Obesity alters molecular architecture of liver cells; repairing structure reverses metabolic disease
For immediate release: Wednesday, March 9, 2022
Boston, MA – Cells use their molecular architecture to regulate their metabolic functions, and repairing diseased cells’ architecture to a healthier state can also repair metabolism, according to a study led by Harvard T.H. Chan School of Public Health researchers.
“Chronic metabolic disease, which includes obesity, diabetes, and cardiovascular and liver diseases, is the biggest global public health problem,” said Gökhan Hotamışlıgil, James Stevens Simmons Professor of Genetics and Metabolism at Harvard Chan School and the director of the Sabri Ülker Center for Nutrient, Genetic, and Metabolic Research. “The fundamental regulatory mechanism that we discovered can be used to evaluate the susceptibility—or resistance—of individuals to a disease state like obesity, and determine what steps, such as diet, nutrients, or fasting, will reduce, eliminate, or exacerbate these states. We can imagine a whole new array of therapeutic strategies targeting molecular architecture, similar to the restoration of an ailing building or preventing its deterioration.”
The study was published online on March 9, 2022, in Nature.
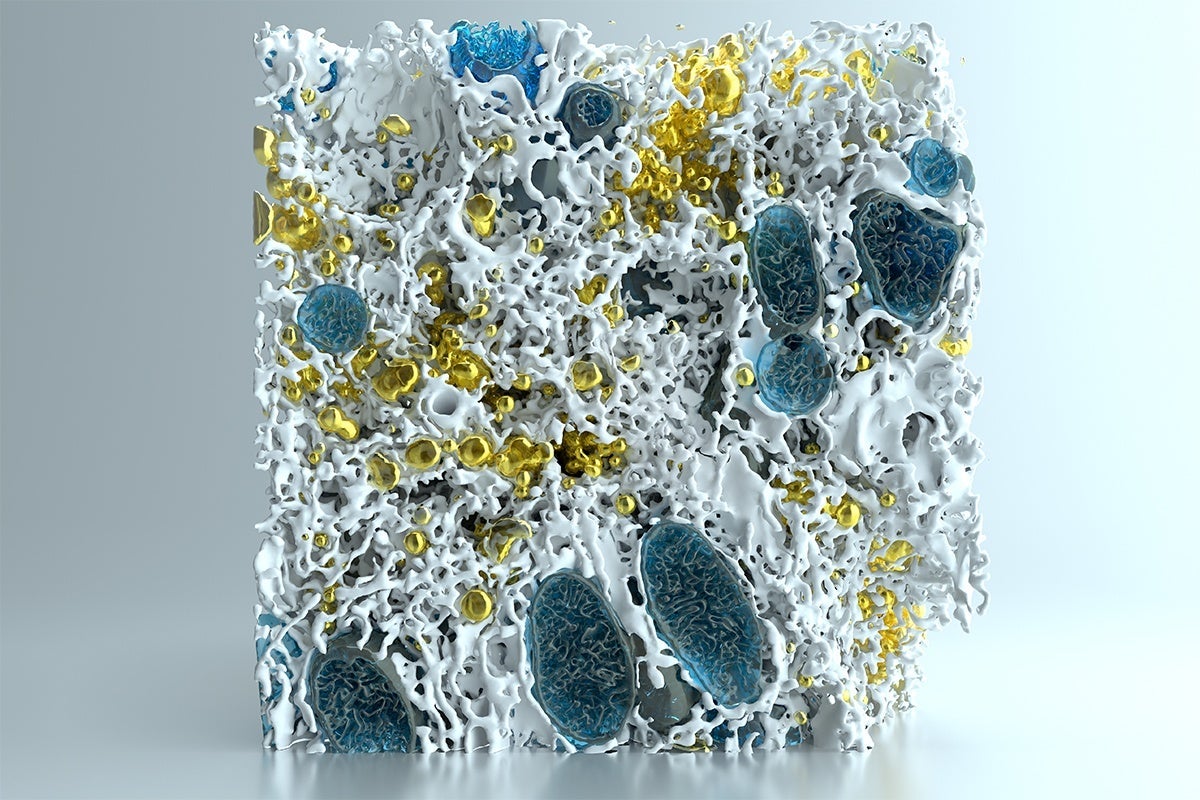
Led by researchers Güneş Parlakgül and Ana Paula Arruda at the Sabri Ülker Center, the study compared liver samples from healthy, lean mice with samples from obese mice with fatty liver disease. Using multiple computational platforms—artificial intelligence, machine learning, deep learning, and neural networks—and high-resolution imaging using enhanced focused ion beam scanning electron microscopy, Parlakgül, Arruda, and colleagues from the Howard Hughes Medical Institute generated three-dimensional reconstructions of specialized structures, called organelles, inside cells and made a comparative analysis of organelle architecture and organization of liver cells from lean and obese samples. Through these analyses, the team determined that obesity leads to dramatic alterations in subcellular molecular architecture, particularly in the endoplasmic reticulum (ER), an organelle involved in the creation and shaping of proteins and lipids.
The team then partially restored the ER’s structure using technologies that can repair molecules and proteins that can reshape cellular membranes—which also repaired the cells’ metabolism. The restored cells looked normal, controlled lipid and glucose metabolism much better, and remained stress free and more responsive to stimuli.
