, which created a contact-tracing system that fed directly into the state’s reporting system; and with 20-plus Harvard Chan DrPH students and alumni who served as team leads.
As a team lead, I oversaw 16 students, ranging from PhD to master’s levels to those in community health worker programs, who supported towns and cities with their COVID-19 response. Volunteers completed two state trainings on Massachusetts’ health system and emergency preparedness, and for REDCAP, the contact-tracing software. I had kick-off calls with public health nurses in the towns I was supporting, conducting a rapid needs assessment to determine the priorities, the number of support staff, and language requirements. I vividly remember the first phone call I had with a public health nurse, her voice exhausted from working for a week nonstop as her city’s only responder, and the immense gratitude she expressed for the additional support. I quickly onboarded my team, who were extremely eager to put their public health prowess to use in any way during the pandemic, and ended up contributing 400 hours during the first month of the response.
At the time, I was working a full-time job and collecting data for my dissertation, so the volunteer efforts became a second full-time job. Pandemic response was stressful, and as part of our rapid response, I was fielding multiple phone calls a day with team members and the public health nurse. Working as a team lead also afforded me the opportunity to work outside of the Harvard bubble and with many students with whom I might not have collaborated otherwise. I had never had the opportunity to work with community health workers domestically before, and they were absolutely crucial to our response, because they were the most tapped into Spanish-speaking communities. Our efforts were primarily in contact tracing, case management, and wellness checks, but also in supporting the local boards of health in public communications, incidence mapping, and translation.
My team’s most significant task was contact tracing. It was often not straightforward and required multiple follow-ups and subsequent hours of calls to find our way to any contacts. Social determinants of health were front and center during these contact-tracing calls. There was a lot of fear—fear of the unknown as it pertained to the virus and fear it would affect employment. Many people we called were essential workers who could not quarantine, others were single mothers unable to isolate, some were part of large families living in tight quarters, and some had concerns that their immigration status would come into question. Contact tracing required a lot of persistence. Human contact with the team included more than health surveillance and data collection, and it was a way for patients to build rapport with someone who could help them navigate the uncertainty.
As graduate students, we rapidly mobilized and served as a tourniquet for the state’s response until a more formal contact-tracing infrastructure was ready. In most towns there was only one public health nurse, and we were able to fill the void by providing teams of students to support the nurses. When the state prepared to come out of quarantine, our work evolved into supporting towns with their reopening plans. As DrPH students, we shared lessons learned from each of the towns that we were supporting, as well as materials that we created in multiple languages, rallying together to support varying local needs. There couldn’t have been a more critical time to rise to the occasion.
“Our bottomless desire for numbers can only be satisfied by something wholly different: not by counting how much and how long, but by telling what, why, who. Stories are what will remain, long after the pandemic has ended.” —Stephen M. Kissler, postdoctoral fellow
COUNTING
Stephen M. Kissler, Postdoctoral Fellow
There’s a great secret they won’t tell you until you’ve studied math for years: There are gaps between the things you can count. But mathematics is the study of things that can be counted and measured, so we place these curiosities to one side, where they remain, casting pale and uneasy shadows.
We are a culture that counts things, even more in the past few months than ever before. My phone alerts me: 228 new cases today. I step outside: maintain six feet of distance, and stay no more than 15 minutes. They say the risk of dying is 0.9 percent—or is it more, or less? And I’m 29, so that adjusts it a bit—but my grandmother is my reciprocal, 92, and I’m at once sad and relieved that she lives on a farm 2,014 miles away and not here in a city of 694,583 anxious people.
I am a mathematician, so I count things. Some things I have counted recently include: the number of months until the second wave begins and the number of people who could be hospitalized; the size of the outbreak in New York City and the difference in the number of cases between the rich and the poor. God, it’s big.
We count to understand, yes, but beneath that, we count to dispel anxiety and fear. We count to prepare. It works, most of the time. A thing that can be counted can be managed; it’s like wrapping the arms of our mind around some great object and finding that our fingertips just touch on the other side.
But for an epidemiologist, counting is different. The units are lives. Assigning a number to such a thing does a violent disservice. We count anyway, because we must; because if we count well enough, more people will stay healthy, more will survive.
Still, the uncountable things demand to be heard. I spend my days counting, but at night the specters arise in my dreams. Each “1” contains a little infinity, something measureless and unrepeatable. I wake, gasping for air.
I once asked a respected professor how she thinks about infinity. It’s not really a thing, she said, but a state of being; it’s an overflowing glass, it’s what happens when you’ve reached the edge of what you can imagine and then keep going. It’s where divisions cease and the concrete and the immaterial embrace. It’s what makes the real intelligible.
That’s what infinity is, she said. That’s what’s hiding there in the gaps. Our bottomless desire for numbers can only be satisfied by something wholly different: not by counting how much and how long, but by telling what, why, who. Stories are what will remain, long after the pandemic has ended.Tell them.
Tell them poorly, tell them well. Our lives depend on numbers, but our souls depend on stories, and now more than ever, we all have one to tell.
—Edited by Madeline Drexler


