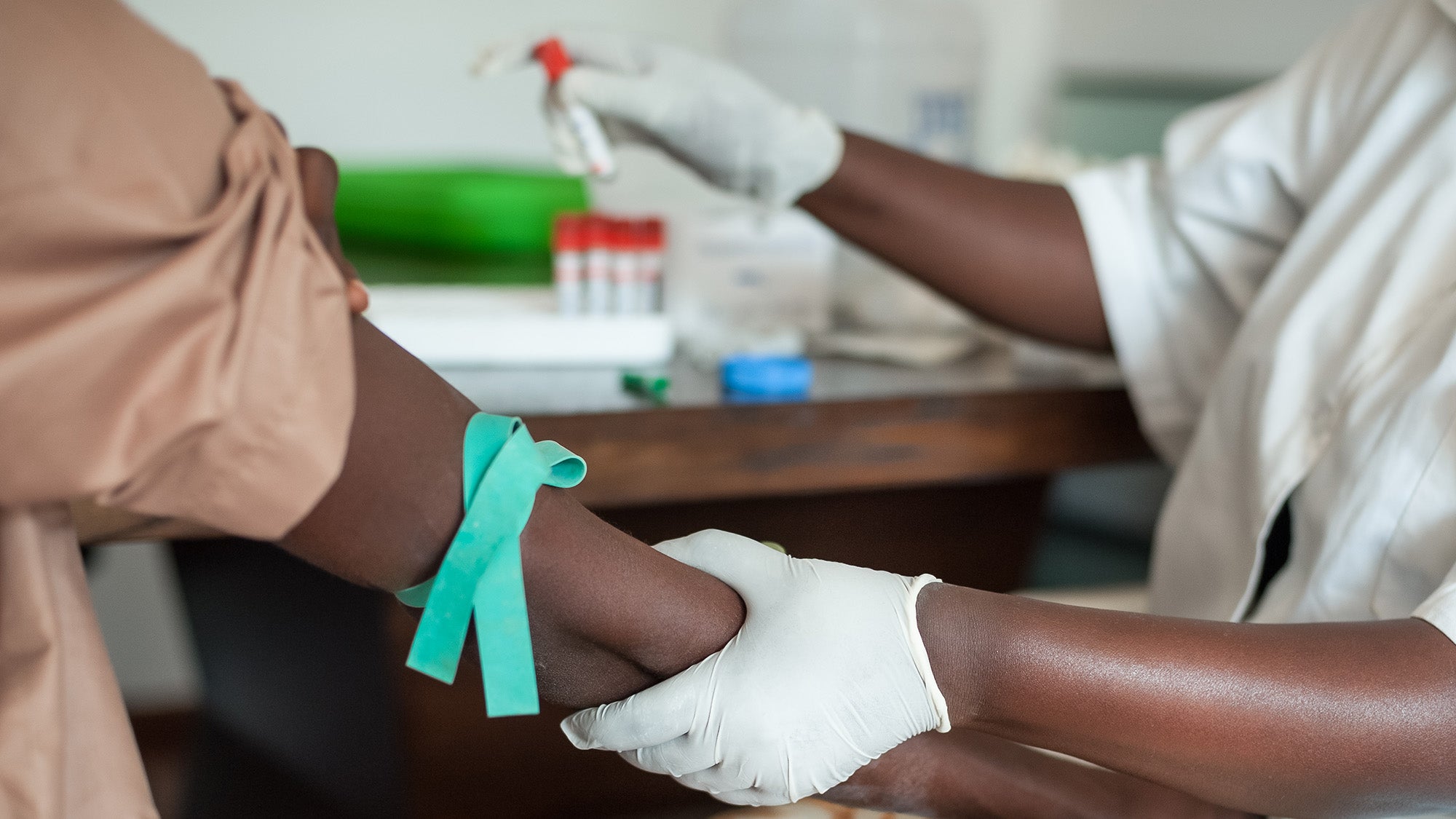
Researching chronic disease in the aftermath of a hurricane

One year after Hurricane Maria devastated Puerto Rico, a large observational study will document the development of cardiovascular and other chronic diseases among the island’s adult population.