“The outcome was really striking—when structure is repaired, so is the cell’s metabolism,” said Arruda. “What we are describing here is a whole new way of controlling metabolism by regulating molecular architecture, which is critical for health and disease.”
The images produced from this research are also the most detailed visualization to date of subcellular structures while the cells are still intact in their tissue environment. Other researchers have created similar imaging before, but mostly in single cells or in culture.
“High-resolution imaging and deep-learning-based analysis helped us to see that structural regulation of intracellular environment and organelle architecture is a key component of metabolic adaptation. Targeting this regulation may hold therapeutic opportunities to treat metabolic diseases such as diabetes and fatty liver disease,” said Parlakgül.
For Hotamışlıgil, the visuals are astonishing. “I was first mesmerized with the complexity, beauty, and harmony of the constructions in the extremely crowded internal space of a cell,” he said. “This is like watching an artistic masterpiece while traveling into the center of a cell.”
This research was supported by the Sabri Ülker Center at Harvard Chan School.
Other Harvard Chan School researchers involved in this research included Erika Cagampan, Nina Min, Ekin Güney, Grace Yankun Lee, and Karen Inouye.
“Regulation of liver subcellular architecture controls metabolic homeostasis,” Güneş Parlakgül, Ana Paula Arruda, Song Pang, Erika Cagampan, Nina Min, Ekin Güney, Grace Yankun Lee, Karen Inouye, Harald F. Hess, C. Shan Xu, and Gökhan S. Hotamışlıgil, Nature, March 9,2022, doi: 10.1038/s41586-022-04488-5
Image: Gökhan Hotamışlıgil/Sabri Ülker Center for Nutrient, Genetic, and Metabolic Research and Refik Anadol, Refik Anadol Studios, LA
Visit the Harvard Chan School website for the latest news, press releases, and multimedia offerings.
###
Harvard T.H. Chan School of Public Health brings together dedicated experts from many disciplines to educate new generations of global health leaders and produce powerful ideas that improve the lives and health of people everywhere. As a community of leading scientists, educators, and students, we work together to take innovative ideas from the laboratory to people’s lives—not only making scientific breakthroughs, but also working to change individual behaviors, public policies, and health care practices. Each year, more than 400 faculty members at Harvard Chan School teach 1,000-plus full-time students from around the world and train thousands more through online and executive education courses. Founded in 1913 as the Harvard-MIT School of Health Officers, the School is recognized as America’s oldest professional training program in public health.