When compared to the general U.S. population and residents of other Hispanic/Latino heritage, multiple studies have found that Puerto Ricans living in the mainland U.S. have a high prevalence of chronic conditions and related risk factors. However, far less is known about the health-related behaviors and disease state of those living in the U.S. Commonwealth of Puerto Rico.
“Chronic diseases are the top causes of death in Puerto Rico, led by heart conditions, cancer, and diabetes,” says Josiemer Mattei, assistant professor in the Department of Nutrition at the Harvard T.H. Chan School of Public Health. “There is still much to learn about the factors that contribute to these chronic diseases, both negative as well as protective, and that are distinctive to the population of Puerto Rico.”
Dr. Mattei has already begun to explore this research question. In 2015, she and her team documented the lifestyle and health characteristics of nearly 400 adults living in Puerto Rico, finding a high prevalence of cardiometabolic and psychological conditions, including hypertension, obesity, diabetes, anxiety, and depression. However, their primary goal was to inform future research efforts to improve the population’s health. After addressing challenges and identifying what worked best, the pilot study concluded that epidemiological studies in Puerto Rico are feasible and indispensable.
Then, on September 20, 2017, Hurricane Maria hit Puerto Rico with rain and wind gusts peaking at 155 miles per hour—causing landslides and flooding that wiped away neighborhoods and knocked out essential infrastructure. The media and public health initiatives have focused on the mortality count, which has been estimated at nearly 3,000. Yet, the consequences for disease and health behaviors post-Maria have not been recorded.
“Puerto Rico lacked comprehensive studies that tracked chronic disease risk factors at the whole population level, and this need intensified in the wake of devastation left by Maria,” says Dr. Mattei. “There is urgency for studying trends in lifestyle behaviors, psychological factors, and chronic conditions after times of distress. This new understanding can help us prioritize strategies to prevent these conditions and improve the population’s health.”
That’s why Dr. Mattei and collaborators from FDI Clinical Research of Puerto Rico and University of Massachusetts-Lowell are launching the Puerto Rico Observational Study of Psychosocial, Environmental, and Chronic disease Trends (PROSPECT), an island-wide research initiative funded by the National Heart, Lung, and Blood Institute, that will recruit two thousand adults and track their health at the start of the study and two years later. To do this, researchers will gather a range of data from participants, including multiple dietary and psychosocial factors (such as stress and social support), biological markers for cardiovascular disease, and medical records. PROSPECT will also assess whether risk factors for chronic disease differ between urban and rural residents.
The long-term goals of PROSPECT are multifaceted. Ultimately, findings from PROSPECT will inform tailored public health programs and interventions to more effectively improve health in this high-risk, underserved population—especially following a natural disaster. The study will also create the framework for a representative island-wide sample, establish a biorepository and participant database for future use, and continue to yield seminal trend data.
Furthermore, the collaborative approach of PROSPECT is also designed to enhance leadership and research capacity in Puerto Rico. A complementary study was recently awarded to the research team in collaboration with University of Puerto Rico investigators to assess food and water shortages and social connectedness after Hurricane Maria, and how these triggered physiological stress responses (i.e., allostatic load). The study is funded by the National Institute on Minority Health and Health Disparities.
José F. Rodríguez-Orengo, Executive Director of FDI Clinical Research and PROSPECT co-investigator agrees that the work will bring significant and needed results to advance public health policy in Puerto Rico. “Hurricane Maria revealed many vulnerabilities in the health and food systems of Puerto Rico,” says Dr. Rodríguez-Orengo. “But our studies will help show the positive aspects that could strengthen such systems in case of another disaster.”
Additional collaborators of the projects include the Puerto Rico Primary Care Association Network, Hospital del Maestro, HIMA system, College of Nutritionists and Dietitians of Puerto Rico, Institute of Statistics of Puerto Rico, Centers for Disease Control and Prevention Dengue Branch, Toledo Laboratories, Puerto Rico Science, Technology and Research Trust, Albert Einstein College of Medicine, University of Massachusetts Amherst, and the Harvard Humanitarian Initiative.
Photo: Andrea Booher